David Johnson: Efforts to revitalize healthcare on Chicago’s South Side underscore a critical national challenge
The United States continues to struggle with daunting inner-city health and healthcare problems borne out of innate social inequities. Effective solutions are few and far between. One initiative on Chicago’s South Side, launched just before the COVID-19 pandemic, encapsulates the potential and perils of system restructuring.
In that distant January of 2020, four Chicago safety-net hospitals almost pulled off a miracle. Mercy Hospital & Medical Center, St. Bernard Hospital, Advocate Trinity Hospital and South Shore Hospital overcame their parochial interests and tried to form a cohesive community health network for their South Side communities.a
This was a made-for-Hallmark movie moment wrapped within the cruel realities of inner-city healthcare. Hope and cynicism intermingled as proponents sought to redirect monies away from antiquated hospitals into more distributed, holistic and community-based care delivery.
The elephant-in-the-room question was whether the healthcare system could actually improve the lives of the South Side’s beleaguered residents. Even as the pandemic raged, the transformation plan gained momentum and widespread political backing for the $520 million in state funding required to cover implementation costs.
Then, with the funding bill on the cusp of passage, disaster struck: Worried about hospital closures and without specific knowledge regarding replacement investments, key South Side legislators withdrew their support on the last day of the legislative session that May.b The big transformation program died a quick death. A smaller transformation collaborative funded by the state of Illinois replaced it.c Mercy announced its intent to close two months later.d
Resurrecting and perhaps expanding on the original transformation plan may be Chicago’s best chance for improving lives and livelihoods on the South Side. In the process, this effort could become a model for revitalizing inner-city health and healthcare nationwide.
The fierce urgency of now
The need for healthcare transformation in Chicago’s disadvantaged neighborhoods is even greater today than it was in 2020. With many in these neighborhoods suffering from excessive chronic disease, COVID became a Grim Reaper. Limited access to healthcare services added to the death toll. The human costs of disfigured, disrupted and lost lives are incalculable.
In his book “The Emergency,” UChicago Medicine emergency department (ED) physician Thomas Fisher chronicles the “healing and heartbreak” of treating patients from the South Side during COVID’s intense first year. Readers can feel his seething anger and frustration in a fictitious letter he writes to a patient named Robert. Suffering from kidney disease, Robert celebrated his 25th birthday in the ER with a gunshot wound in his leg. The letter includes this remarkable passage: “Families on the South Side have less education, income, and wealth, which contributes to diminished access to goods, services, and legal protections. …. As a result, Black people, who densely populate the South Side, are forced to endure a gauntlet of health risks: jobs that maim, food that sickens, air that chokes and guns that kill.”
This would be a simple story of winners and losers, except there is no competition — not a fair one, at least. The contest was decided at birth, and this tournament trades in the most important of human endowments — our health.
A sad reality
Fisher’s anger has merit. The U.S. healthcare system has an unchecked tendency to be unfair, inequitable and uncaring. Healthcare disinvestment in highly segregated, low-income communities mirrors the broader societal disinvestment in these communities.
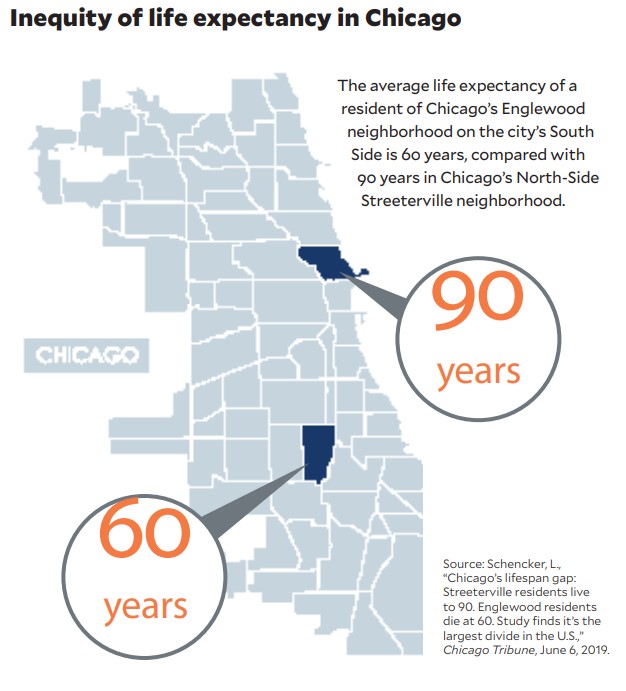
The impact of this structural disinvestment on individual and community well-being is catastrophic. The ambitions, productivity and health of those on the losing end of this high-stakes “tournament” wither. As a consequence, South Side residents live shorter, harsher lives. The difference in life expectancy between the impoverished Englewood and the affluent Streeterville neighborhood (just under 11 miles apart) is 30 years, the largest “death gap” in the country.e
Fighting against gravity to preserve an inadequate status quo, the State of Illinois spends hundreds of millions of dollars each year through complex funding arrangements to support safety-net hospitals. It’s wasteful and the equivalent of putting Band-Aids on open wounds.
As a nation, we already spend enough on healthcare. We need to spend the money we have more wisely. St. Bernard Hospital’s CEO, Charles Holland, said as much in January 2020 when he observed, “We recognize that it doesn’t make sense to keep pouring millions of dollars into aging, outmoded, out-of-date healthcare facilities.”
More of the same approach will yield more of these same dismal results. It’s time to think bigger and act differently. Incremental improvements aren’t enough. The system requires exponential, not incremental change. Post-COVID, America has a moral imperative to reimagine inner-city healthcare. Why not start on Chicago’s South Side?
Health over healthcare
Earlier this year, Chicago elected Democrat Brandon Johnson as its mayor. “Treatment Not Trauma” became his signature campaign issue and propelled him to victory in a close race. Mayor Johnson now faces the challenge of translating his campaign promises into policy.
The headline from Mayor Johnson’s first “Treatment Not Trauma” program was a modest $4.8 million allocation (out of a total $16.6 billion budget) to expand mental health services.f Imagine how much more “treatment” Chicago could provide by spending more safety-net monies on vital primary and preventive care services. This type of health-first investment would constitute a galvanizing paradigm shift.
The state of Illinois has enacted hospital assessment legislation to bring an additional $250 million in federal dollars to fund safety-net hospitals.g Generating this funding requires taxing all the state’s hospitals to gain access to federal matching funds that the state redistributes disproportionately to safety-net hospitals.
Most of this incremental funding goes to safety-net hospitals in lump-sum payments. This is problematic because federal regulations call for phasing out this type of non-claims-based payment to hospitals by 2027, thereby compromising Illinois’ ability to provide ongoing funding to prop up the shaky finances of its safety-net institutions.
Rather than patching-up antiquated facilities with low-quality scores to dispense uneven and fragmented care, Chicago and Illinois could align care provision with resident needs. That approach would promote expansive investments in pre- and post-natal care, chronic disease management, mental health and health promotion services. This policy shift would not only save money but also dramatically improve health outcomes.
As I mentioned previously, there’s already a good transformation plan on the books from 2020. With the exception of Mercy, the original organizations — St. Bernard Hospital, Advocate Trinity Hospital and South Shore Hospital — are still there. Put the band back together, dust off that plan, sharpen it up, invite others to participate and market it like the devil to South Side
residents,
Earning South Siders’ trust will be difficult. Win their support with deeds, not words. Build the new hospitals and aligned facilities before closing or repurposing existing institutions. Promise all existing employees’ jobs in the new community health network. Healthcare workers are in short supply. It makes sense to redeploy those already employed.
Don’t stop there. Recruit and train an army of people from the community to fill new positions as health coaches, nutritionists, physical therapists, aids and technicians. Celebrate the new approach to South Side health and wellbeing expansively. Create health champions within each South Side neighborhood.
This is what “Health over Healthcare” investment looks like. With this approach, there would be appropriate and sufficient healthcare facilities and services on Chicago’s South Side. Overall healthcare spending would decline. Individual and community health and well-being would improve. In the process, the City of Big Shoulders would lift up rather than push down its South Side residents.
Footnotes
a. Ihejirika, M., “4 South Side hospitals seek $1.1 billion merger, build one hospital,” Chicago Sun-Times, Jan. 23, 2020.
b. Goldberg, S., “Government funding to fuel South Side hospital merger falls through,” Crain’s Chicago Business, May 22, 2020.
c. Illinois.gov, “Healthcare transformation collaboratives,” Page accessed Nov. 22, 2023.
d. NBC Chicago, “Mercy Hospital announces closure after operating for nearly 170 years,” July 30, 2020.
e. Schencker, L., “Chicago’s lifespan gap: Streeterville residents live to 90. Englewood residents die at 60. Study finds it’s the largest divide in the U.S.,” Chicago Tribune, June 6, 2019.
f. Davis, K., “Johnson’s ‘Treatment Not Trauma’ plans start to take shape,” Crain’s Chicago Business, Oct. 16, 2023.
g. Illinois.gov, “Gov. Pritzker signs hospital assessment legislation bringing $250 million in additional federal funding for health care to Illinois,” press release, July 7, 2020.





