Hospital CFOs concerned about service lines; some embrace coming disruption
Haven Health may have withered on the vine. Google Health may have been broken up. But a disruption of healthcare’s business model still is likely coming, and the actions hospital CFOs take now to prepare for the coming changes will play a major role in how well the industry fares.
A survey of 141 healthcare finance leaders, conducted for HFMA’s four-part special series “Healthcare 2030,” tells the story of an industry fearful of possible changes by disrupters that could make life difficult for hospitals that don’t reinvent themselves. Disrupters could threaten service lines, damage hard-earned reputations and potentially threaten the very existence of some operations.
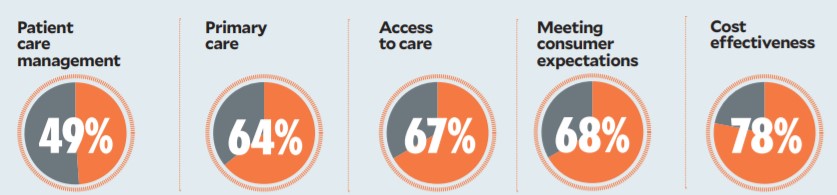
In the survey, respondents were asked to rate five areas on a 5-point scale based on vulnerability to disruption, 1 being not vulnerable and 5 being very vulnerable. Responses showed CFOs believed four of the five areas leaned toward being vulnerable to disruption, with cost effectiveness being most vulnerable. The category had more than 78% of respondents rating it as a 4 or 5 in their responses.

But for CFOs who aren’t caught flat-footed, a disruption may present an opportunity. Tatyana Popkova, chief strategy officer for Chicago-based Rush University System for Health, doesn’t view Amazon or other disrupters as a threat.
“When I look at Amazon, I think, ‘How can we partner with them and complement each other?’” Popkova (pictured) said in an interview to be published in Part 3 of the “Healthcare 2030” series, coming in November. “For us to be a regional partner for one or several of these companies would be a terrific opportunity. This is a very real possibility.”
Of course, innovation is going to be central to hospitals maintaining their operational and financial footing, even if it means changing their fundamental business model. “The most promising innovations are the ones that will keep patients out of the hospitals,” one respondent wrote in the survey. “That may be somewhat incongruent with long-term financial viability of some hospital services. Those innovations that provide health information to patients so they can act before needing to be hospitalized.”
Already, the COVID-19 pandemic has been the driver of the switch to being more accepting of telehealth care, and of so-called digital front doors, which are online systems for guiding patients through their care. “Before COVID, digital front door and telehealth were differentiators for a lot of us,” Popkova said. “Now, though, it’s an expectation. We’re past the point of no return.”
Another challenge identified in the survey concerned workforce and management. When CFOs were asked about which types of workers will be the most difficult to find, nurses and other clinicians (not including physicians) were cited as likely being harder to find in the future by 94% of respondents. The second-ranked category, data/information technology, was described as harder to find by 63% of respondents, followed by physicians/advanced practice providers (60%), finance/revenue cycle (50%), facilities management (34%) and executive management (32%).
Other positions could prove even more challenging. Another respondent said, “We are struggling to find bedside staff and support staff …. [there are] no applicants to train.”
Many respondents say more education and training is in the cards. One of them wrote, “Given the baby boom nurses retiring, the number of experienced nurses available will significantly decrease and we will need a training program to get [new nurses] to an experience/competency that other clinicians are used to.”
Progress with DEI?
But efforts to improve diversity, equity and inclusion (DEI) may finally begin to bear fruit, with many respondents describing detailed plans to do so. “We have extensive efforts to increase diversity across the entire organization. In the CFO division, we have a formalized mentoring program and team that keeps diversity tactics on the front burner,” wrote one respondent.
And another wrote: “We have created a DEI committee that reports to our [board of directors] charged with developing mission and vision statements around DEI. This will be far-reaching to include workforce recruitment, patient recruitment, services offered and further developing our public posture.”
When it comes to demand for executive management, no clear consensus could be drawn from the results of the question, “Do you anticipate a structure with fewer executive leaders by 2030?” Forty-seven percent said, “Yes,” and 53% said, “No.”
In comments accompanying their negative responses, survey participants often said they are overworked or anticipate continued regulatory red tape. “All the increased regulations and having to deal with managed care insurance plans that find all kinds of new reasons to deny claims has really increased the burdensome tasks that executive leaders have to deal with,” wrote one respondent.
At the same time, others think consolidation and improved operations will reduce demand for managers, including a respondent who said they “expect that as we move decision-making down, and through efficiency and automation,” fewer executives will be needed.
Preparing for more outpatient care
Another serious trend hospitals are expected to face is the continued transition to outpatient care, managing where care should be provided and the type of care to provide. One respondent described what hospitals should be doing, given the industry’s complicated needs and interrelationships:
- Expanding permanent virtual health tools across all areas
- Reducing physical footprints to critical services while focusing on the higher-acuity care services that will always require hospital intervention and care (such as for the aging population with higher-end service needs)
- Balancing out the right mix of virtual and physical visits for outlying clinics
More generally, Rush’s Popkova suggests being receptive to new ways of doing things. “We need comfort with ambiguity, and we need to be open to innovation,” she said. “We need to experiment with business models and take risks. If we can continue the momentum we gained during COVID-19, we’ll be OK.”
Healthcare’s vulnerability to disruption
Percentage of 132 CFOs in an HFMA survey who rated the areas listed below a 4 or 5, based on a 5-point scale, with 5 being most vulnerable and 1 the least.