Leaders share experiences and insights in launching healthcare consumerism initiatives in today’s dynamic environment.
Healthcare organizations that embrace healthcare consumerism and are proactive in adapting to better meet patient needs are more likely to succeed in their initiatives than those whose consumerism efforts are more patient- or market-driven, a survey of healthcare finance leaders shows.a
According to the survey, cosponsored by HFMA and CareCredit, a Synchrony solution, the top three priorities for consumerism initiatives launched by hospitals, health systems, physician practices and ambulatory centers are to:
- Identify, hire and train the best staff
- Identify and implement the best technologies
- Understand and justify the additional costs associated with consumerism
Lower-ranked priorities included efforts to define and implement operational support, identify financing and reassess or reprioritize existing projects to focus more on consumerism.
The survey of 178 HFMA members, primarily directors and CFOs in finance and patient financial services, conducted in February and March of 2020, shows that the higher consumerism priorities rank in an organization, the greater the chances of success in these areas. Survey respondents say they have demonstrated the greatest success in implementing technologies that improve the consumer experience. This is followed by gains made from identifying the best staff for consumerism-focused programs and understanding and justifying the costs associated with these plans.
“The survey clearly shows that technology plays a crucial role in creating positive consumer experiences,” said Tim Donovan, chief marketing officer, CareCredit. “In a matter of months, companies have accelerated advancements in healthcare technology and digitization to respond to needs highlighted by the pandemic that otherwise may have taken years to gain traction. And now that consumers are more familiar with contactless ways of working, from virtual visits and digital patient portals to online payments, there’s no sign they’ll stop seeking these conveniences — in fact, they’ll likely expect more.”
Likewise, respondents that place a low priority on finding the right technologies to support consumerism priorities were likely to report poor success around the patient experience, transparency and engagement (see the exhibit below).
Comparing consumerism priorities with organizational success
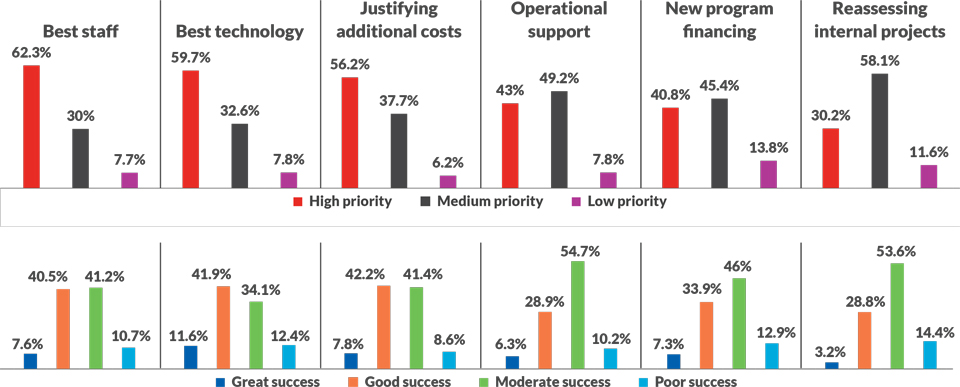
Source: CareCredit Healthcare Consumerism Survey, conducted by HFMA, February 2020
What do healthcare leaders view as the key contributors to creating a consumer-centric organization — and what stands in the way of success? Here, survey results and market leaders point to three factors.
1. A proactive versue reactive consumerism strategy
Leaders in creating a consumer-centric model of care and service say they take a proactive approach to improving the patient experience, according to the survey. Most or all of their efforts are driven by a desire to improve, rather than a reaction to patients’ demands or market requirements — and this strengthens their success. Some outcomes are:
- 53% of organizations whose consumerism efforts are mostly proactive report good or great success with their initiatives, compared with 32% whose work is mostly reactive.
- 43% of respondents report a balanced approach — an equal combination of proactive and reactive response to patient or market demands — that generates good or great success.
“We like to be ahead of the curve,” said Katherine Cardwell, vice president, revenue cycle, Ochsner Health, a 40-hospital system based in Louisiana. “We work hard to understand consumer expectations, anticipate patients’ needs with actionable analytics and focus on high-impact ways to optimize the patient experience.”
In 2018, Ochsner Health created the role of senior vice president of consumer strategy to continue the organization’s focus on developing new capabilities around patient access, billing transparency, care navigation and service excellence while strengthening digital connectivity. A consumer strategy committee meets biweekly to propose innovative ways to meet patients’ needs and develop, launch and assess the organization’s best ideas, including:
- A price estimator tool that provides cost estimates for more than 200 shopped services (the system’s goal: estimates for more than 300 services), available through the Ochsner website and patient portal
- A new partnership with a digital health startup that serves as a unique digital front door to the health system, connecting consumers with high blood pressure or diabetes with Ochsner’s digital medicine program
- “InnovationHubs” that provide access to health and wellness information and introduction to new care delivery options in high-traffic retail locations, with stations to sanitize cellphones and the opportunity to evaluate and purchase remote monitoring devices
- An “Optimal Hospital” that adjusts nighttime care routines to lessen disruptions in sleep — resulting in a shorter length of stay (8.6 hours) and a 16% reduction in 30-day readmission ratesb
Visioning and executing on a three-year road map to optimize the digital front door and simplify navigation, with an emphasis on providing patients with the information they need to effectively schedule and prepare for a visit via live chat.
The committee includes representatives from across the system, including finance.
During the first months after the coronavirus outbreak, Ochsner’s proactive mindset around improving the patient experience positioned the health system to respond with agility to a changing environment.
“We understand our patients’ need for additional safety measures when returning for in-person care, so we provide both digital and non-digital options for low-contact arrival for our patients. These options allow patients to check in from and wait in their car or another location until we are ready to start their appointment,” Cardwell said. “Digitally, patients utilizing our patient portal app are prompted on their smartphone to check in when they arrive on campus. For patients who do not utilize the digital check-in, we have posted signage in our parking areas that provides information on how to call us when they arrive to be checked in over the phone. We also instituted virtual lobby rounding, the ability to reach out to patients while they wait and provide updates and reassurance. This helps avoid or deescalate patient frustrations.”
Proactively exploring innovation from a number of angles bolsters Ochsner’s ability to provide care the way patients want it, when they want it. “The strength of our consumer strategy is that we are providing options for our patients based on their expectations and preferences,” Cardwell said. “We’re continually looking at new opportunities to reshape the patient experience and provide increased value.”
2. Setting priorities for consumerism investment
The research showed that organizations that most effectively supercharge their consumer experience are more likely to be successful in coming to a consensus around the types of initiatives that should be pursued, and the resources required to implement them. They also are skilled in resolving competing priorities.
The HFMA/CareCredit survey shows that when leaders are unable to manage the tensions between operational needs and long-term strategy, this internal conflict weakens their ability to put consumer-centric tools and programs in motion. When they do embark on consumerism strategies, they said they typically have poor success.
According to the survey, one lesson learned from organizations that have had good or great success in setting consumerism strategies and resolving internal priorities to put them into action is to keep patients at the center of all they do (see the exhibit below).
Success factors in resolving internal priorities to make way for consumerism
How have you managed to be successful at resolving other higher priorities internally so that you may properly address healthcare consumerism?
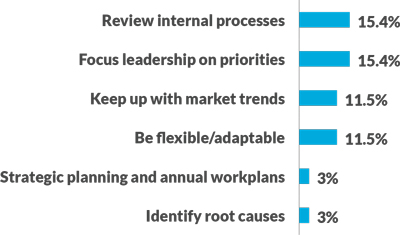
Source: CareCredit Healthcare Consumerism Survey, conducted by HFMA, February 2020
Additionally, organizations that are more proactive in their approach to consumerism rate patient satisfaction as more important than organizations that define their approach as more reactive to patient demands or the market environment.
At Privia Health, a national physician organization with more than 2,500 providers in multiple states, prioritizing patients’ needs keeps consumerism strategy focused on initiatives that matter most. For the past five years, Privia has won the HFMA MAP Award for excellence in revenue cycle performance.
“Our patient engagement road map focuses on several aspects of the patient-provider relationship,” said Jen Porter, vice president, marketing, communications and patient experience for Privia Health. “Patients share feedback through a number of venues, including online reviews and our patient satisfaction survey. We value their feedback, and we leverage this actionable insight to streamline our efforts to meet patients where they are — and where they are is often online and on the go.”
To develop a trusted relationship with patients, Privia Health focuses on eliminating points of potential friction to elevate the patient experience. The organization also seeks opportunities to engage teams and use technology to help patients.
“Privia provides resources to keep patients connected to their healthcare teams,” Porter said. “Our proprietary technology enables patients to message their doctors, schedule appointments, pay bills, see lab results, refill prescriptions and receive reminders about important health screenings.”
Also important during the coronavirus pandemic: addressing consumers’ safety fears, especially at a time when 72% of consumers have changed their use of healthcare services due to the outbreak.c “Consumers want to know, ‘What are you doing to help keep me safe?’” Porter said. “We make sure they understand how many processes are in place to help protect their health.”
3. Patient involvement in setting the organization’s consumerism strategy
The degree to which healthcare organizations understand what patients want and use this insight to inform consumerism strategies is a key contributor to success. So is the extent to which organizations value patient access to information, patient satisfaction and hands-on, personal relationships, the HFMA/CareCredit survey found.
At Ochsner Health, the health system’s Patient & Family Advisory Board shares firsthand input with leaders into ways the organization could better meet the needs of families, such as through new services, support mechanisms, and robust partnerships between families and healthcare professionals. The board also offers suggestions for creative, cost-effective solutions to challenges faced by the health system, as well as ways to promote awareness of Ochsner’s services. Meetings take place at locations throughout the system.
“We’re a big system, so we’re not able to implement new consumerism initiatives as quickly as a smaller system,” Cardwell said. “That’s one reason why we’re very intentional in our approach to developing a consumer-centric experience. We gather feedback from patients as well as core groups throughout the system to improve the patient experience, and we use patient experience coaches to help refine interactions patients have with our system and our staff.
“For example, our region was hit pretty hard by COVID-19, and a lot of our economies — from tourism to the restaurant service industry — were shut down. The first thing we did was to turn off our collection dialers so that patients weren’t receiving calls about outstanding balances at a time when they were facing extreme financial distress,” Cardwell said. “We continued to send statements, so patients would know the amount they owed, but they would also know: ‘We understand the situation you’re facing, and we’re going to give you extra time to pay for your care.’”
Creating a patient advisory council also is a 2020 strategy for Privia Health — and it’s one the organization was able to accomplish in spite of the challenges of the pandemic. “We already have 2,000 patients who have volunteered to be part of this group,” Porter said. “We’re very proud of our ability to keep this going, even during the pandemic.
“When you think about healthcare consumerism, it is critical that healthcare continue embracing opportunities to create a seamless experience for patients and their families,” Porter said. “Patient input is vital to designing a patient-centric consumerism model.”
Consumerism in the age of coronavirus (COVID-19)
The coronavirus pandemic made a deep impact on consumer finances, with 5.4 million Americans losing their health insurance due to job losses during the pandemic — more than have ever lost insurance in a single year.d Here are three ways healthcare organizations can help strengthen their relationships with patients during the pandemic.
Take a more proactive approach to financial engagement. With cost concerns prompting many consumers to avoid seeking care, hospitals should consider proactively helping consumers understand not only their out-of-pocket costs of care, but also their options for payment. Offering payment options that allow patients to pay over time could be key to helping them move forward with the care they want and need.
Make sure payment policies reflect empathy for your patients. Consider delaying collection calls during the height of a coronavirus surge in your market, and provide the tools and training staff need to offer the right support for patients at the right time. Double down on efforts to contact patients through their preferred communication channels, stressing the desire to work with them in establishing financial arrangements that meet their needs, such as financing or payment options.
Strengthen remote workforce efficiency. As more revenue cycle work shifts to a remote work environment, assess where opportunities exist to improve efficiency, such as by automating specific tasks, like eligibility checks, and hiring a vendor to handle paper-heavy processes, such as payment processing.
Footnotes
a HFMA, “Understanding the approach to successful healthcare consumerism initiatives,” November 2020.
b Milani, R.V., MD, et al., “Reducing Hospital Toxicity: Impact on Patient Outcomes,” The American Journal of Medicine, May 2, 2018.
c “COVID-19 Shifts Consumer Behavior, Attitudes Toward Health Care Services,” Alliance of Community Health Plans, press release, May 21, 2020.
d Stolberg, S.G., “Millions Have Lost Health Insurance in Pandemic-Driven Recession,” The New York Times, July 13, 2020.
Common impediments to developing a consumer-centric model of care
- A survey of healthcare finance leaders, conducted jointly by HFMA and CareCredit, identified numerous impediments to achieving consumer-centric care and services.a Those impediments include:
- Lack of appropriate staff resources to lead initiatives
- Budgetary disputes
- Limited resources — and multiple priorities
- Too many priorities, and not enough time to thoughtfully address requirements
- Inability to come to a consensus around the types of initiatives that are needed
Footnote
a. HFMA, “Understanding the approach to successful healthcare consumerism initiatives,” November 2020.
This content is subject to change without notice and offered for informational use only. You are urged to consult with your individual business, financial, legal, tax and/or other advisors with respect to any information presented. Synchrony and any of its affiliates, including CareCredit, (collectively, “Synchrony”) makes no representations or warranties regarding this content and accepts no liability for any loss or harm arising from the use of the information provided. Your receipt of this material constitutes your acceptance of these terms and conditions.






