Hospitals object to ACA marketplace changes
High deductibles have long been a hallmark of ACA marketplace plans.
Proposed changes to the rules of the ACA marketplaces will shift more costs onto hospitals, industry advocates told CMS.
The comments came in response to a proposed rule for 2027 marketplace plans that aimed to stabilize enrollment from 2026 to 2027.
“Hospitals are often the providers of last resort for many patients, and policies that increase patient cost-sharing or reduce network adequacy often shift uncompensated care costs onto hospitals and health systems that are already under significant financial strain,” Ashley Thompson, a senior vice president for the American Hospital Association, wrote in comments to CMS.
More catastrophic plans
Several proposals would expand catastrophic plans, access to which is now generally limited to enrollees 30 and younger. Older enrollees could qualify for such lower-premium, higher-deductible plans through a broadened hardship exemption if they don’t receive subsidies for premiums or out-of-pocket costs.
Such plans could increase deductibles to as high as $15,500 for individuals and be automatically renewed for as long as 10 years. CMS also proposed allowing bronze plans to increase their cost sharing above statutory maximum out-of-pocket limits.
“Rural hospitals or other providers may not be able to collect payment from rural patients with catastrophic or bronze plans because the individuals cannot afford to pay their bills, leading the facility to take on uncompensated care costs,” Alan Morgan, CEO of the National Rural Health Association, wrote in submitted comments. “Ultimately, this becomes a bad debt for the rural hospital or other provider.”
Concerns that the proposed changes would drive increases in bad debt was a common concern among hospital advocates.
America’s Essential Hospitals (AEH) stated that uncompensated care among its member hospitals had reached $11 billion in 2023. And the Catholic Health Association (CHA) noted that member hospitals had more than $25 billion in bad debt in the latest reporting year.
New increases in uncompensated care would come on top of a recent surge in those costs. Year-to-date 2026 bad debt and charity per calendar day is 40% more than year-to-date 2023, according to the latest Kaufman Hall hospital flash report.
“CMS should require robust monitoring and transparent evaluation of the impacts on delayed care, medical debt and hospital uncompensated care,” Lucas Swanepoel, JD, a vice president of CHA, wrote in submitted comments.
Out-of-pocket trend
High deductibles have long been a hallmark of ACA marketplace plans. In 2025, the average deductible was $4,902 for silver plans and the average deductible was $7,186 for bronze plans, according to the Peterson-KFF health system tracker. In 2026, average deductibles increased to $5,304 for a silver plan and $7,476 for a bronze plan.
Those out-of-pocket costs increased in 2026 after Congress allowed COVID-era extra subsidies to expire.
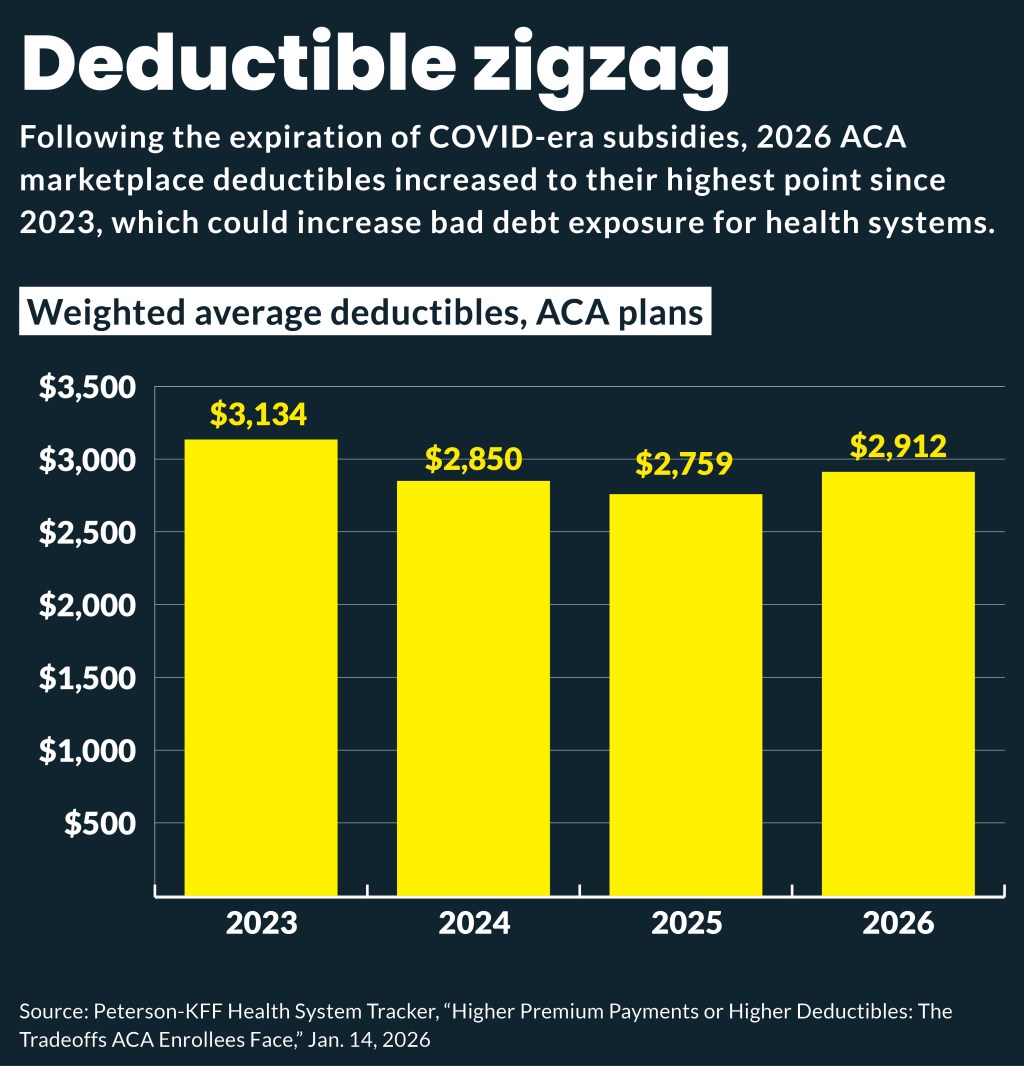
But even when out-of-pocket subsidies were considered, deductibles remained high. The weighted average deductible — including subsidies — across all plans was $2,759 in 2025 before it increased to $2,912 in 2026, according to the tracker.
Any increase in out-of-pocket costs also could exacerbate losses that some health system executives have reported previously from ACA-covered patients who didn’t pay their share of their hospital bill.
Kevin Hammons, CEO of Community Health Systems, told investors in January that ACA marketplace enrollees mainly use the system’s emergency departments and often don’t pay their deductibles or co-insurance.
Network changes
Among a range of proposed network changes, CMS proposed to permit “non-network plans” on the marketplaces and detailed how they could achieve qualified health plan status. Such plans may include those that use reference-based pricing.
Hospitals warned that such plans may provide “illusory benefits” if few healthcare organizations would provide services for its offered payment rates.
“Even if a non-network plan has low premiums, it may not provide meaningful access at the point an enrollee actually requires care,” Charlene MacDonald, president and CEO of the Federation of American Hospitals, wrote in submitted comments.
MacDonald also questioned whether such plans violate federal law.
Enrollment cuts
CMS projected the rule’s changes will lead 1.2 million to 2 million enrollees to drop their ACA marketplace coverage in 2027. Twenty-three million enrollees selected coverage in 2026, although it was not yet known how many effectuated that coverage by starting to pay their premiums. The initial decrease of more than 1 million enrollees in 2026 was substantially less than the more than 5 million decrease this year projected by the Congressional Budget Office if the COVID-era subsidies expired.
Still, hospital advocates urged against finalizing measures in the proposed rule that don’t prioritize preserving coverage.
“Absent such modifications, people could lose access to needed healthcare,” Swanepoel of CHA wrote. “Our members will continue to serve patients. but these enrollment losses will predictably increase uncompensated care, emergency department utilization and financial pressure on hospitals serving as essential safety-net providers.”
Democrat plans
Congressional Democrats have focused on ACA marketplaces in their healthcare pitch to the electorate for the upcoming midterm elections.
Senate Democrats have offered a somewhat vague plan to enact a range of policies, including reinstating COVID-era subsidies for the ACA marketplaces and ban short-term limited-duration plans expanded by the Trump administration.
It also included plans to offer “Medicare-type choices for healthcare,” which could mean creation of so-called public option plans on the ACA marketplaces. Congressional Democrats have previously failed to push such plans through Congress, even when they had large majorities.
“Republicans have spent the past year making these problems worse by passing the largest healthcare cuts in history and pursuing administrative actions that further destabilize health insurance markets,” the Senate Democrats wrote.





