3 objectives for an innovative and practical revenue cycle work-from-home program
An effective revenue cycle work-from-home policy requires healthcare organizations have the means for tracking and measuring staff productivity and effectiveness.

Healthcare organizations are accustomed to dealing with change, and sometimes that change has been dramatic. But nothing could have prepared them for the recent COVID-19 distancing policies, where organizations have been forced to pivot from face-to-face interactions with staff to virtual communication, particularly around revenue cycle functions. All of a sudden in this environment, remote work is poised to become the new normal. And this outcome seems likely if remote-work policies can be fine-tuned so there is no loss in staff productivity or effectiveness.
Key work-from-home concerns
To develop a sustainable remote-work policy, it is necessary to address concerns about staff morale, team cohesion and protection of cash flow. Healthcare organizations usually take months, if not years, to make significant operational changes. Yet as a result of COVID-19, work-from-home solutions had to be deployed in a matter of weeks, thus challenging organizations’ abilities to manage the process effectively.
As a blended office environment becomes the predominant model across the industry, organizations will have to ask themselves: What techniques can we use to squeeze the maximum amount of cash from our current accounts receivable to help us ride out the drop in elective procedures and potentially develop a long-term remote employee strategy?
Work-from-home design
Not all work will be performed remotely. Some employees will desire to work from home, and their job requirements will fit nicely into that model. For example, coding assignments have been performed remotely for years. Other employees will work part-time from home and part-time in their current offices. Ideal candidates for this type of role are employees who work on account follow-up or claims billing. Some employees, however, will need to work full-time in the office due to their job requirements. Patient access employees, for example, need to be onsite to interact with patients.
The shift in workplace policy, and the new structures needed to achieve it, will require a different management mindset. Yet organizations that effectively adopt this new mindset will likely emerge healthier and more flexible in general.
Achieving a successful transition will require a focus on three objectives that reflect performance excellence:
- Productivity and effectiveness
- Staff morale and team cohesiveness
- Security of patients’ protected health information (PHI)
1. Productivity and effectiveness
Ensuring staff are productive and can work effectively in a work-from-home environment requires attention to both technology requirements and staff behavior.
Technology. To truly understand and improve performance, organizations must address fundamental technology issues. The first step, of course, is to build the remote-access environment. Most organizations have this capability, but it is often not fully deployed. To enable staff to effectively perform work remotely, technology must be configured and activated with the associated required job tools necessary to perform daily activities. For example, access to the host system, electronic billing system, shared drives and imaging systems — every application used daily by staff — will need to be made available to them remotely.
Staff performance. Organizations also should understand that the workforce might not have the discipline needed to initially work from home. It therefore is highly important that the organization have the ability to track what team members do and how well they do it. Organizations should be able to measure not only productivity, but also quality of work — that is, how well individuals perform their tasks in the work-from-home environment.
Analyzing what actions are taken throughout the day and how well those actions align with driving cash velocity is critical. Applying an action taken methodology can be an effective approach, where new actions are consistently added to whatever system the organization uses to monitor employee account activity.
With this approach, organizations should develop a comprehensive list of actions taken, where efforts are classified according to whether they involve “processing” or “resolution” actions.
Processing actions are the specific actions where activity occurs, but the action performed does not advance the account to final resolution. Examples include:
- Leaving a message with payer
- Sending emails requesting status
- Checking an online portal for claim status
Resolution actions are those that move the work activity on to the next most appropriate step to adjudicate. Examples here include:
- Correcting and resubmitting a claim
- Filing a clinical appeal
- Adding new insurance and billed claim
Staff also need to be trained to be more aggressive with their follow-up activities. All too often, the primary motive in working accounts for A/R follow-up staff is to get credit or to move on to the next account. If not managed appropriately, this motivation can cause staff to overlook the appropriate action needed to obtain resolution. Follow-up staff should instead have three goals: get credit, obtain resolution and move quickly to next account
Keeping performance monitoring simple is essential. If the monitoring system is set up correctly, managers should be able to assess in real time how productive and effective a staff member is compared with other staff doing similar tasks, thereby easily and accurately identifying high and low performers. Managers then can provide training opportunities that should help improve staff engagement, effectiveness and satisfaction.
Segmenting job duties is an important step in setting up work-from-home operations that can help facilitate comparisons of staff productivity and effectiveness. Having a comparative set of performance measurements across employees working in similar roles is critical. But just as important is consistency in defining similar job functions.
Thus, for example, the work of a biller should be compared with that of other billers, whereas the work of follow-up staff should be compared with the performance of others who perform such activities.
Furthermore, follow-up activities should be split into different groups dedicated to handling Medicare, Medicaid and commercial type accounts, respectively, because the pacing between the three groups is vastly different. For instance, staff working with Medicare accounts should be able to work several more accounts per day than those working with commercial accounts because the Medicare tools clearly detail the information needed to correct accounts for adjudication and online access enables claim corrections.
2. Staff morale and team cohesiveness
Working from home can be lonely in some instances and frustrating in others if family members are around to distract employees. Some individuals adapt to this situation quickly and enjoy the flexibility it provides — such as a two-minute commute, or the ability to not ‘dress’ for work. Others have a hard time making the adjustment and staying productive.
One technique that helps bolster morale is to publicize how individuals’ efforts contribute to the organization’s success. If staff can see how their work is having a positive effect for the facility, and is not just busy work, they will generally perform at a higher level. Being able to track and show their performance, while leveraging payment velocity data to show how much money staff members drive over the course of time is a significant way to show value.
Moreover, if tracking is consistent across teams, some groups have used gamification to keep staff engaged. Offering gift cards or other incentives to those who are the most productive each day or have the highest effectiveness score over a specific period also can be a positive engagement tool. Presenting these incentives to employees in virtual gatherings, such as a lunch Zoom meeting, can build morale by allowing everyone to see and hear their coworkers and feel part of the of community.
3. PHI security
Ensuring the security of PHI is a complex undertaking, with many facets, given the many ways in which PHI can be compromised. Article space constraints will not permit an in-depth discussion of all that is required to fully address this issue. A recommended practice is to use SSL [secure sockets layer] certificates on web pages intended to maintain PHI and leverage remote desktop technologies to require staff to credential themselves through the existing IT security protocols.[1] This approach ensures the only way remote users can access applications will be behind the organization’s firewall infrastructure.
Case example: Memorial Health System
Memorial Health System (MHS) in Marietta, Ohio, is a not-for-profit integrated health system employing more than 2,700 employees, including 325 providers representing 64 clinics. In recent months, beginning prior to the COVID-19 crisis, MHS initiated significant changes related to revenue cycle activities. Historically, MHS had a blend of remote workforce for both hospital and physician-based activities in its patient financial services area. As more work was increasingly shifted from on-site to remote at the onset of the pandemic, it became clear to MHS that measuring productivity and effectiveness posed a significant challenge.
In late January 2020, MHS leadership implemented a workflow solution to drive higher performance and understand staff activities. In six weeks, the MHS management team had visibility into individual performance, team outcomes and cash velocity. They were also able to track and identify issues with internal process breakdowns and variable payer processes that impeded MHS’s ability to maximize cash collections. The solution also enabled MHS to standardize the follow-up process across the payer sectors of Medicare, Medicaid and commercial payments. A/R staff also can communicate effectively with front-end staff to resolve issues without the traditional email communication getting lost or creating a “black hole.”
Once the processes were standardized and codified, the MHS team began to monitor and evaluate staff performance in new and meaningful ways. The graphic below provides an example of the type of sector reporting MHS uses to understand how efficiently accounts are being worked and how effective staff are performing, on average.
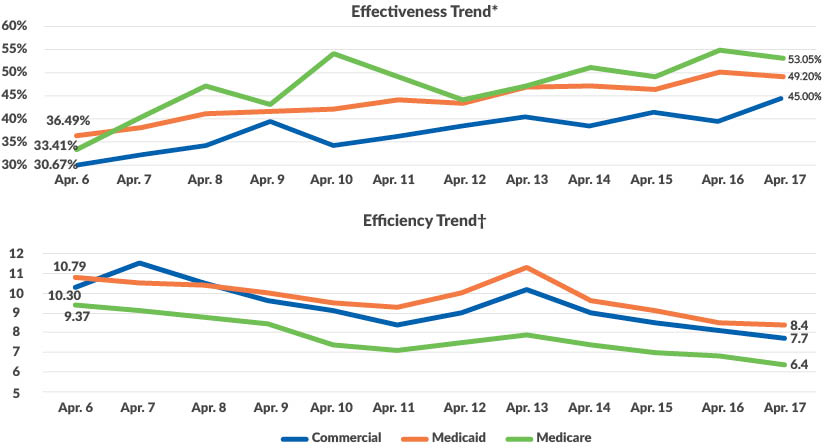
*Measured by % of resolution action
†Measure by average minutes between actions
Source: BakerTilly, 2020
48.72%
Overall effectiveness score
(Measured by % of resolution actions)
Effectiveness by sector
Commercial: 45.00%
Medicaid: 49.20%
Medicare: 53.05%
In the commercial sector, User 2 had the biggest increase in effectiveness (100%) and User 3 had the biggest decrease (-58%).
In the Medicaid sector, User 4 had the biggest increase in effectiveness (161%) and User 3 had the biggest decrease (-6%).
In the Medicare sector, User 2 had the biggest increase in effectiveness (67%) and User 1 had the biggest decrease (-6%).
This example shows performance scores initially were below expectations. As MHS has used monitoring to enable individual user training, however, the scores have continued to rise, and effectiveness is expected to reach 70%, on average, while efficiency scores are expected to improve to less than 7 minutes, on average.
Once sector productivity was established, the MHS team could drill down into individual efficiency and effectiveness with the ability to see exactly what team members accomplished over the time period selected. By knowing who the low-performing team members are in real time, the management team can quickly work with them to improve performance and quickly drive change in their organization.
With these, and several other improved capabilities, MHS has improved staff performance and morale all while having two of the highest cash months it has experienced in the past 18 months. These results demonstrate that the new normal of work from home for patient financial services can be a reality and help future-proof an organization against disruptions such as those posed by the COVID-19 crisis.
Footnote
[1] See, for example, Digicert, “What is an SSL certificate?” Accessed June 7, 2020.





