Over the past few years, our nation has seen an intensified focus on health equity. Spurred in part by the pandemic, which laid bare the vast human cost of remediable health disparities, both civil society and government are increasingly focused on improving health equity. So are healthcare organizations themselves, many of which are launching or planning to launch new health-equity initiatives.
For many of these organizations, investing in health equity is a new endeavor that poses a new set of planning, budgeting and operational challenges. As each organization proceeds, it will be embarking on a unique journey shaped by its regional markets, consumer dynamics and internal culture. Yet every organization will have to pass common milestones along the way.
Preparing for the journey
Any successful journey requires adequate preparation, especially when the terrain to be traversed is challenging and unfamiliar. Before embarking on the health-equity journey, organizations should take four preparatory steps.
1 Identify opportunities and set goals. As with any business venture, the place to start is to identify opportunities and set goals. Health-equity initiatives should always be based on an assessment of unmet needs in the community, and they should build on proven strengths of the organization. They should also include concrete health and ROI goals toward which the organization can measure progress.
2 Review analytic capabilities. Before an organization embarks on the health-equity journey, it should conduct extensive analysis to determine which types of initiatives identified in the first step seem most promising. Once an initiative is launched, the organization will need to assess the extent to which it is meeting health and ROI goals. It therefore is imperative that the organization review its analytic capabilities prior to launch, and if necessary, upgrade them.
3 Forge external partnerships. Successfully carrying out most health-equity initiatives will require forging ongoing relationships with external partners. These partners may include nonprofit foundations, which can collaborate in designing the initiatives and provide funding. They will almost certainly include nongovernmental organizations (NGOs) operating in the community. All potential partners should be carefully vetted to ensure that they possess the relevant capabilities and are trusted in the community.
4 Forge internal partnerships. At least initially, health-equity initiatives will need to lean heavily on the resources and capabilities of the rest of the organization, including existing personnel, operational systems and digital platforms, even if they are not a perfect fit. Ensuring that this support will be forthcoming is critical.
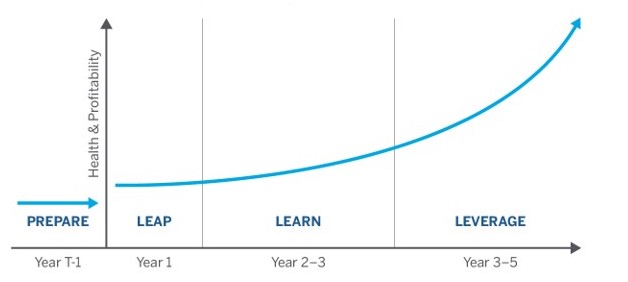
It is helpful to conceive of the health-equity journey as comprising three stages. We call these stages the “Three Ls,” which stand for “leap,” “learn” and “leverage.” Progressing from stage one to three will typically take three to five years.
The three Ls
Leap (year 1). The journey normally begins with the launch of one or more pilot projects. Although such a step inevitably involves a leap of faith, it need not be an uninformed one if adequate preparations have been made.
Learn (years 2 to 3). Clearly, learning begins the moment that pilot projects are launched. But it accelerates once organizations have collected and analyzed sufficient data to determine what is or is not working. During this learning stage, which should be reached by the second year of the health-equity journey, organizations will be able to refine their pilot projects to better meet the needs of patients and members. Even as they learn more about the demand side, they will also learn more about how to manage the supply side efficiently, thereby reducing unit costs. Along the way, they will begin to better understand personnel needs, allowing them to add dedicated staff, as necessary. They will also begin to better understand their IT needs, allowing them to customize their digital platforms.
Leverage (years 3 to 5). The final stage of the health-equity journey, normally reached in the third or fourth year, is all about leverage. During this stage, organizations should close down unsuccessful pilot projects and scale up successful ones to larger populations and/or new geographies. By this point, the fixed costs incurred in launching successful projects will likely have been recouped, allowing profits to fund additional growth. Operational systems, job descriptions and digital platforms should also have been standardized. In short, health-equity initiatives will have developed into their own sustainable business lines.
The health equity journey
Pitfalls and payoffs
There are many pitfalls to avoid on the health-equity journey. Organizations will need to carefully vet their external partners, whose core capabilities should complement rather than compete with their own. They will also need to resist the temptation to jump to the leverage stage too soon. It takes time to know with confidence which pilot projects are worth scaling up and which should be closed down.
Finally, organizations should accept that they cannot do everything. Although it makes good sense to start with an array of pilot projects that address a broad spectrum of needs, once an organization has discovered what it does best, it should specialize. By trying to do everything possible to advance health equity, an organization may end up doing nothing well.
Yet if the pitfalls are many, the potential payoffs are large. There is of course the satisfaction of knowing that lives have been improved and injustices redressed. But along with this satisfaction, there will also be tangible business benefits, including the direct financial ROI from pilot projects that are successfully scaled and the indirect ROI that can flow from enhanced brand appeal and improved employee engagement.
Above all, a healthcare organization can obtain important strategic benefits from promoting health equity. It ensures that the organization is will keep pace with an America that is becoming more diverse and is increasingly focused on eliminating health disparities. And it will also ensure that the organization remains aligned with the ongoing transformation of our nation’s healthcare system as it continues to move inexorably toward value-based payment arrangements.
Initiatives organizations should consider
Following are examples of the types of health-equity-focused initiative a healthcare organization might want to pursue.
Community center clinics. An organization could establish clinics at community centers in underserved neighborhoods. Bringing healthcare to where people already are, as opposed to requiring them to come to the organization, can increase appropriate utilization of services and result in better health outcomes.
Food-as-medicine programs. By creating food-as-medicine programs in neighborhoods where nutritional needs are high, an organization can help prevent, manage and treat chronic illness. Such programs also provide opportunities for dieticians and case workers to have regular interactions with patients that may suggest the need for additional health interventions.
Nonmedical benefits. Lack of affordable transportation and childcare are major barriers to access for underserved populations. Organizations could provide shuttle services for nonemergency health visits, as well as to meet additional patient needs such as prescription or grocery pickups. They could also provide back-up childcare services on site.
Community health training programs. An organization could create programs to train community health workers and patient navigators, who would be tasked with identifying unmet needs in the community and then referring people to appropriate medical and nonmedical resources.
Editor’s note: This column shares results from an ongoing research initiative by the Terry Group, Health Equity Strategies, which is aimed at helping healthcare leaders play a more active role in improving health equity across the nation.





