How one hospital improved patient access, specialty referrals and completed-appointment rates
Texas Children’s Hospital recognized it had a problem: Too many patients could not get the care they needed when they needed it. The hospital responded by launching an initiative to overhaul its referral and scheduling processes, and the payoff was evident after only one year.
An expanding patient base traveling from all 50 states and nearly 70 countries challenged the mission of Houston-based Texas Children’s Hospital: to provide women and children with access to exceptional healthcare. Facing long wait times to access care, patients were unable to get through the door. Leadership knew limited accessibility could lead to poor health outcomes and, in turn, damage the organization’s reputation and financial well-being.
In August 2017, Texas Children’s launched an initiative to increase access across all its entities. The effort helped the organization achieve signifi cant improvements in performance and access within the first 12 months. The Access and Patient Scheduling 1.0 Task Force, which was conceived by the organization’s CEO and directed by a team of hospital executives and physician leaders, succeeded in transforming pediatric specialty-care access and did so without adding incremental clinical resources.
The access-improvement journey required organizational transformations focused on:
- Improving referrals to pediatric specialty care
- Optimizing capacity and utilization of clinic appointment slots
- Improving the patient-appointment scheduling experience
Improving referrals to pediatric specialty care
Texas Children’s uncovered issues with outside referrals and reinvented the process to achieve higher levels of efficiency. In doing so, the organization realized an 11.5% increase in completed appointments by the end of FY18 over FY17 performance, and has continued to see improvements in FY19. (See the exhibit below.)
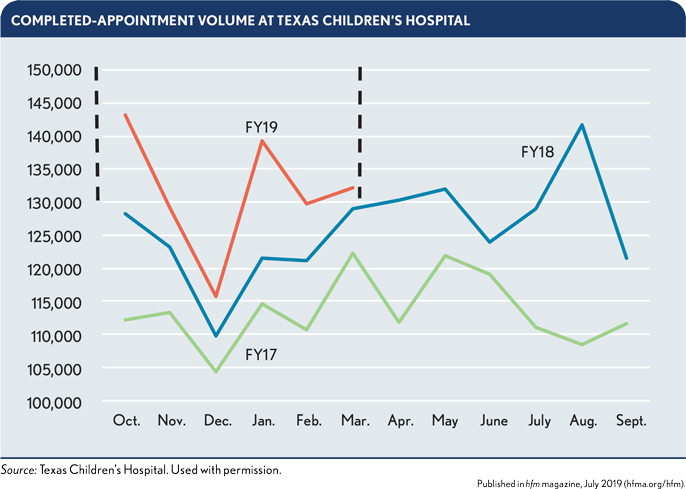
The following were key components of the new approach.
Streamlined referral processes. For specialty-clinic referrals, more than 60 processes were identified across the system, with over 40 submission routes. On average, the referral process took two minutes to complete. The lack of standardization resulted in inefficient scheduling methods and lost or incomplete submissions.
The referral process was transformed to create a simple, uniform process, with more than 90% of the referral content standardized and coalesced into one submission form. Submission time was reduced to just 30 seconds through use of the new form.
With just one submission route, the request process was significantly accelerated. Texas Children’s achieved a new service level of one business day to convert referrals into patient-outreach attempts to schedule appointments.
Automatic referral responses. The hospital added a standardized response to be sent to referring providers within 24 hours of a submission, with a follow-up notification transmitted when an appointment was scheduled.
Automatic visit summaries. Under the old model, after referrals were made to Texas Children’s clinics, outside physicians received inconsistent feedback about patients from the hospital’s providers. In fact, only 60% of Texas Children’s specialty clinics automatically sent visit summaries to referring providers. To address this lack of communication, which can be harmful to patient health and may result in unnecessary utilization, a standardized process was created within the electronic health record (EHR). The idea was to ensure correspondence between physicians.
Now, when a specialty provider sees a referred patient, a letter with pertinent information is automatically generated from the documentation of the consultation and sent to the referring provider. With this standardized process, Texas Children’s specialty providers have attained a 100% success rate for sending visit summaries to referring providers.
External provider portal. This portal was developed to maximize the communication and delivery of information between Texas Children’s providers and external physicians. Outside physicians may obtain a limited version of the EHR to view records of mutual patients, eliminating lost information and redundant medical services.
Access to Texas Children’s EHR includes the ability to make electronic referrals, receive test-result notifi cations, view patient face sheets and demographics and send HIPAA-compliant messages. Outside physicians thus remain up to date with patient care and treatment plans, enabling them to provide the best care possible and be more productive. After implementation of the provider portal, a survey of referring physicians revealed 85% were more likely to refer a patient to Texas Children’s.
Optimizing clinic-appointment capacity and utilization In FY17, around 20% of clinic appointments went unfilled, with appointment cancellations reaching 292,000 for the year. The task force investigated how to convert canceled and vacant appointment slots into dynamic access opportunities to maximize clinic schedules and increase timely patient access.
The team expanded new-patient appointment slots by 44% and added over 53,120 annual patient appointments, a 3.7% growth over FY17.
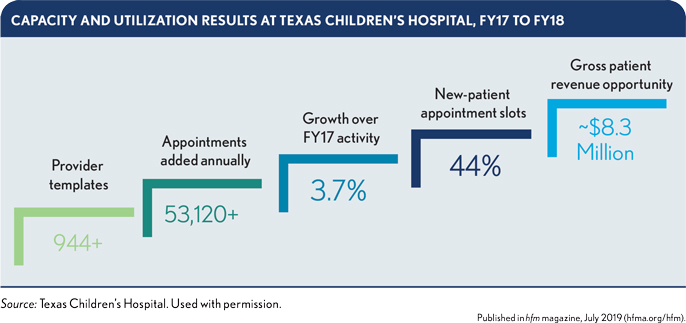
Physicians’ completed appointments outpaced the FY18 budget by 2.8% as an institutional trend.
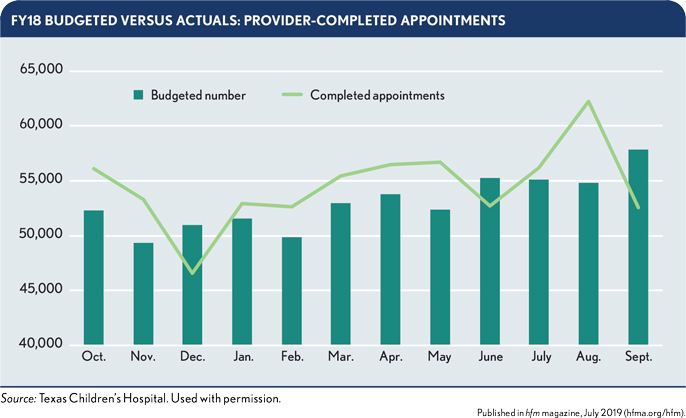
Enhanced patient access generated an $8.3 million grross patient revenue opportunity, acheved via the following approaches.
Maintaining open and fl exible schedulss. In the previous approach, restrictive scheduling practices were applied, visits were specialtyspecific and time slots were held for various reasons. By establishing that all unutilized appointment slots automatically would be released 72 hours out, the task force ensured additional new appointment slots were available. Appointments could be within the physician’s realm of practice and did not have to be specialty specific.
Ensuring provider availability. With clinic schedules differing between providers, over 944 providerscheduling templates previously were in use. Setting and adhering to a specific, fixed clinic time offers more appointment availability and more productive labor hours.
As part of the new initiative, the organization defined a clinic session as a time interval of four hours. Applying this standard definition across all templates ensured four hours of clinic availability and supported governance to ensure accountability.
4 elements to upgrade and improve the scheduling experience
To create ease in scheduling, enhance throughput and improve patient access, Texas Children’s embraced advanced technology and adopted a patient-centered electronic patient portal and scheduling system.
Today, 83% of specialties can offer the thirdnext available new-patient appointment within 14 business days, an increase from 66% in FY17.
The following elements allowed Texas Children’s to upgrade the appointment-scheduling process.
1. Patient portal. The portal allows patients to take control of their healthcare by having access to medical records, test results and appointment scheduling and maintaining communication with staff and physicians. Utilization of the patient portal increased from 51% to 60% in FY18 after a hospital-wide campaign. Patients reported high satisfaction with the portal.
2. Online scheduling. Survey results revealed that online appointment scheduling is the preferred option for most patients. Two online options were implemented.
First, the online patient portal allowed established patients to schedule appointments electronically. To date, online self-scheduling via the portal has generated more than 2,000 appointments, validating the use of technology to engage patients. No-show rates also were reduced for appointments scheduled through the portal, and the hospital’s Press Ganey Top Box ease-of-scheduling scores increased from 57% to 72% in the first year following implementation.
Second, online scheduling was expanded to new patients via a scheduling widget on texaschildrens.org. In just six months, more than 2,000 new-patient appointments were scheduled through this system.
3. Electronic automated wait list. Maintaining scheduled clinic appointments is a challenge, with high rates of canceled appointments happening within 24 hours and most of those slots going unfi lled. In response, Texas Children’s created an electronic automated wait list as a feature within the patient portal. Patients may enroll on the wait list if they schedule an appointment but prefer an earlier appointment time. If an appointment cancellation occurs, this opening instantly becomes available and offered to patients on the wait list via a text or email notification. Clicking the confirmation automatically schedules a patient for the new appointment.
Efficiency in filling those appointment times has increased by eliminating “phone tag.” More appointment slots have been filled, and appointment wait times have declined by 52 days on average for the more than 500 patients who have used the wait list.
4. Sustainability plan. Under the old model, nearly 400 internal EHR users had access to make permanent scheduling changes. To sustain the scheduling improvements, permission settings have been limited to a smaller, centralized group of users. This change has ensured that Texas Children’s can more efficiently maintain institutional improvements and can solidify new standards for a patient-centric approach to scheduling.
Additional aspects of the sustainability plan include limiting the ability of users to change templates, removing holds during certain appointment slots and requiring a formal approval process to make permanent changes to the scheduling approach.
What it takes to successfully revamp processes
Texas Children’s Hospital made significant organization-wide improvements in just 12 months thanks to a process revamp that involved various groups and departments within the hospital:
- A strong physician partnership was at the center of the task force, allowing for a transformation of the organizational culture and improvements in clinical processes.
- Adaptability of information services facilitated the technological advances needed to support the development of additional software while ensuring patient privacy and safety.
- Frequent meetings of the executive steering team ensured that the focus and vision of the initiative were translated into actions and accomplishments.
- Marketing and communication were at the forefront in elevating patient usage of new digitized features, thus enhancing workforce productivity.
The experience of Texas Children’s confi rms that healthcare organizations can overcome obstacles and overhaul operations in ways that are favorable to both patients and hospitals. In its journey to improve the patient experience and health outcomes, the organization has launched the next iteration of the task force to investigate additional opportunities for patient-access improvements (see also the sidebar on how the patient-access initiative created revenue opportunities).
Texas Children’s Hospital at a glance
Texas Children’s Hospital is a not-for-profit pediatric hospital located in the Texas Medical Center in the heart of Houston, with locations spanning the surrounding areas and as far away as Austin. Behind a workforce of more than 14,000 physicians, nurses and other employees, Texas Children’s provided care to more than 4.3 million patients in FY18.
Texas Children’s provides expert care in more than 40 pediatric subspecialties, is nationally ranked in all 10 children’s specialties by U.S. News and World Report and enhances its provision of specialty care services through partnerships with external providers. The experience of Texas Children’s confirms that healthcare organizations can overcome obstacles and overhaul operations.





