5 lessons on launching a provider-sponsored health plan
Market trends are shifting to enable increased adoption of provider-sponsored health plans (PSHPs), often through strategic partnerships.
As leading health systems begin to enjoy success in launching provider-sponsored health plans (PSHPs), the potential benefits of health plan ownership are coming into focus. Lessons learned from health systems that have succeeded in the area can serve as a guide to others that have struggled with finding the best way forward. Health systems that have navigated the PSHP terrain can show the way by illuminating the key challenges in operating a PSHP and pointing to the capabilities required for success.
Shifting health system interest in PSHPs
Interest in launching a PSHP has waxed and waned among U.S. health systems in recent years. By 2017, more than 100 health systems provided coverage to about 18 million members through PSHPs.1 It seemed that PSHPs might become the new normal, altering health systems strategies and enabling them to capture market share. Yet struggles to grow membership profitably caused excitement to dim for many health systems.
Today, however, interest in PSHPs has been rekindled in part by health systems’ growing discontent with alternative “payer-provider partnerships.” Over the past three years, the paucity of payer-provider collaborations that have successfully built true joint-risk models has caused many health systems to reconsider their health plan strategies.
It is expected that many of the plans entering the Medicare Advantage (MA) market in the next two years will be PSHPs.2 Among executives of leading health systems responding to a 2018 survey, 27% anticipate launching an MA plan and 29% are confident in their systems’ ability to do so.
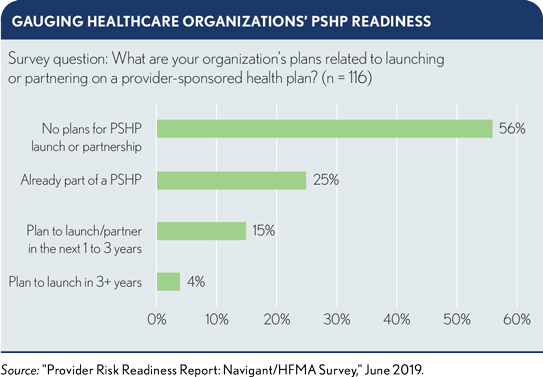
Meanwhile, a recent risk-readiness survey also finds emerging interest in PSHPs:3
- Among provider leaders surveyed, 72% (i.e., 86% of health system respondents and 66% of hospital respondents) plan to assume additional risk, including sponsoring a health plan, in the next one to three years.
- One-in-five respondents say they plan to assume risk by launching a PSHP.
- One quarter of respondents are already part of a PSHP.
(For additional discussion of the factors driving renewed interest in PSHPs, see the web-exclusive sidebar, “Providers explore new territory with health plan ownership.”)
How leading health systems are navigating success
Health systems that have successfully launched PSHPs invariably have already addressed capabilities and competencies needed to start a PSHP. (See the sidebar.)
Here, we offer lessons learned from four health systems that are beginning to realize real benefits from their PSHP strategies.
Lesson No. 1: Use data analytics to inform your approach. Optima Health, the health plan division of Sentara Healthcare, a 12-hospital system based in Norfolk, Va., uses artificial intelligence to identify members who are at high risk of developing sepsis.
The health plan’s approach has:
- Significantly improved accuracy of risk detection
- Reduced redundant nursing staff screenings by 70%
- Decreased manual screening hours by up to 72% while ensuring patients at risk receive the care they need more quickly
Meanwhile, use of data analytics has enabled the health plan to identify unnecessary emergency department (ED) encounters, realize opportunities for millions of dollars in ED savings and develop protocols, including patient education, that help ensure the right care is delivered at the right time.
“We’re just beginning to understand the potential to improve quality of care and member relationships through data analytics and artificial intelligence,” says Howard P. Kern, president and CEO, Sentara Healthcare. “Having a provider-
sponsored health plan gives us a much richer view of the data needed to drive improvement.”
Among other leading PSHPs that also leverage data analytics to design care management services that focus on the areas of greatest impact is Danville, Pa.-based Geisinger Health Plan. Care managers at the PSHP work with 15% to 20% of the health plan’s Medicare population — a much higher percentage than under traditional payer models, where care management typically is limited to the top 5% of the highest-cost Medicare members. The results have been outstanding: Efforts to lower acute inpatient stays have reduced costs by 19% per member per month (PMPM).
“If you want to reduce PMPM costs, you need to know where your costs are coming from, and that varies by line of business and whether the plan is commercial, Medicare or Medicaid,” says Janet Tomcavage, RN, MSN, chief population health officer for Geisinger Health Plan. “In a Medicare population, most of the costs are coming from hospital admissions, ED visits and post-acute care. If you can prevent the inpatient admission, you’ll also prevent a skilled nursing facility admission. The impact on cost is significant, since an avoided hospital admission for a Medicare patient saves on average around $12,000. If the patient has more complex medical conditions, that amount could increase to $18,000 to $20,000.”
Lesson No. 2: Be prepared to sustain losses in the first years after implementation. Given the amount of investment in talent and infrastructure required to support a health plan, the enrollment thresholds required for success and the challenges associated with managing the health of complex populations, health systems should plan for the time it will take to get such a large undertaking up to scale and fully operational.
“Until you’ve built sustainable scale, you have to accept that for a number of years, you’re going to have losses,” Kern says. “Many health system leaders think, ‘I’m going to get a health plan, and it’s going to be great. I’m going to make money, and I’m going to improve health outcomes.’ They overpromise results to their board. As a consequence, when the health plan experiences losses, they are greatly disappointed, and they end up losing trust. They get a lot of pressure to dump everything and exit.”
Kern notes that Optima Health lost money the first 12 years after the health plan was launched. “We learned a lot of hard lessons those early years,” he says.
Lesson No. 3: Create programs tailored to meet the needs of specific populations. Presbyterian Health Plan, part of Presbyterian Healthcare Services in New Mexico, offers home-based care for high-need Medicare Advantage (MA) members and Medicaid members with serious illnesses and functional decline who are at risk for long-term institutional care. The goal of this program, called Complete Care, is to focus on the 5% of members who account for 50% of total medical costs.
Complete Care uses a multidisciplinary care team and wrap-around approach to care, including:
- In-home access to primary care
- Same-day urgent care
- Foot care (critical for members with diabetes facing high risk of amputation)
- Limited spectrum of acute care services, such as X-rays, lab collection and vaccine administration
- Social support and palliative care as needed
Complete Care began as a home-based program and expanded in 2018 to include an outpatient clinic. Its approach is designed to reduce costs of care while helping members achieve their quality-of-life goals.
“Complete Care’s readmission and hospitalization rates are less than expected for this population,” says Sharon L. Fletcher, PhD, MBA, president of Fluent Health, a subsidiary of Presbyterian Healthcare Services that leverages Presbyterian’s 30 years of managed care experience to partner with providers seeking to start or strengthen their PSHPs. “Not only does this represent a significant decrease in costs, but also a seamless care experience,” Fletcher says.
At Optima Health, MA members are concentrated in specific medical practices that are uniquely positioned to meet the complex care needs of MA patients, including patients with multiple chronic conditions and behavioral health needs.
“We’ve found that when the MA population is spread too broadly, we’re unable to achieve the same level of effectiveness as when these members are directed to practices that are finely attuned to working with MA members,” Kern says.
Kern cites two other keys to success in managing MA members’ health:
- The use of extensivists who can extend care for MA members outside traditional care settings, such as the home or assisted living facilities.
- The addition of specialized coding staff within MA-focused practices.
Lesson No. 4: Seek ways to partner with the health system’s clinical team in developing high-value interventions. At Presbyterian, the health plan pharmacist has collaborated with the care delivery team to promote the use of highly effective, cost-efficient prescription drugs, thereby lowering medication costs and driving positive member outcomes. Such innovative approaches are critical given that Americans spent $535 billion on prescription drugs in 2018, while rate hikes in 2019 average 6% for more than 1,000 medications.4
“Over 90% of our physicians now prescribe more cost-effective medications to our members,” Fletcher says. “We’ve focused on diabetes, hepatitis C and growth-hormone drugs to establish best practices in prescribing that improve care while reducing costs.”
Through collaboration with clinical pharmacists, physicians and other Medicaid health plans, Optima Health has developed opioid prescribing interventions that have reduced opioid prescriptions by 43% since October 2017. Today, 30% fewer members receive prescriptions for opioids, which is a potentially life-saving improvement, given the addictive nature of these drugs and the nation’s opioid epidemic.
Lesson No. 5: Invest in high-touch, high-tech solutions for member engagement. At a time when tech-enabled MA startups are clamoring for enrollees, PSHPs are compelled to tightly hone their member-engagement strategies, including the use of digital tools that help members manage their health and the cost of their care.
SelectHealth, the PSHP for Intermountain Healthcare in Salt Lake City, partnered with a vendor to develop a mobile pharmacy benefit app that helps members save money on their prescriptions. The mobile app provides information around:
- Drug prices and potential lower-cost alternatives
- Medications covered by the plan
- Tier statuses of prescription drugs
- The member’s prescription copays and benefits
- Maintenance drugs
- Explanation of benefits for the members’
drug claims - Preauthorization and step-therapy requirements
- Participating pharmacies
“The most effective tools enable members to do things themselves, such as schedule appointments with specialists, check their prescriptions and transfer records,” says Eric Cannon, PharmD, FAMCP, associate vice president of pharmacy benefit services for SelectHealth.
A revitalized opportunity
After briefly seeming to lose steam, PSHPs are coming around again. This time, health systems that plan to launch a PSHP for the first time have the benefit of drawing from other providers’ experiences to design their approach.





