4 Tactics of Effective Strategic Technology Planning for the Digital Future
The digital future for health care is a rapidly emerging certainty; the goal of evaluating and implementing innovative digital technology should be core to any healthcare organization’s strategic planning process.
As a major transformational force in health care, technology promises to significantly affect how health is managed and care is delivered in the United States. It will create a competitive market advantage for providers nationwide that are prepared to embrace it, while resistant legacy providers that fail to keep pace will experience increased market pressure. a
A complex industry in transformation demands enormously thoughtful investment in technology. Proactive providers intent on reshaping their care delivery role and processes for a digital future likely will view the types of infrastructure investments that providers typically made in the past to be insufficient and out of alignment with the ultimate transformation they envision for their organizations.
Hospitals and health systems are just now emerging from a period of massive investment in electronic health record (EHR) implementations. But they cannot expect any relief from high spending as new forces such as increased consumer expectations and new delivery models (e.g., telehealth) continue to reshape health care’s technological landscape. Significant capital spending will be needed to support investments in health and healthcare technology that meet the needs of digitally engaged consumers and other stakeholders.
See related sidebar: Current Forces Shaping the Technological Landscape
Many healthcare executives are uneasy and uncertain about the appropriate level of IT spend and where to invest allocated dollars. Such concerns are understandable and appropriate. The cost of making bad capital investment decisions can be severe, if not fatal, for organizations.
A healthcare organization’s long-term success depends on the capital investment decisions it makes today. b Such decisions must be made on solid analysis; “gut feel” is not enough in the current environment. To fully prepare their organizations for a digital future, leaders of provider organizations must use planning processes that ensure sufficient capital can be allocated through right-sized IT budgets to the right technology solutions, tailored to organizational strategies.
Following are four tactics healthcare executives can use to integrate technology into systemwide planning. Such integrated planning forces leadership teams to be deliberate with investments, identifying and funding initiatives likely to most effectively position the organization for success.
1. Commit to an Integrated Planning Process
IT provides the platform for the delivery and financing of health care, so its inclusion in the organization’s overall planning process—encompassing strategy, budgeting, financial planning, and capital allocation and financing—is essential. The need for integrated planning might seem like common sense, but the fact is many organizations continue to perform planning and capital decision making for IT as a separate process. The problem with such an approach is that it is likely to result in a portfolio of technology investments that do not fully support the organization’s desired strategic position. Such investments may be duplicative, non-standardized, and more expensive than required, and they may pose considerable security-risk concerns.
The allocation of capital for IT should occur in the same way that other types of capital initiatives are funded in healthcare organizations—within a structured process that includes the following key elements: c
- A high level of governance, education, and communication
- A coordinated calendar and planning cycle
- Direct links to a sound strategic and financial plan
- Clear definitions of available capital and capital expenditures, allowing equal access to dollars generated by the organization as a whole d
- Rigorous, quantified, and consistent business planning for each investment opportunity
- A standardized, one-batch review of potential investments
- Consistent application of quantitative analysis using corporate finance-based techniques
- Data-driven and team-based decision making
- Rigorous post-approval project monitoring and measurement
Potential technology investments benefit from the same in-depth business planning and quantitative and qualitative analyses performed for all other potential major investments. This approach ensures comprehensive consideration of an IT initiative’s short- and long-term costs and benefits—its value-add and revenue—within the organization’s overall portfolio of investments. This approach also ensures the likely financial implications of that investment are transparent and available for review. Allocation decisions are based on an initiative’s fit with the organization’s strategic plan and its individual merits, not necessarily on past or present performance of a recommending entity.
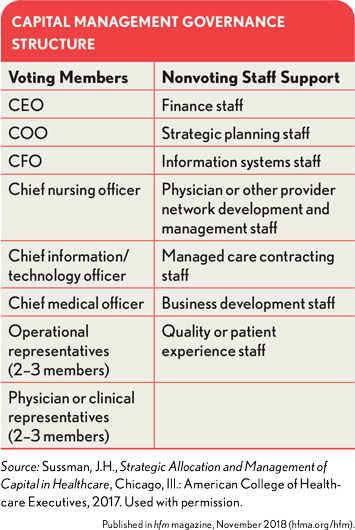
Governance of this capital allocation and management process must involve high-level corporate and operational management, as shown in the exhibit below. The decisions this group makes will have significant strategic and financial consequences for the entire organization. Governance structures also vary from organization to organization.
For example, some organizations currently do not extend voting privileges to CIOs or CTOs, although this situation likely will change due to the increasing size and scope of needed technology investments. The role of the board is to provide appropriate oversight of the process—as it does with other management processes, such as financial planning and operational budgeting—rather than being directly involved. e
2. Understand the Current State
To determine the right level and type of technology investment, leadership teams must understand their organizations’ current strategic-financial position. Each organization has its own unique strategy and capabilities. Readiness for health care’s transformation requires a specific set of competencies that includes physician integration, care coordination, service distribution, cost management, scale and market essentiality, brand identification, consumer experience and insights, payer relationships, capital capacity, and information systems sophistication that supports all these domains. f
A well-prepared organization has an IT platform that enables clinical decision making, convenient access points for consumers, information management, and facile communications for all stakeholders (e.g., clinicians, patients, and managers). The platform supports high-quality treatment and strategic decision making related to consumer-centric access, experience, health care, services, and pricing. g
Meeting the needs of digitally empowered consumers is a priority for providers, but the capabilities are not yet widespread. Ninety percent of respondents to a recent survey identified “improving customer experience” as a high priority, yet the survey also found that most organizations have a weak infrastructure for their consumerism efforts. h Only 64 percent identified “using digital tools to engage consumers” as a high priority, and less than 20 percent reported video visits and e-visits as being widely available. Organizations have much work to do to transform themselves into next-generation, consumer-centric enterprises. Deep consumer insights and analytics would allow leaders to create a realistic plan to make that transformation.
The strengths and weaknesses of an organization’s approach to technology investment can be identified through a specific assessment of the organization’s technology capabilities. To be thorough, such an analysis should look at how well applications, infrastructure/network, security systems, resiliency, and the IT organization support customer management (e.g., systems including patient relationship management, telehealth, imaging, population health/disease/care, and utilization management), workforce and facility management, billing management, reporting and analytics, and administrative back office function.
Key questions to answer in assessing the current IT platform include the following:
- What are the current pain points in key business and clinical processes?
- What business drivers have influenced current technology investment, and are these drivers congruent with organizational strategy?
- Who “owns” data and data storage, integrity, definitions, and maintenance?
- How aligned with current strategic priorities are technology-related operations, enterprise architecture, and governance?
The assessment will benefit from the engagement of the finance team and managers in departments or organizations that do not depend on IT for all their technology needs. Perspectives offered from beyond the IT department and outside the organization enhance credibility about needed future investments.i
Recent research conducted to gain a picture of how ready hospital IT platforms are for the digital future has identified three approaches hospitals are using to invest in technology. The profiles of these approaches differ based on the extent that they encompass the innovation necessary to fulfill the organization’s mission and strategy.
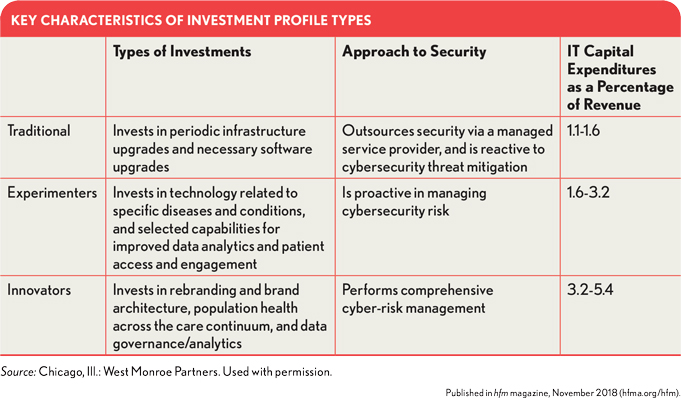
Traditional. Under the traditional approach, IT is solely a cost center, playing a support function to other business areas. If present, innovation is limited.
Experimenters. For hospitals employing an experimental approach, IT is a cost center for most functions, but in some of these organizations, technology partners with other business areas to improve operational efficiency and cost—for example, with billing and revenue cycle, and clinical documentation—and/or to positively affect revenue, such as with initiatives to enhance the patient experience and reduce referral leakage. Innovation tends to be home-grown and kept within the organization.
Innovators. Organizations that have adopted this approach are constantly leveraging and innovating technology, so that IT drives revenue as well as the optimization of costs. With a consumer-centric focus, innovators seek to deliver a superior consumer experience via a superior provider experience. The innovation pipeline is larger and broader—across patient engagement, analytics, technology-driven patient care, revenue models, and more.
With each approach, the appropriate spend as a percentage of revenue and the types of technology in which to invest are interpreted differently, as shown in the exhibit below.
3. Define a Desired Future Technology State and the Key Gaps That Impede It
After understanding the current state, the next step is to understand where the organization wishes to go and the technology that will be required to get there. j Not every organization needs to strive to achieve the innovator level of service delivery and technology maturity; the experimenter level may be appropriate. However, remaining a traditional player, which is not a recommended strategy, is a recipe for marginalization as profitability of core hospital services declines.
Extensive input from across the organization is required to define the desired strategic business and clinical capabilities and the technology that will drive and support such capabilities. That process is driven through significant contributions from, and close collaboration among, an organization’s business and IT executives.
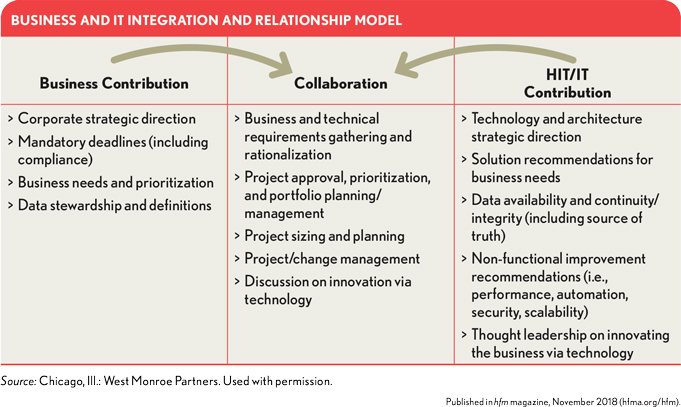
Questions that must be addressed include the following:
- Which strategies are high-value and high- priority items?
- How will IT operations, enterprise architecture, and governance be aligned with the future strategic priorities?
- How will the technology investment portfolio serve as a lever for competitive differentiation as well as a value generator for the organization and its communities?
Strategies will need to be right-sized and right-placed for the organization by the business and IT leaders. These initiatives may include population health, bundled payment, consumer engagement, health plan/risk optimization, cloud capabilities, predictive clinical analytics, superior revenue cycle operations, and, especially important, digital health.
Pursuit of digital health value.Value for the digitally focused providers of the future will be created through patient experiences that adhere to a consistent quality and generate desired outcomes financially, clinically, and experientially. To become a digital health system, an organization must exhibit three experiential capabilities: It must be accessible, integrated, and data-driven. k
Being accessible requires conveniently located facilities, mobile patient portals, online open scheduling, provider messaging, telehealth/video medicine, alternative visit options, timely access to test results, and more. Smart, omni-channel communication capabilities are essential. A training and education component may be necessary for adoption of digital healthcare offerings, but a strong technical foundation for these options—one designed in collaboration with end users—is of critical importance.
Being integrated involves developing a caregiver and patient-centric network of processes, devices, systems, and people across geographical and departmental locations. A key objective of such integration is to empower patients to take charge of their own health by providing them and their caregivers with focused and relevant information at the right time.
Security is a key consideration when creating an integrated care process. Regardless of the maturity level of integration, health systems are increasingly becoming the target of malicious cyberattacks. Understanding how to enable collaboration without exposing security risks is a challenging but necessary step.
Being data-driven means using data to develop and make recommendations to all parties involved in the end-to-end process of health care—from supply chain to caregivers to patients and patients’ social circles. To be able to make a data-driven transformation that outlines specific, evidence-based courses of action, an organization requires a strong data governance model; a defined process from data acquisition to implementation of data learning; and a team of data scientists charged with exploring data to understand consumer behavior, patient clinical conditions, intervention effectiveness, and more.
Case example: Future state and gaps.To define its desired future digital strategy and related technology needs, one health system in the Western United States started with a standard SWOT (strengths, weaknesses, opportunities, and threats) analysis. The opportunities identified included:
- Unified patient experience through a clinically and financially integrated system
- Patient advocacy not only to maintain clinical reputation, but also to build upon it
- Improved referrals from inside and outside the network
- Value-based care and bundled payments, based on knowledge of care quality and outcomes, profitability, and other analytics capabilities
The health system understood that significant progress in building out an initiative to improve the patient experience, for example, would be required. It had been tracking patients’ experiences to some extent, but it lacked a formal patient experience strategy for targeted consumers, such as Medicare Advantage members or millennials, and it had no defined metrics for tracking and measuring experience. To improve its efforts in this area, the organization would need to strengthen its ability to iteratively collect patient experience data and design interventions to enhance that experience.
Optimizing the patient experience would ensure patients are strategically and regularly engaged by means of a feedback loop. Such an approach might be appropriate for serving Medicare Advantage members, whose needs might include regular check-ins with advanced practice providers. Targeting millennials, however, might require a more innovative approach involving integration of internal and external data sources, input, and creative solutions.
The health system conducted similar vision-setting and gap analyses in many other areas, including:
- Governance
- Payer management
- Operations strategy and service line partnerships
- Processes occurring before, during, and after the time of care
- Supply chain
- Shared services
- Reporting and analytics
- Enterprise architecture and security
- Organizational change management
Based on these analyses, priorities could be set and a roadmap developed.
From gap to digital health roadmap. Financial-impact projections for a health system’s desired future state, including costs and revenue implications of required strategic and technology investments, must be thorough. Leadership teams must address questions such as the following:
- What IT/broader technology should be in place to support our strategic areas of focus?
- What does the gap analysis tell us about our biggest challenges in this regard?
- What specific resources are needed to address these challenges (e.g., infrastructure, tools, human and capital resources)?
- What cultural issues will need to be addressed, and how?
A thorough analysis estimates for each initiative the hours; types of resources; one-time costs, including software, hardware, and implementation (whether internal labor or external); and ongoing costs.
4. Create and Implement an Actionable Roadmap
The roadmap essentially defines how the organization will fill the gaps identified through the preceding analysis to achieve its desired future state. To successfully turn the corner on building the access, integration, and data-driven capabilities to move up the continuum from being a traditional investor in IT to becoming an innovator, health systems must invest in the areas identified in the exhibit below. They then must deepen their foundation in key investment areas, as appropriate to their mission and strategy.
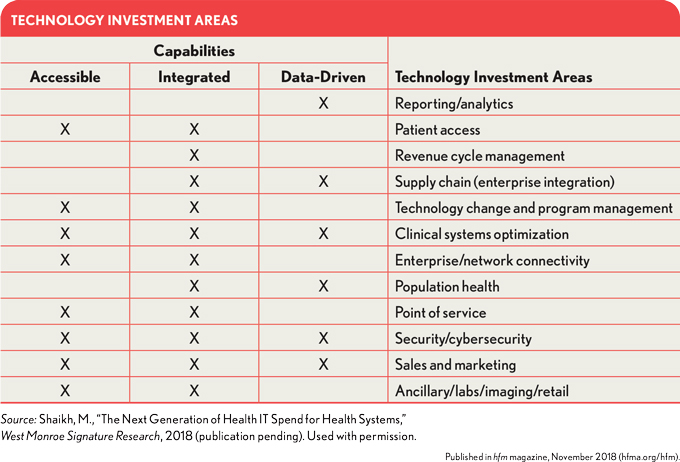
Key questions at this stage include the following:
- In what sequence should we work through our list of priority technology-related initiatives?
- What timing will be expected for putting in place the infrastructure, tools, and resources to drive IT/technology improvement?
- How will we track strategic, operational, and financial performance and identify risks, adjusting course as needed?
- How will we ensure that investments/resources create ongoing positive technological and cultural change?
Health systems typically cannot keep up with all the projects they should be doing, especially in technology. A high-quality roadmap is a practical execution tool that offers a resource-conscious arrangement and sequencing of initiatives. It is built on a foundation of data and analytics that allows the organization to prioritize its efforts over time based on the effects on patients, the impact on revenues, and the resources needed. An effective roadmap also holds technology leaders and business sponsors accountable in creating and capturing value.
Use of a value framework helps to identify value created and value captured through each proposed project or initiative on the roadmap. The framework ties the organization’s strategic objectives to each project to provide a value narrative for each project. The value framework also helps planners prioritize projects in roughly the order they should be executed and determine how to deal with projects in cases where triage is necessary.
The exhibit below provides a project prioritization matrix using value/impact and complexity as the vertical and horizontal axes. Many of the major projects on the roadmap, appearing in the upper left quadrant, are both “high” in complexity as well as “large” in impact. Typically taking longer than other initiatives, these projects require additional focus to see through to completion. Initiatives in the upper right quadrant are “high” value/impact with “low” complexity. These should be top priorities. Initiatives in the lower left and lower right quadrants should be reevaluated or accomplished, respectively.
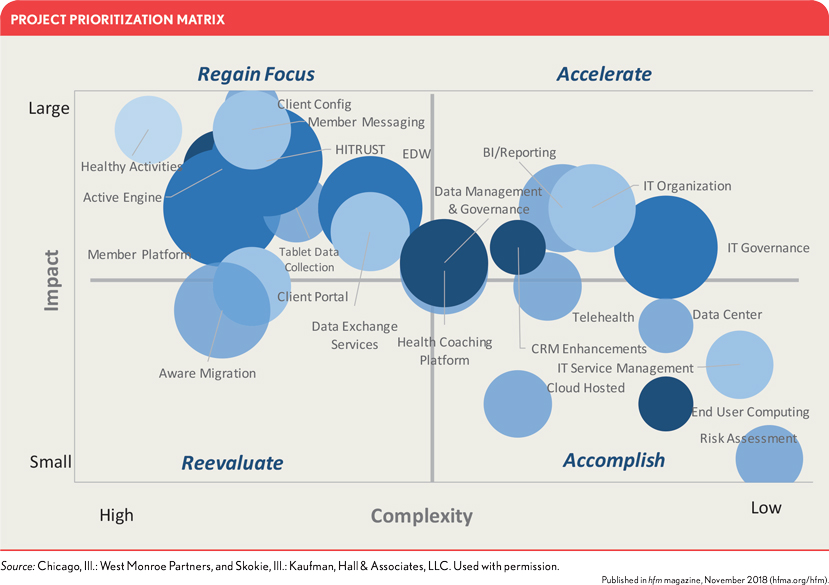
The detailed roadmap must be developed, reviewed, and revised, as needed. The development phase requires several iterations with both business sponsors and technology leaders.
At this point, the organization should form a strategic review board to assess the first version after it is completed and to navigate the changing requirements, given the changing healthcare and technology landscapes. With the general makeup of a board strategy/planning subcommittee of the board, this strategic review board should include, at a minimum, IT, clinical, strategic, financial, and operational representation (CIO, CMO, COO, CFO, and perhaps CEO). If a planning committee currently does not have IT representation, such representation should be added; if the organization is advanced and has a chief data officer or chief digital officer, these individuals should be on the board.
The board should revisit the roadmap routinely (semiannually or at least annually) to ensure its efficacy.
A strategic reporting mechanism, including dashboards and board-level summaries of key metrics, also should be developed to visualize and track the progress of initiatives along the roadmap. The exhibit below provides a sample dashboard that gives executives an “at-a-glance” view of the status of key projects, and current performance based on support, technology spend and delivery, security, and technology metrics. This dashboard can be used independently or as part of an integrated strategy management dashboard that enables oversight of performance along dimensions such as operational efficiency, clinical performance, financial health, strategic growth, and customer experience. l

Connected Services for Tomorrow’s Digital Consumers
Although the technological implications of health care’s transformation may as yet be somewhat opaque, a digital health future is clearly a certainty. Through digital technology, well-funded competitors, such as Amazon, Google, Berkshire-Hathaway, CVS, and others, will quickly resolve many of health care’s longstanding consumer frustrations, like confusing bills, long wait times, and limited primary care hours.
The transformation stakes are high for legacy hospitals and health systems. An all-important factor in moving forward more assertively to reposition an organization is the ability to identify the right level of strategic and technology spending and the right capital initiatives for each, as achieved through use of an integrated planning process. The next priority will be to gain the ability to develop and execute a clear plan for using those resources effectively to reposition the organization for a digital future. Leadership teams that recognize the value of integrated business-technology planning and an IT-enabled transformation can create connected healthcare services for tomorrow’s digital consumers.
Todd Fitz is managing director, Kaufman, Hall & Associates, LLC, Skokie, Ill.
Munzoor Shaikh is director, Healthcare & Insurance, West Monroe Partners, Chicago.
Footnotes
a. Kaufman, K., “Lower Forever,” Blog from the Chair, Kaufman, Hall & Associates, Feb. 8, 2018.
b. Sussman, J.H., “Concept Four: Allocating Capital,” In Kaufman, K., Best Practice Financial Management: Six Key Concepts for Healthcare Leaders, Chicago, ll.: American College of Healthcare Executives, 2006.
c. Sussman, J.H., Strategic Allocation and Management of Capital in Healthcare. Chicago, IL: American College of Healthcare Executives, 2017.
d. Here, equal access refers to equality of access to available dollars for all organizational entities, but not equal dollars.
e. Sussman, J.H., Strategic Allocation and Management of Capital in Healthcare. Chicago, IL: American College of Healthcare Executives, 2017.
f. Grube, M.E., Kaufman, K., “Hospital Readiness for the New Era: What We’ve Learned To-Date,” 2010 (out of print).
g. Kaufman Hall, Meeting the New Consumer Expectations—Is Your Organization Ready? June 2016.
h. Crnkovich, P., Clarin, D., and O’Riordan, J., 2018 State of Consumerism in Healthcare: Activity in Search of Strategy, Results of the Kaufman Hall Healthcare Consumerism Index, June 2018.
i. Shaikh, M., “The Next Generation of Health IT Spend.” West Monroe Signature Research, 2018. (publication pending).
j. Shaikh, M., and Amiot, M., The Next Generation of Health IT Spend: Where Should Health Systems Invest? Signature Research, West Monroe Partners, Nov. 1, 2017.
k. Shaikh, M., The Next Generation of Health IT Spend for Health Systems, Signature Research, West Monroe Partners, 2018 (publication pending).
l. Goetz, K., Spence, J., Shoger, T.,“Strategy Management: From Goals to Results,” Whitepaper, Kaufman Hall & Associates, LLC, 2018.





