In this interview, Janet Howard, director of member engagement at Practice Greenhealth, a Reston, Va.-based not-for-profit member organization that helps healthcare organizations with sustainability initiatives, discusses how finance leaders can support cost-saving “green” initiatives in their organizations.
On the “green always costs more” misconception. Many senior leaders, including those in finance, perceive that sustainable strategies are always pricier than traditional approaches, Howard says.
“One of the challenges is that the person who is taking the lead on sustainability may not have direct access to senior leaders in finance, so sometimes there is a disconnect,” Howard says.
The sustainability lead—usually a director-level leader in the organization—may lack the financial acumen to make the business case for a sustainability initiative, including projecting the ROI. “We urge these leads to try to connect with someone in finance to make sure they are able to speak in a language that senior finance leaders understand. That kind of communication is very important. But when it is not there, it means that many cost-saving opportunities are not fully realized,” she says. “Conversely, we work to help healthcare leaders calculate the total cost of ownership, including the cost of negative health outcomes, lost work days, and other environmental impacts. For example, styrofoam may be a low-cost product for food services, but due to its toxicity in manufacturing and challenge in recycling, it’s out of alignment with a commitment to health and the planet and not a good choice for health care.”
To bridge the gap between finance and sustainability leaders, Howard proposes that organizations hire finance interns who could help support the sustainability team on identifying viable cost-saving, healthier initiatives, and then use cost savings to fund costlier endeavors. These emerging leaders also could help the organization understand the total cost of ownership of a new green technology. In the end, environmental stewardship activities should be cost-neutral and not only seen as a cost-saving measure, she says.
On creative strategies to fund green projects. When green projects require an initial investment, organizations may turn to their development team to start a green-revolving fund. This practice has caught on in academia but has been slower to gain momentum in health care, Howard says. For example, development could raise $1 million or more to serve as an internal capital pool for sustainability projects that produce cost savings. Hospitals could then seek requests from the departments and create a green capital committee to select various projects to fund each year.
As an alternative, hospitals can partner with utility suppliers or apply for grants to fund some of these projects. “Sometimes, it does require some creativity,” Howard says.
On the No. 1 green-savings opportunity for hospitals. No surprise—it’s energy conservation, Howard says. This strategy not only helps to reduce greenhouse gases generated by facilities but also curbs costs. Howard points to Downers Grove, Ill.-based Advocate Health Care, which saved $23 million from 2008 to 2015 by reducing its energy consumption by 23 percent per square foot, equivalent to the energy required to power 19,000 homes for a year. The health system also avoided releasing 203,000 metric tons of carbon dioxide into the environment. Greener building practices that improved energy and water efficiency were key to this cost reduction.
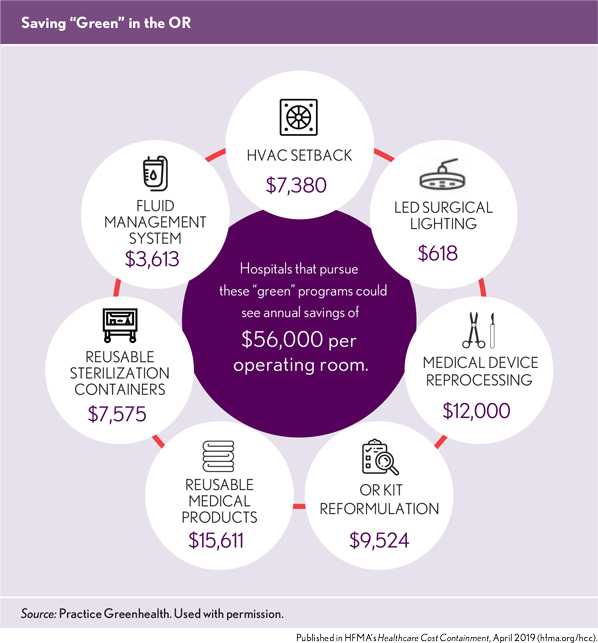
Another cost-saving strategy is using HVAC setbacks, which reduce air turnover when surgical suites are not in use. Typically, these setbacks can save more than $7,300 per operating room each year, according to Practice Greenhealth data. In fact, Cleveland Clinic was able to save $250,000 per year using OR setbacks, Howard says.
Finance leaders should recognize, though, that some green strategies, like lighting retrofits, might require an initial investment. But they do pay off in the long run: Opting for LED surgical lights in the operating rooms (ORs) can save more than $600 per OR each year and lower the ambient room temperature, creating a more comfortable surgical suite, which saves energy on cooling as well. The lights last longer, yielding maintenance and replacement savings, Howard says.
Beyond conserving energy, many hospitals also are exploring greener energy procurement. Although some finance leaders perceive renewable energy as costly, Howard says using power-purchase agreements or other procurement strategies can have little to no impact on the budget but significant cost savings. In December 2018, Rochester Regional Health in New York started purchasing renewable energy from a solar farm, a move that will allow leaders to save as much as $100,000 to $200,000 annually over time—with no up-front cost to the organization, Howard says.
On conserving water. Sterilizers in the ORs are a significant source of water usage. However, making the move to water-efficient sterilizers saves money and is better for the environment, Howard says.
Fluid management systems allow suction fluids to go straight to the sanitary sewer, dramatically reducing disposable suction canisters and improving safety. This has an impact on both supply purchasing and generation of regulated medical waste stream, a waste stream that is at least five times more expensive than solid waste. Practice Greenhealth estimates these systems can save more than $3,600 per OR each year.
On standardization opportunities. Decentralized hospitals often have opportunities to save money by moving to a centralized purchasing department that can standardize procurement strategies across the enterprise. When leaders at Mayo Clinic, Rochester, Minn., standardized their hand soaps to a single, green-certified hand soap without the antimicrobial agent triclosan, they saved approximately $200,000 a year, Howard says. In cases like these, having a clinical champion to address questions about patient safety is essential, she adds.
Advice for healthcare leaders. To gain buy-in from senior executives, leaders should align their sustainability plan to the organization’s strategic plan. “What senior leaders really want to see is the connection [of sustainability] to population health, community benefit, quality care, patient experience, safety, and risk,” Howard says. “The way that we can most successfully engage leaders is when we understand what their strategic priorities are.” For example, reducing meat procurement and transitioning to healthier meat and increasing plant-based options is a way to connect a climate strategy with health. Increasingly, clinical leaders are joining green teams to help connect the dots between environmental commitment and human health.
Howard also stresses that every single hospital function has a role to play in sustainability. This includes setting performance goals (such as a waste-reduction target) and collecting data to measure progress toward those goals. “It’s important to embed that responsibility in the leadership of every department,” she says. “All too often, sustainability activities fall on the shoulders of one person and it’s not sustainable. When leadership sets the tone and expectation and sets performance goals for key stakeholders, the momentum and return is exciting. With climate change being the biggest health issue for the 21st century, finance leaders can help embed healthier solutions for a long-term commitment to the health and well-being of staff, patients, the community, and our future.”





