Analysis: Implications for providers as Amazon offers its employees access to a virtual clinic
- Amazon has launched a virtual health clinic for employees and their families living in Seattle, Modern Healthcare reported.
- There are more than 53,500 Amazon employees living in the Seattle region, according to Modern Healthcare.
- HFMA’s Chad Mulvany says this effort by Amazon will not only improve the convenience of its healthcare offering for its employees and reduce costs, but also could give it experience in managing population health.
Modern Healthcare is reporting, “Amazon has launched a virtual health clinic, dubbed Amazon Care, for employees and their families living in Seattle.”
“The pilot program, which offers a combination of telemedicine and home visits, marks the most recent step the Seattle-based tech giant has taken into the healthcare sector,” the article continued.
“Amazon Care is marketed as a benefit being piloted for company employees enrolled in an Amazon health insurance plan, according to a company website,” Modern Healthcare said. “Employees will be able to reach physicians or nurses for urgent care, preventive health consults and sexual health services, such as testing for sexually transmitted infections. Employees will be able to chat with clinicians via a messaging app, video consultations and home visits. Employees can also request for a courier to deliver their prescriptions to their home or office. The pilot is only available to employees and their families in the Seattle area. However, there are more than 53,500 Amazon employees living in the Seattle region, according to the Seattle Times.”
Takeaway
Specific to Amazon, it’s not surprising they have launched a virtual option for their employees. Viewed narrowly, it’s a play to improve the convenience of their healthcare offering for employees, maximizing employee productive time, especially given that the average clinic visit requires two hours. This virtual option will likely also reduce cost.
Viewed through a broader lens, this is Amazon experimenting with their captive employee population, which is like how many health systems have used their own employee health plans to gain experience “managing population health.”
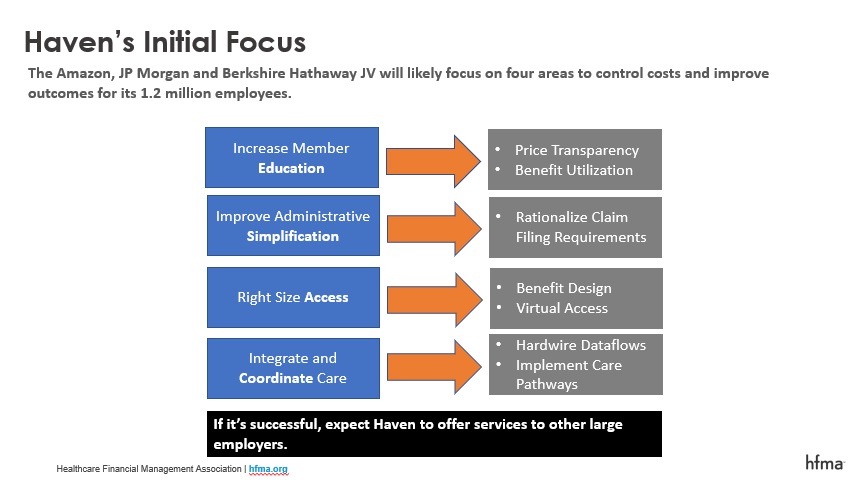
This also is very much aligned with two of the strategic goals of Haven — the Amazon, JP Morgan, Berkshire Hathaway joint venture aimed at helping reduce the participating companies’ employees’ healthcare cost. As illustrated in the chart below, it squarely checks the “right-size access box” and creates an opportunity to “integrate and coordinate care” by helping control referrals. Not only could this become part of the Haven solution, but I would imagine that Amazon will also apply lessons learned from this exercise to its efforts to create a healthcare platform. This is an option many employers are already providing, and I would anticipate we’ll see more in the future.
Similar to my comments on Humana’s pilot of a virtual-primary care-only plan for small employers, my assumption is when Amazon employees or Amazon employees’ covered family members using virtual care needs a referral to a specialist, an AI algorithm in the background will likely recommend physicians in the network. The recommended network physicians will be those who based on claims experience and clinical data are more cost efficient and achieve better outcomes.
For health systems whose employed/aligned physicians achieve high-quality outcomes in a cost-efficient manner, this presents an opportunity to grow market share for services. For everyone else, this strategy basically negates investments in primary care and outpatient clinics.





