Why rural hospital finances improved in 2025
Strategic financial options were increasingly pursued by rural hospitals in 2025.
Although rural hospitals remain in financially precarious positions, their overall finances improved in 2025. The reasons for this enhancement likely vary by market.
The national median operating margin for rural hospitals has improved over the last three years: from -0.1% in 2023, to 1.0% in 2024 and 2.0% in 2025, according to the annual Chartis tracking of their finances.
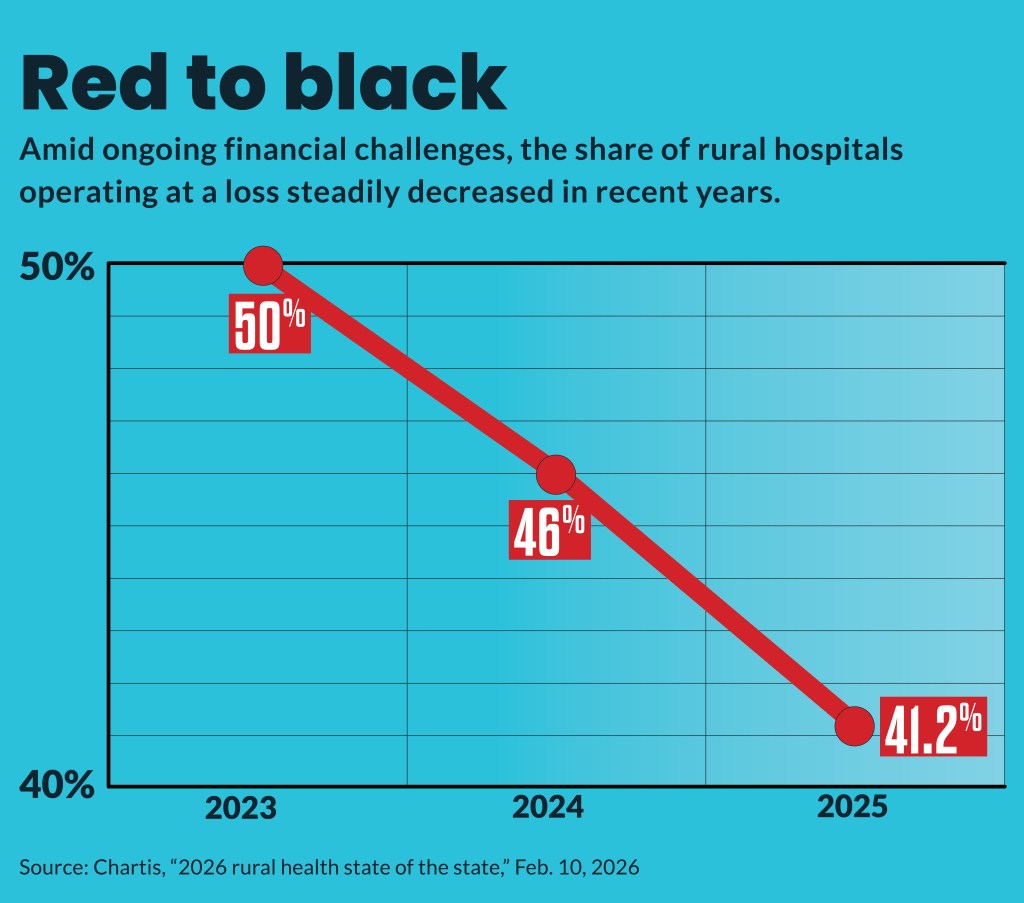
Another finding from data from 2023 to 2025 included the share of rural hospitals operating in the red:
- 50% in 2023
- 46% in 2024
- 41.2% in 2025
“Those numbers did improve slightly and a big part of that is the Medicaid expansion,” said Michael Topchik, partner and executive director of the Chartis Center for Rural Health.
In Medicaid expansion states, 34.9% of rural hospitals are in the red, while 52.2% had negative operating margins in non-expansion states. Similarly, expansion state rural hospitals had 2.9% median operating margins, while non-expansion ones had a -0.7% median operating margin.
The share of hospitals that Chartis’ analysis deemed in danger of closure varied from 418 in 2023 to 432 in 2024 and 417 in 2025.
Closure risk was underscored by the finding of 18 rural hospital closures over the last three years, according to tracking by the Sheps Center for Health Services Research. However, there were 11 closures in Medicaid expansion states and 7 in non-expansion states.
State variation
The picture became more complicated at the individual state level.
While rural hospitals in most states improved their finances from 2023 to 2025, that improvement — and some deterioration — varied widely.
Improvements. States that saw their share of rural hospitals with negative operating margins decrease the most in terms of percentage points included both expansion and non-expansion states:
- Kentucky 38 points (to 8.3%)
- Arizona 34 points (to 6.3%)
- Vermont 33 points (to 42%)
- Iowa 29 points (to 13%)
- New York 26 points (to 57%)
- South Carolina 25 points (to 27%)
Deterioration. Similarly, both expansion and non-expansion states were among those seeing the biggest increase in their share of rural hospitals with negative operating margins:
- Maryland 15 points (to 40%)
- Texas 14 points (to 46%)
- Nebraska 7 points (to 49%)
- Oregon 6 points (to 50%)
- Hawaii 6 points (to 46%)
- Pennsylvania 5 points (to 45%)
Why variation
Topchik said there’s likely a range of state-specific healthcare policies driving that variation. For example, in New Mexico, where rural hospital closure risk decreased 14 points to 26%, the state created the Health Care Affordability Fund to provide extra subsidies for ACA exchange enrollees.
Pennsylvania hospital executives have told Topchik that the low margins Chartis has found don’t reflect their reality because it doesn’t account for state funding on top of their operating revenue.
Many expansion state hospitals also have benefited more from Medicaid state-directed payments (SDPs), which can increase Medicaid payments to as high as average commercial rates.
For instance, SDPs improved Medicaid rates for Owensboro Health, which operates a 477-bed hospital in rural Kentucky, according to Fitch. That SDP revenue contributed to the rating agency last year upgrading the organization’s revenue bond rating.
Wider trend
Rural hospitals’ financial improvement also came amid broad hospital and health system financial improvement since the 2022-2023 timeframe, according to Fitch Ratings.
Over recent post-COVID-19 years, hospital volumes have surged, while organizations have focused on delivering productivity enhancements and process improvements. These have helped improve cash flows for investment and to maintain balance sheet strength, according to Fitch.
Many rural hospitals have lagged in overall financial improvement because they lacked the ability to afford increasingly costly technology upgrades or to implement the value-based payment (VBP) push from Medicare and Medicaid, said Teresa Waters, PhD, an economics professor and dean of the Augusta University School of Public Health.
“That’s just a lot to ask of small organizations who are also facing other challenges,” Waters said in an interview.
Strategic options
Some rural hospitals also have used strategic moves to improve their financial positions in recent years.
“There are a lot of options available to rural hospitals and they are exploring them,” said Waters. “There are no magic bullets out there.”
Regional partnerships. Such partnerships among independent rural hospitals aim to pool resources to expand access to care, increase the use of health information technology and explore alternative healthcare delivery models. There are at least 40 such regional partnerships around the country comprising mostly independent hospitals, according to one assessment.
Topchik highlighted the emerging push toward rural hospital clinically integrated networks as another trend to watch.
However, not much data have emerged about whether such arrangements have boosted the finances of their rural hospital members, said Topchik and Waters.
Consolidation. Merging with a health system or other independent hospitals has benefited some rural hospitals. A majority (55%) of rural hospitals that closed from 2011 to 2021 were stand-alone hospitals, according to a 2024 analysis conducted by Dobson DaVanzo & Associates, a healthcare consulting firm. It also found that average total margins for acquired rural hospitals improved from 1.5% prior to affiliation to 2.3% post-affiliation.
Consolidation has provided some rural hospitals the technological infrastructure and back-office functions to participate in VBP, said Waters.
Even though mergers and acquisitions (M&A) slowed in 2025, at least 11 rural hospitals either joined health systems or partnered with another hospital to form a system. Those included:
- Hugh Chatham Health, an 81-bed acute care hospital in Elkin, North Carolina, joined Atrium Health Wake Forest Baptist, which is part of the larger Advocate Health system.
- In Oklahoma, Comanche County Memorial Hospital, a 265-bed rural hospital, announced an agreement to acquire Southwestern Medical Center, 199-bed rural hospital, and form a health system called Memorial Health System of Southwest Oklahoma.
Critical access hospital (CAH). Conversions to CAH’s have increased in recent years and are used by some to garner higher payment rates in exchange for a low number of inpatient beds. Forty-five hospitals have converted to CAH status over the last three years, according to one tracker.
Last year, Fitch specifically cited the CAH status — and the higher Medicare payments that come with that — in supporting Grande Ronde Hospital’s expectation that operating EBITDA margins would hit 9% by the end of fiscal 2026. That would be a big turnaround from the rural Oregon hospital’s 1.9% operating EBITDA margin in fiscal 2025, which was driven by inflation, turnover and elevated expenses from a 2022 expansion project.
Rural emergency hospital (REH). REH conversions are among the most fraught options for local hospital leaders because they provide higher payments but only in exchange for eliminating inpatient services. Forty-three rural hospitals have converted to REH status since January 2023, according to Sheps Center.





