Despite delays, hospitals optimistic on SDPs
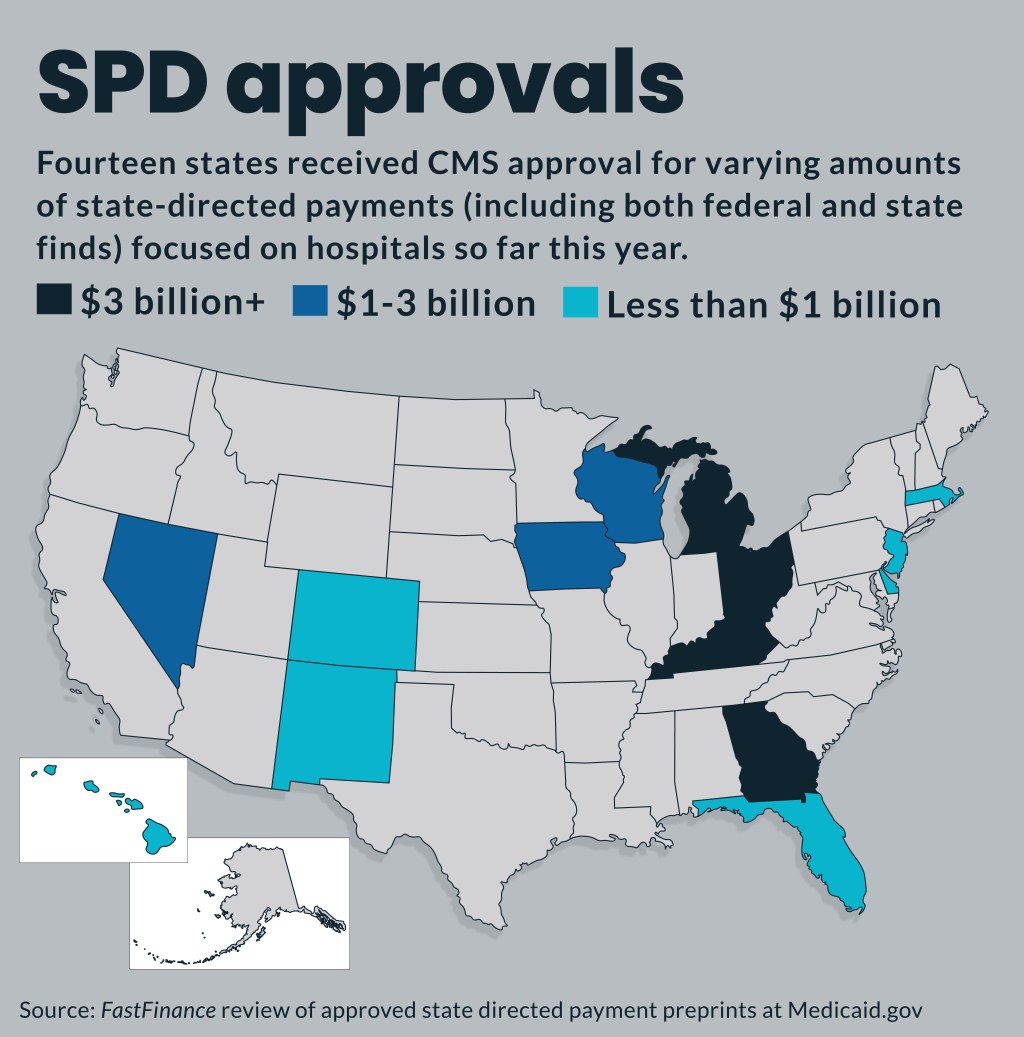
CMS has approved $26.2 billion in hospital-focused state-directed payments so far this year.
Although at least one state has waited nine months for CMS approval of its state-directed payment (SDP) plan, hospital executives said the approval process continues to churn.
So far this year, CMS has approved $26.2 billion in hospital-focused SDPs, according to a FastFinance count of the list of approved SDPs. That amount includes both the federal and state funds included in the SDPs. Those approved preprints range from broad, uniform percentage increases for all hospitals in a state, increases for specific types of hospitals and increases focused on a single hospital.
CMS estimated it will approve about $145 billion in SDPs in 2026 for various provider types. That’s a big jump from $124 billion in 2025.
Florida delay
Florida hospitals have raised increasing concerns in recent months over delays in CMS approval of the SDP the state submitted in May 2025. SDP approvals usually occur within several months of their submission, according to industry observers.
“We’re encouraged by the ongoing dialogue in that state and then again just overall that we continue to see movement in terms of state applications being approved,” Chris Wyatt, senior vice president and controller for HCA Healthcare (HCA), said March 16 at an investor conference.
Kevin Hammons, CEO of Community Health Systems (CHS), said the following day at the same conference that he heard CMS had reached agreement with Florida and a formal announcement was pending.
“Our understanding is they received far more — by multiples — of submissions than they expected and there’s just a backlog,” Hammons said.
CMS did not respond to questions on the status of the Florida SDP. However, the Florida Hospital Association (FHA) said it was not yet approved.
“Florida’s Hospital Directed Payment Program (DPP) for FY 2025 has not been approved by CMS,” Mary Mayhew, president and CEO of the FHA, said in a March 20 email. “The Florida Agency for Health Administration and CMS are close to finalizing a plan that we are optimistic will result in an approval for 2025 and a plan for subsequent approvals.
Many states scrambled to submit SDP applications before the July 2025 enactment of the One Big Beautiful Bill Act (OBBBA) because that law included a range of restrictions on them. Those submitted before OBBBA deadlines were grandfathered in several ways from the law’s cuts.
In February, CMS issued guidance that expanded the opportunity for providers to receive a higher rate of SDP funding over the next two years. The bulletin made it easier for states to maintain eligibility for higher SDPs before OBBBA restrictions start in 2028.
It was unclear why the Florida SDP’s approval was delayed, although some reports stated that it could stem from its program size. The application was for a $7.8 billion SDP, up from $3.3 billion in the previous one, according to media reports.
“While future limits on provider taxes and SDPs apply under [OBBBA], they should not apply to Florida’s proposal submitted before OBBBA’s enactment,” Mayhew wrote in a February op-ed seeking approval of the SDP.
Florida’s Republican congressional delegation also has pushed CMS in recent weeks for quick approval of the application.
2026 SDPs
The latest hospital-focused SDP approvals posted by CMS included six for Georgia for a combined total of $4.5 billion.
Hammons said CHS is expected to garner between $10 million and $15 million from the Georgia SDP.
HCA expects to garner an estimated $83 million from the SDP. However, the for-profit system expected its revenue from SDPs, overall, to decrease from $250 million to $450 million this year due to lower-than-expected CMS approvals of retroactive payments for previous years. However, that expected decrease does not include “incremental” SDPs grandfathered under OBBBA, like the ones from Florida and Georgia, said Wyatt of HCA.
“We’re very happy to see states continue to get approved under this grandfathered construct,” Wyatt said.
Other leading hospital-focused SDPs approved, so far this year, include:
- Kentucky, $5.1 billion
- Michigan, $4.9 billion
- Ohio, $3.9 billion
- Wisconsin, $2.3 billion
- Nevada, $1.5 billion
- Iowa, $1.5 billion
OBBBA impacts
A recently issued analysis by the RAND Health aimed to quantify the impacts of OBBBA on SDPs.
Its findings as of 2025 included:
- OBBBA will adversely affect 24 of the 31 states with active SDPs
- Affected SDPs averaged more than $3 billion in 2025
- SDP Medicaid payment rates varied from 36% to more than 300% of Medicare rates
- Median SDP rate was nearly twice the Medicare rate
The RAND report found South Carolina and Nevada had the highest mean SDP rates relative to Medicare in 2025 — 280% and 251%, respectively. That meant their SDPs face the largest OBBBA cuts as a proportion of their total value.
The largest SDP cuts in dollars will occur in Texas and Tennessee: $19.7 billion and $15.9 billion, respectively, from 2025 to 2034.
The largest reductions in terms of percentage of the state Medicaid budget will occur in Tennessee, Mississippi and South Carolina.
OBBBA’s SDP provisions will cut Medicaid spending by an estimated $241 billion by 2034, including $72 billion in state funds and $169 billion in federal funds.





