How a new view of performance improvement can help healthcare organizations rein in costs

With the right systems and infrastructure in place, organizations can integrate their clinical and financial management and genuinely transform their organizational approach to managing costs.
As hospital leaders confront the prospect of long-term, sustained declines in payment, it is imperative that they develop, establish and communicate financial targets for cost-reduction initiatives that can help them create a pathway to financial sustainability. To do so, they must set aside the common historical assumption among hospital boards that volume will increase year over year, which has too long allowed them to avoid making tough decisions about where to cut costs.
Set and sustain realistic targets using a data-driven approach
Succeeding in today’s more challenging financial environment requires a disciplined, data-oriented approach that reflects previous performance, blends financial and clinical analytics and begins with a clear understanding of how far the organization must go to create a sustainable path forward.
Although each organization must develop and refine its target by assessing a range of clinical, financial and market-specific factors, all organizations may find that establishing at the outset an initial goal of breaking even on Medicare payment is an effective minimum benchmark, because it requires most hospitals to dramatically improve their performance.
According to the Medicare Payment Advisory Commission, the average Medicare margin for hospitals was –9.9% in 2017; even hospitals providing high-quality care at lower costs performed at –2%. However, according to the Kaufman Hall/HFMA 2019 Healthcare Performance Improvement survey, 84% of respondents said their organizations’ target for cost reductions over the next three years was 10% or less.
Emerging systems allow organizations to integrate data on financial and clinical performance, and analyze indicators ranging from productivity to service utilization to cost-effectiveness. Current comparative analytics tools also allow hospitals to access real-time or predictive data, a major improvement from traditional retrospective data.
Increased data on its own, however, will not necessarily lead to improvements in performance. Hospitals run the risk of becoming data rich and information poor, with harried department leaders deluged with monthly analytics reports that are more a source of noise than actionable information.
Comparative analytics systems that compile and provide benchmarks for similar institutions can help hospital leaders better understand how their performance aligns with and varies from that of peers. These efforts should be grounded in developing a meaningful understanding of why variance from benchmarks occur before potential adjustments are determined.
For instance, an organization might discover that its staffing for a specific service line exceeds that of its peers by one clinical full-time employee (FTE). However, the FTE in question might deliver an increased positive impact on patient care or satisfaction by meeting a specific clinical need not met by peer organizations.
Stay on course using a results management office
Organizations can make the most of their analytics only when their leaders and staffs are empowered to act on the analytics’ findings. For many organizations, the solution is to create specific performance improvement champion roles that empower senior leaders to drive change and take accountability for organization-wide results. However, this approach can sometimes hamper accountability at the department or individual unit level by creating the perception that the champion is solely responsible for the success or failure of the project.
An effective approach to promoting accountability throughout the entire enterprise is to create a results management office that reports and tracks results — but is not responsible for the performance of individual departments.
One hospital in a mid-sized Midwest city, facing a $15 million performance gap projected to grow to $40 million in five years, performed a comprehensive assessment to identify areas of improvement across the entire enterprise. As part of its overall cost reduction effort, the system established a results management office charged with answering the following questions:
- What are the services we are using?
- Are we using them in an optimal way?
- How can we maximize the effectiveness of our spending to provide the level of service and product that are important to both patients and clinicians?
The office reported results to the system’s controller, who reported directly to the CFO. The results management office, in its role of monitoring organizational change, also offered project management assistance to those responsible for specific initiatives. Two years into the initiative, the system hit 96% of its overall cost management target.
Effective cost management depends on systems and infrastructure
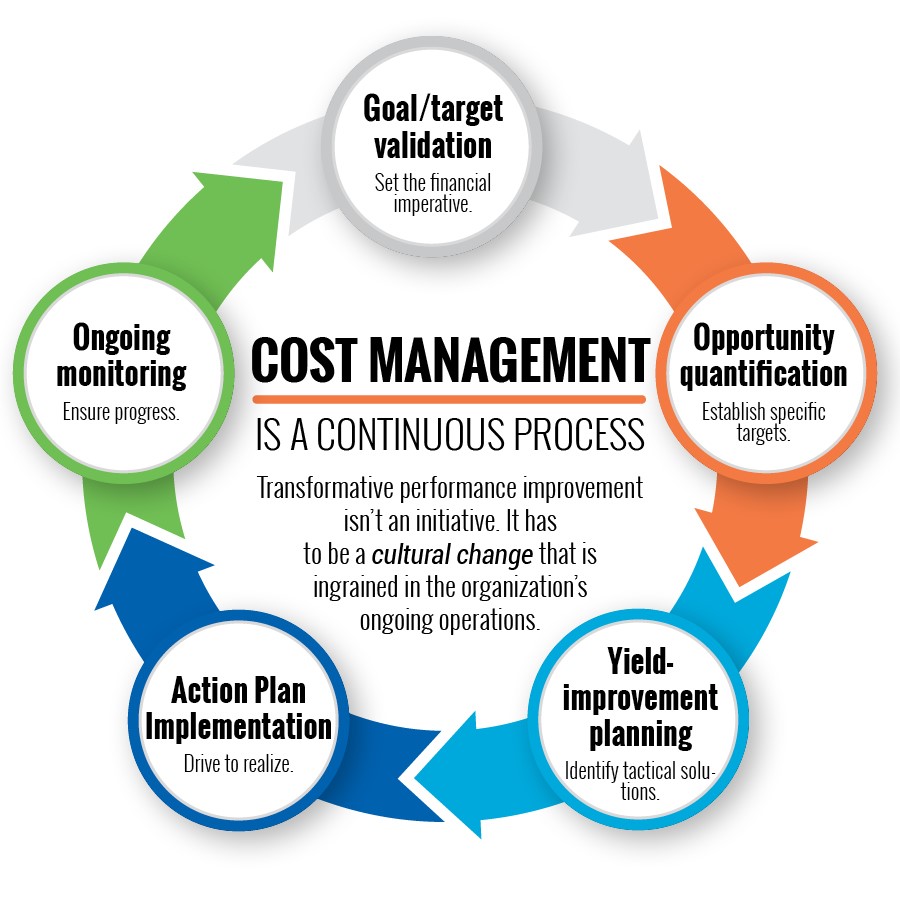
With the right systems and infrastructure in place, organizations can integrate their clinical and financial management and genuinely transform their organizational approach to managing costs. Ultimately, cost reduction should be part of an organization’s DNA — and a continuous journey, not a destination.
This article is excerpted from a three-part series on performance improvement. For more information, visit Kaufman Hall’s website.
Sidebar: Cost management pitfalls and best practices
Avoiding cost management pitfalls and implementing best practices are key to overall performance improvement. Here are some easy-to-follow tips.
Pitfalls
- Making budgeting determinations based on the assumption that volume will increase
- Having a narrow focus on peer group performance
- Flooding staff with too much data
Best Practices
- Analyzing prior performance as a predictor of future volumes
- Probing into the root causes of variance
- Training staff to effectively use real-time data






