4 essential tactics for sustaining an independent community hospital
Independent community hospitals in the United States are not endangered species. But they are threatened, and their survival as independents depends on the deliberateness of the actions they take now.

Many independent community hospitals are in a precarious position, with almost 40% of these organizations having recorded a negative operating margin in their most recent cost reports. They also have suffered a mounting financial toll from the pandemic, which has only heightened the urgency and caused executives and governing bodies of many of them to question the viability of remaining independent.

There are exceptions, however. In the midst of record hospital closures and post-pandemic financial distress, some community hospitals have managed to achieve financial sustainability and, in some cases, to thrive. Results of recent interviews with more than 100 executives from leading independent community hospitals provide valuable insight into what these successful community hospitals are doing to create durable independence.a These hospital leaders shared four essential tactics, described in this article, which other community hospitals that want to remain independent can incorporate into their planning to bolster their autonomy.
When independence is the best path forward, leading hospitals’ strategic plans leverage the following tactics to ensure independence is sustainable.
1 Collaborate to create virtual integrations
Throughout the interviews, many leaders referred to their organizations as “fiercely independent.” But paradoxically these same hospitals maintained their independence by relying on others. The case for health system integration frequently rests on the ability to achieve scale, but successful independent organizations have been able to partner to create virtual integration without sacrificing their autonomy.
To explore virtual integration, leaders need to prioritize areas that can deliver value to all participants without forcing any party to risk its competitive position. Such collaborations often begin in non-clinical and administrative functions.
For instance, independent community hospitals in Arkansas banded together to form the Arkansas Rural Health Partnership to find scale through shared staffing agency support, shared laundry and linen services and robust provider workforce pipeline, all without giving up a single board seat to a health system.
Independent hospitals also need to find ways to make up for their lack of other advantages enjoyed by health systems. For example, in addition to administrative service partnerships, health systems can partner with national vendors to bring scale to programs that may not otherwise be possible in certain markets. Consider the challenge of establishing an accountable care organization (ACO). For an ACO to deliver on its transformative promise, it first must achieve a meaningful number of covered lives to mitigate the risk.
This can be a prohibitive challenge for a small independent organization in an area of limited population density. However, by partnering with organizations like Caravan Health, Kansa City, Missouri, independent organizations can achieve the same scale as their larger health system colleagues by banding together to create access for their patients locally.
Lynn Barr, the founder of Caravan Health, says these strategies can extend the reach and bench strength of independent hospitals. According to Barr: “Independent hospitals frequently don’t have the expertise, IT infrastructure, risk capital or even enough patients to participate on their own in these programs and achieve consistent, successful results. By joining together, they can reduce their costs and increase their performance.”
2 Adopt practices of high-performing community hospitals to optimize staff recruitment and retention
Independent hospital leaders from nearly every state said the future of staffing their organization was among their greatest concerns. The state of Mississippi alone has seen at least 2,000 nurses resign since the beginning of 2021.b
For community hospitals, remaining independent depends on the ability to recruit and retain staff, and the best strategies going forward will creatively transform how many of them approach their workforce.
For clinical staff and providers, the focus should begin with retention. Since 2016, the average hospital has turned over 90.8% of its workforce at a staggering cost.c
Among independent hospital leaders interviewed, those whose organizations had lower turnover underscored the need for an unrelenting effort to reduce the pain points for staff at work by implementing flexible roles, self-scheduling, burnout reduction efforts and competitive pay practices. High performers also have focused on enhancing the capabilities of their managers and leaders through training and leadership development. These initiatives create value in the longer term, but because they require increased investment in the near term, they must be accounted for in any strategic planning initiative.
Many organization leaders also said they are considering ways to transform their overhead departments to reduce cost. To allow for more work-from-home options, it’s necessary to rethink back office to better incorporate a remote workforce. Such changes can reduce the time to recruit new staff by allowing a hospital to cast a much broader net, and they also drive down costs by allowing organizations to consolidate their physical office space over time.
For difficult-to-recruit team members in highly technical areas such as IT or finance, many community hospitals have considered partnering with new entrants like Amazon or others to outsource key back-office functions.
3 Seek broader opportunities to access capital
It is often said that you have to spend money to make money. In the case of independent hospitals, it is clear that those that have stronger balance sheets have a greater ability to replace routine capital, update facilities and equipment and execute strategic investments.
Given that nearly 40% of the independent hospitals have recorded a negative operating margin, many of these organizations apply slim operating cash flows to fund operations and often neglect routine capital and other critical capital needs. Over time, facilities and equipment begin to age, leaving organizations less able to stay current with service delivery advancements in the market, which hampers their ability to retain a long-term patient base.
To meet this challenge, some independent private hospitals are strategically transforming their governance model into a public authority to gain access to tax-based funds, resources and, in some cases, access to capital through municipal debt financing.
Lakeland Community Hospital in Haleyville, Alabama, for example, converted its governance model from a private hospital to a public county health authority, making the city and county authority the owner of the hospital with a separate management structure operating the organization. This move allowed them to employ a $0.01 sales tax and a county property tax increase to fund both short-term and long-term strategic and capital needs. Although the hospital relinquished private control, it was able to remain a community asset, independent from any large health system and under control of the community, which had a strong interest in keeping the organization locally independent.
Small independent hospitals that have difficulty gaining access to capital through conventional avenues — such as bank-qualified loans with local or regional banks as well as from HUD or other federal and state programs — have explored pooled loan arrangements with other organizations in similar situations. Not as common as other loans, credit enhancements backed by local or state authorities help raise ratings and lower borrowing costs for hospitals participating in a pooled arrangement, thereby helping improve access to capital for hospitals participating in the pooled loan.
4 Engage the hospital’s workforce and community to create and drive strategy
A hospital’s ability to maintain independence is highly reliant upon its having a tight alignment with its workforce and, more broadly, with the community that it serves. Employees and local community members are more likely to be engaged if they feel a sense of ownership with a hospital, which is why it is essential to open up the strategic planning process for input beyond the C-suite and the board and make strategy real for every level of the organization.
One possible option to develop an “open strategy” process, in which employees and the community are invited to provide input. For example, the hospital could create disease-specific focus groups to gain insight into how patients would like from the hospital providers to deliver their care, or it could involve employees to vote on elements of the strategic plan.
A good place to start is by revisiting the community health needs assessment (CHNA) in light of the pandemic. Many organizations have continued to look to their pre-pandemic CHNA when developing their strategy, but this approach does not recognize how their communities’ needs and expectations have changed since early 2020.
Regardless of how a hospital chooses to partner with its workforce and community in the strategic planning process, success rests on creating ownership for strategy at every level of the organization. One of the greatest differentiators between a high-performing independent hospital and its peers is its ability to translate visionary strategic statements into tactics that can be easily understood, implemented and measured by front-line leaders.
Consider the experience of Hill Country Memorial Hospital in Fredericksburg, Texas. Hill Country Memorial has been recognized as a Malcom Baldrige National Quality Award winner and has vigorously aligned its workforce, processes and strategic goals to create a culture of high performance.
Jayne Pope, CEO of the hospital, said, “We know our patients won’t come here [if we don’t have] an A+ scorecard and the very best service, and so that is our priority.”
Creating that culture has taken deliberate efforts to cascade vision into the workforce goals.
Amanda Stevens, chief strategy officer at Hill Country Memorial, points out just how structured their approach to strategy is and how it translates to results. “We carry our goals down through our alignment boards at the department level and into the front-line team members who have their own strategic coaching plan,” she says. “We take it zone by zone across the organization, and in aggregate, it has a significant impact.”
Maintaining independence is about sustaining value
Independent community hospitals play an essential role in the nation’s healthcare system in ensuring the unique needs of every community in the United States are met fully and appropriately. By remaining independent, these hospitals can ensure that they continue to fulfill this important role. But maintaining independence will require a strong commitment to excellence and diligence in pursuing the four essential tactics described here.
3 core capabilities needed for maintaining independence as a strategic asset
Independence is a compelling choice for a community hospital because it can allow for a self-determining strategy. There are fewer levels in an organizational chart between leadership and the front lines, and quite often, there is an even smaller distance between the front lines and the communities that they serve.
Conversely, when a community hospital is part of a health system, the priorities of its community must be balanced within the needs of an often geographically and socioeconomically diverse portfolio of hospitals. As a result, capital and services may end up being focused elsewhere.
Ultimately, some community hospitals may conclude that they have no choice but to join a larger health system to be able to continue serving their community mission. But other hospitals will continue to see their independence as an invaluable asset that must be protected throughout their strategic planning process.
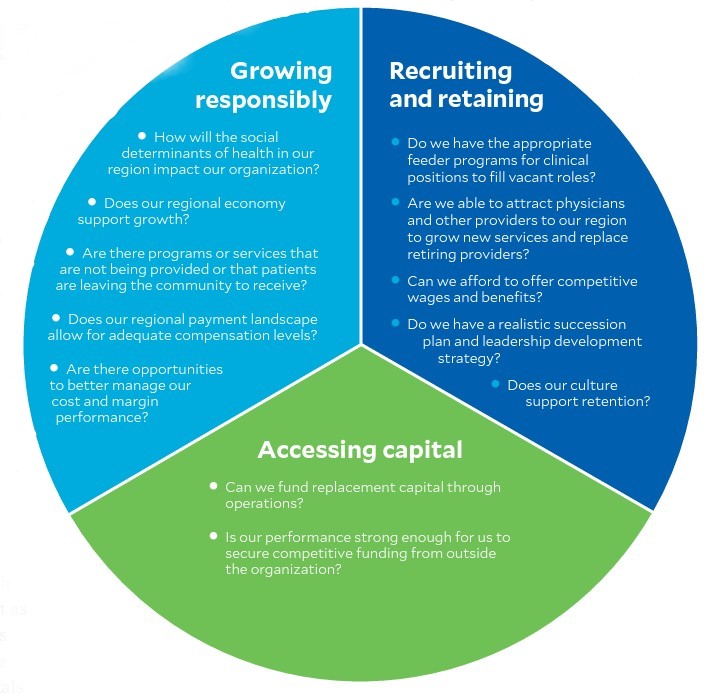
These hospitals can succeed only if they understand the three core capabilities necessary to retain independence and develop a strategic plan that closes the gaps and solidifies these competencies. Simply put, as shown in the exhibit below, the hospitals must address key questions that determine the extent of their core capabilities in three areas:
- Growing responsibly
- Recruiting and retaining physicians and other providers
- Accessing capital
Core capabilities community hospitals require to maintain independence
Footnotes
a. The interviews were conducted by the authors throughout 2021.
b. Holcombe, M., Hill, E., Dolan, L., “‘I think we already broke’: Mississippi’s nurses are resigning to protect themselves from Covid-19 burnout,” CNN, Aug. 25, 2021.
c. NSI Nursing Solutions, Inc., 2021 NSI National Health Care Retention & RN Staffing Report, March 2021.





