Federal scoring system spurs state action on certificate-of-need laws
Other expected 2026 state legislative action includes Medicaid cuts.
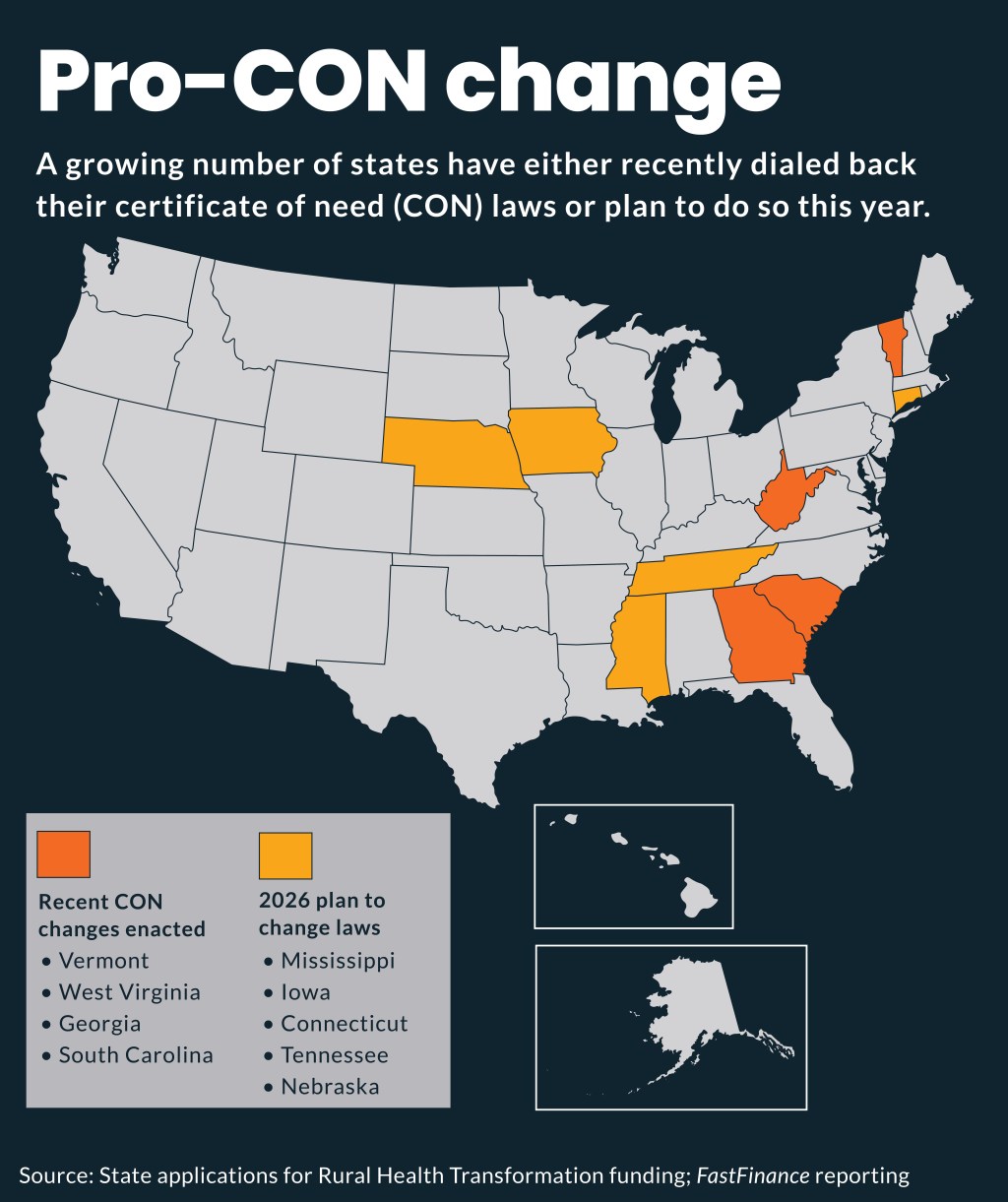
Spurred on by the Trump administration, five states plan to undertake changes in their certificate-of-need (CON) laws this year:
- Mississippi
- Iowa
- Connecticut
- Tennessee
- Nebraska
Their plans were highlighted in late 2025 applications for a share of the $50 billion Rural Health Transformation (RHT) program, authorized by the One Big Beautiful Bill Act (OBBBA).
That law allowed the Trump administration to develop a scoring system that would reward states for taking certain actions. One of those actions was changing their laws to increase healthcare provider competition in their states.
If states do not make the promised changes to state law, CMS may claw back some of the funding that it approved in late 2025.
Initiative so far
Earlier this month, the Mississippi House Public Health and Human Services Committee approved the same CON bill language from last year’s legislative session. The new bill was tweaked to drop a provision that led Gov. Tate Reeves (R) to veto the legislation. The bill would allow medical facilities to make improvements to buildings and medical equipment without state approval.
The Mississippi Hospital Association stated last year that it opposed CON law changes “which harm member hospitals by duplicating healthcare services and redirecting profitable service lines without the ability to offset costs of uncompensated care.”
Tennessee pledged 2026 action on CON law changes.
“Tennessee will introduce and pass legislation to eliminate CONs across facility categories in the 2026 legislative session,” stated its RHT application. “The elimination of CON will reduce barriers to entry for new providers, which will help facilitate greater access, lower costs, and improve quality of care. Implementation will occur by Jan. 1, 2027.”
Tennessee state legislative leaders said no specific legislation has been filed and potential fiscal impacts have not yet been studied but noted that the filing deadline for legislation is Jan. 31, according to local media reports. Legislation introduced in 2025 to remove acute care hospitals from the requirement of obtaining CON approval after July 1, 2028, did not advance out of committee in either chamber.
The Tennessee Hospital Association said the 2025 legislation would cause hospital closures, cutbacks in the types of services offered at local hospitals and ultimately result in a reduction in the availability of care for many Tennesseans.
Connecticut also promised “simplifying and refreshing the purpose of our CON laws to promote market competition and remove barriers to entry.”
The Connecticut Hospital Association backed a 2025 bill that would create an expedited process for increased licensed bed capacity.
Hospital advocates also sought changes to the bill if it was brought back this year. Changes sought included streamlining the CON process by not requiring approval for the relocation of any outpatient service within the same municipality or for the termination of inpatient or outpatient services due to various factors.
Medicaid cuts expected
In addition to the rural health funds, OBBBA also implemented a series of Medicaid cuts over the next several years, some of which will spur state legislation.
Most states have not yet released their next budget proposals, but Texas, Colorado and Idaho already have proposed Medicaid cuts.
In Colorado, Gov. Jared Polis (D) proposed rolling back a planned 1.6% increase in Medicaid provider rates as part of more than $250 million in budget cuts to address a funding shortfall. Additionally, certain provider rates would be reduced to 85% of Medicare rates.
Idaho would cut 4% across all Medicaid provider types and services, except for payments to Indian Health Services and other tribal clinics.
Texas proposed rate reductions for FY27 for substance-use treatment facilities and durable medical equipment.
Washington state hospital advocates recently raised concerns about cuts focused on those facilities in Gov. Bob Ferguson’s (D) budget, including:
- Reduced Medicaid payment for outpatient services provided in off-campus, hospital-based clinics
- A carve-out of the Medicaid pharmacy benefit from managed care, prohibiting 340B entity retail pharmacies from recognizing 340B discounts
The first cut would target facility fees for outpatient clinics and cut $38 million annually from hospitals.
The state hospital association stated that the cuts were needed to fill a projected $1.6 billion to $2.3 billion deficit over the next four years caused by rising caseloads, inflation, a cooling labor market and softening housing activity, as well as unprecedented trade shifts and federal spending cuts.
“Gov. Ferguson’s budget proposal fails to recognize the perilous financial position for hospitals created by state-imposed payment cuts and tax increases and” OBBBA, stated the Washington State Hospital Association. “Not only does the budget fail to provide relief, but it also proposes further cuts to Medicaid hospital reimbursement.”





