Growth projects lead amid reduced capex
Forty-one percent of hospitals and health systems will cut capital spending, while 31% plan to increase it.
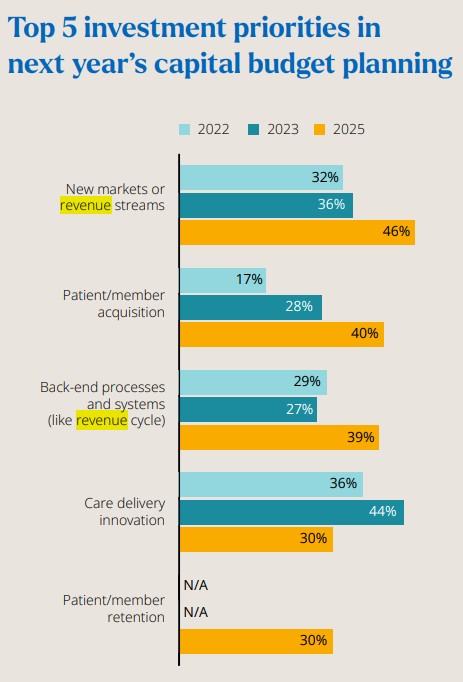
Even as health systems reduce their capital investment, they’re focusing greater shares of funds on expansion efforts, according to a recent survey.
Health system and hospital capital investments are declining and few are expecting significant increases in the next two years, according to a Sage Growth Partners survey of 101 health system and hospital executives.
Capital investment spending planned for 2026 includes:
- Cut of 20% or more — 19%
- Cut of 10% — 22%
- No change — 19%
- Increase of 10% — 17%
- Increase of 20% or more — 14%
Factors driving the overall decrease in capital spending include tight margins driven by elevated labor and supply costs and tighter rate increases, Dan D’Orazio, CEO of Sage Growth Partners, said in an interview. Adding to pressures are increased borrowing costs and looming Medicaid cuts under the One Big Beautiful Bill Act.
“[We’re] at a point where everyone keeps saying, ‘This can’t continue,’ [and] employers are getting highly frustrated [as] the price of healthcare keeps going up,” D’Orazio said. “And so, the pressure is coming from a lot of places.”
Capital investment priorities
Overall, revenue growth initiatives are the leading priority for 2026 capital budgets. That includes 46% of C-suite leaders prioritizing initiatives to target new markets or revenue streams. That was up from only 36% prioritizing those investments in 2024.
Additionally, 40% are prioritizing initiatives focused on patient/member acquisition, which is up from only 28% doing so in 2024.
D’Orazio sees those two priorities as interrelated, as policies and payments pushing care out of hospitals come together with patient preferences for better access and convenience.
“We’re seeing slight, sort of, engagement in consumerism — healthcare is not a very consumer market — it’s very challenging,” D’Orazio said. “But people want to be in better places. They don’t want to be in the hospitals.”
Also taking on increasing capital budget planning importance are back-end processes and systems like revenue cycle, which 39% are prioritizing — up from 27% in 2024.
A decreasing priority for capital budget planning is care delivery innovation (30% in 2026 versus 44% in 2024). That caught D’Orazio’s attention because care delivery innovation is sorely needed.
“As payment moves from inpatient to outpatient — hospital outpatient to ASC, site neutrality — I think care is going to be innovated, maybe driven by the dollar, unless [it is driven] by the clinical model,” D’Orazio said.
Technology initiatives
AI-based clinical technology solutions led among health system’s planned technology initiatives, with 57% planning such spending in 2026 and 2027, up from only 19% in 2024 and 2025.
“One of the most powerful areas we’ve seen work are the ambient [listening] solutions,” D’Orazio said. “I’ve heard time and time again, ‘The doctors can look at their patients, they spend more time with their patients, they’re not looking at the computer.’”
In a given week, physicians using AI scribes spent 13.4 fewer minutes on electronic health records (EHRs), 16 fewer minutes on documentation, and delivered 0.49 additional visits, according to recent research in JAMA.
In contrast, the share planning to spend on optimizing their EHR dropped to 43% from 60% in the last two years.
AI-driven administrative solutions also are an emerging focus, with 29% of health systems planning to spend in that area, up from just 6% in the last two years.
Plans to spend on revenue cycle solutions was more stable, with 37% planning such spending, compared with 32% such spending plans in the last two years.
EHR lessons for AI
The massive costs and extensive operational challenges of healthcare’s EHR implementation over the last 15 years offer important lessons for the ongoing adoption of AI technology, said D’Orazio.
“The technology is only ever 20% to 30% of what is going to determine success,” D’Orazio said. “Process and people are absolutely the drivers.”
That reality is likely to drive large failures in enterprise wide AI deployment because organizations are not first focusing on governance, data integrity, data quality and workflows.
“We have to be really mindful because AI has the power to make things happen fast,” D’Orazio said. “And in many ways, they could make things worse if we’re not really thoughtful.”
ROI focus
Executives have shifted toward rigorous business-case justification, prioritizing clear and measurable financial returns, as part of their digital health purchasing process, according to the survey.
The most critical factor in purchasing decisions for 77% of respondents was the anticipated ROI, up from 50% prioritizing that in the previous survey.
Other digital health purchasing priorities for executives included:
- Cost, 72%
- Integration with EHR, 68%
- Breadth of functionality, 58%
Additionally, hospital and health systems are interested in more predictable pricing options: Monthly or annual contracts are currently the top preferred model, according to the survey.
“If someone were to say, ‘Hey, look. I’m going to generate all this value for you and maybe I’ll keep some of it,’ that’s far over on the other side of what people want. They want predictability,” D’Orazio said.





