Mystery Markups: Medical Supply and Drug Pricing Policies Vary Across Hospitals
In general, medical supplies and pharmaceuticals represent 20 percent of gross charges. Even the slightest change in markup policies could have enormous financial impact.
Charging for medical supplies and pharmaceuticals is a complex process that differs from other areas in chargemaster and billing systems. Understanding whether charges are high or low and what impact changing processes might have presents challenges for healthcare finance leaders.
A large national survey of hospital billing policies and practices reveals how hospitals charge for supplies and pharmaceuticals and offers insight on ways to effectively evaluate charge changes.
Charge Structure
Most hospitals use markup policies based on costs (or a derivative of costs) to set prices of supplies and pharmaceuticals. Our survey results show that these markup policies can vary significantly across the country, leading to large variances in drug and supply charges.
Medical Supplies
For the purposes of analyzing the data set, we created eight tiers based on cost from a national sample consisting of more than 250 hospitals. However, we learned from the individual markup policies we received that hospitals utilize anywhere from one to 55 markup tiers. To clarify, hospitals with one tier would price all items—regardless of cost—with the same ratio, whereas hospitals with 55 tiers would frequently adjust ratios based on different ranges of cost. The average number of tiers is seven.
In addition to standard supply markups, we found that nearly 50 percent of providers maintain separate schedules for implants. As medical supply costs increase, markup factors decrease. However, the lowest-cost tier (items costing less than $5.01) deviates from the linear progression. These low-cost supply items could represent patient-sensitive areas in the chargemaster. As a result, many providers may be charging differently—or not at all—for them. Anecdotally, we can affirm this observation based on conversations with providers who want to either reduce or eliminate charges for routine supplies.
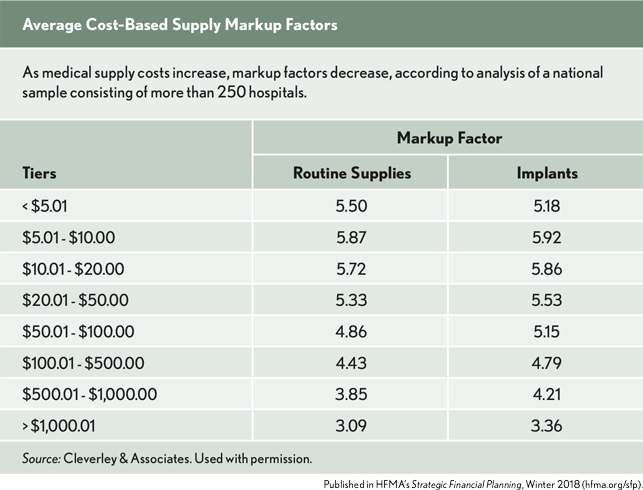
Implant markups mimic the same relationship in that as cost increases, markups decrease. While it is difficult to imagine a $5.00 implant, most provide charging logic to cover any possible item so that charges will always occur.
Pharmaceuticals
The markup policies of drugs often differ from that of supplies in that they are based on either average wholesale price (AWP) or some form of cost-based methodology, such as wholesale acquisition cost (WAC). In our survey, we discovered about equal usage of AWP and WAC. There has been some momentum to change from AWP to WAC because some sources of AWP have been discontinued. However, Red Book® actively publishes average wholesale prices for brand name and generic drugs so hospitals that want to maintain their current platforms can do so from that source.
To analyze the data set for drug markups, we constructed six tiers based on cost, although the number actually ranges from one to 30 tiers. Pharmaceutical markups parallel the linear progressions observed in supply markups.
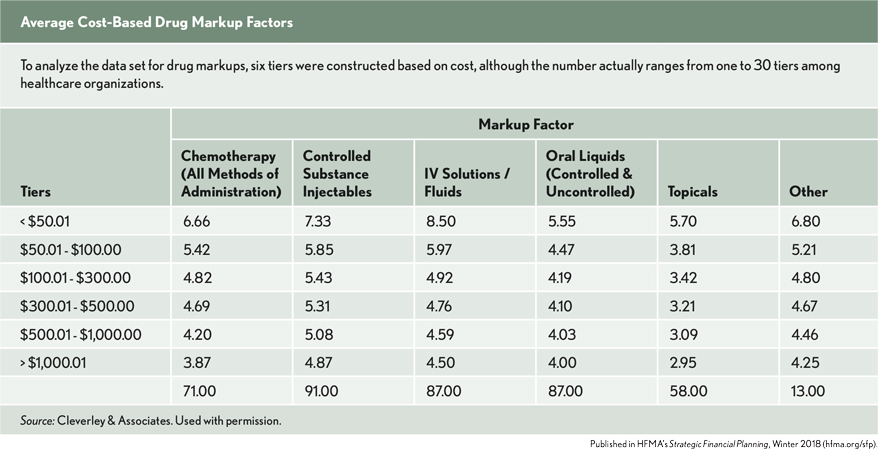
Our research indicates that many hospitals use various markup methodologies for different drug categories. The main categories are chemotherapy, controlled substance injectables, IV solutions/fluids, oral liquids (controlled and uncontrolled), topicals, and other.
It is likely that hospitals use these different categories and unique markup methodologies to provide greater flexibility in pricing different drugs. Interestingly, oral liquids and topicals appear to have the lowest markup factors. We would have expected chemotherapy drugs to have a lower markup compared with other pharmaceutical categories due to their high costs, but that is not an observable relationship. Unlike supplies, drugs included in the lowest-cost tier appear to follow a regressive structure for the markup policy. We found this interesting because we have had conversations with numerous hospitals about reducing charges for low-cost drugs.
Charge Dynamics
Our research found two primary methods of charge practice: hardcoded and dynamic. In the hardcoded approach, prices are established at initial entry into the chargemaster and then changed periodically by a flat percentage to account for inflation. Hardcoded prices can get disconnected from cost/AWP relationships, and margins may erode if the costs used to determine patient charges do not accurately reflect hospitals’ current costs. However, hardcoded prices have the benefit of providing greater certainty during revenue budgeting.
On the other hand, dynamic prices change when the underlying cost or AWP changes. These changes can occur frequently—even daily—or at predetermined times (e.g., quarterly, annually). The benefit of dynamic pricing is that it reflects the most current cost, which helps maintain margins for items with rapidly increasing costs (e.g., chemotherapy drugs). However, hospitals can experience greater revenue fluctuation from budgeted amounts.
Case Study: Charge Change
To test the connection between policy and actual claim charge data, we compared the markup policies we received to detailed Medicare claims data. Then we examined the markup relationships for a hospital employing a high markup structure and for a hospital employing a low markup structure.
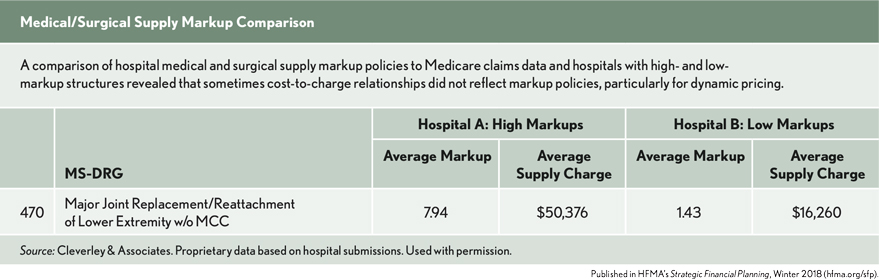
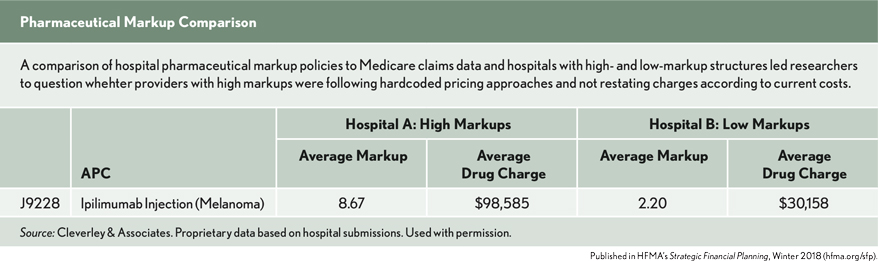
During our review of policies, corresponding costs, and charges, sometimes cost-to-charge relationships did not reflect current markup policies, particularly for dynamic pricing. In these instances, we wondered whether providers were following hardcoded pricing approaches and not restating charges according to current costs. The other possibility seems unlikely—that their costs were substantially lower.
Charge Policy Changes
Finally, we considered the implications of changing charge policies. For example, what would the implications be for hospital A to reduce its markup and prices to better compete with hospital B, or vice versa? Three major areas need to be carefully evaluated prior to executing markup revisions.
Gross charges. In general, medical supplies and pharmaceuticals represent 20 percent of gross charges, and as a result, even the slightest change in markup policies could have enormous financial impact. Prior to converting markup methods or executing new markups, hospitals should model impacts to gross charges.
Net revenue impact. Each item in the chargemaster has an individual recovery rate. Recovery is defined as the change in net revenue that results from a change in gross charges based on payer mix and payer terms for those services. High charges do not necessarily correlate with high payment. Performing a scenario analysis can help hospital finance leaders better understand overall payment and net revenue impacts prior to implementing changes. Drugs and supplies can have carve-out language in many commercial contracts—especially for high-cost drugs and implants—that can result in significant net revenue changes if markup relationships are altered.
Data complexities. When modeling markup policy changes, it is essential that the details used in data modeling tie to policies and billing systems. Often, there are additional layers of detail hidden behind the chargemaster—especially for drugs—which can complicate impact modeling. For example, one charge code in the chargemaster can have multiple national drug codes, each of which may map to different markup tiers. In addition, in many billing system environments, “shell codes” are used in chargemasters to represent a multitude of individual drugs and supplies. The key is to identify which markups are applied to derive current and proposed charges.
Viable Charge Models
The billing methodologies for medical supplies and pharmaceuticals are complex and continually changing, and a one-size-fits-all method does not exist. However, healthcare finance leaders can compare their charge positions for these critical areas and determine whether changes are needed.
Although changes can be complicated, they can be successfully implemented with a full understanding of the related elements and implications. The benefits of those changes can yield a more competitive and financially viable model for patients and providers.





