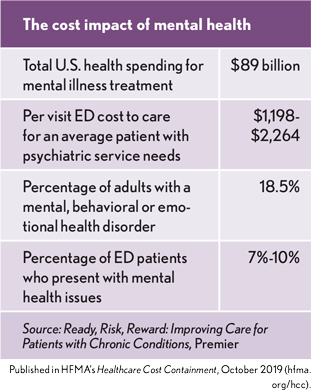
Care coordination can reduce $89 billion behavioral health cost impact
Behavioral health issues account for about one quarter of all emergency department (ED) visits, according to a Premier analysis. One of the primary reasons for ED visits associated with mental health conditions is lack of access. Nearly 40 percent of adults with severe mental illness — such as schizophrenia or bipolar disorder — received no psychiatric treatment in the previous year, according to the 2012 National Survey on Drug Use and Health. Among adults with any mental illness, 60 percent were untreated. National shortages of mental health professionals and affordable psychiatric care means that in many communities the ED is where patients seek care.
A continuum of care program is one way hospitals and health systems can address this challenge. For example, Henry Ford Allegiance Health, a 475-bed health system in Jackson, Michigan, used a cross-continuum of care management program that streamlined access to behavioral health and community services and decreased wait times in the ED, according to a Premier report. Other results include reduced opioid overdoses and readmissions and $430,000 in consolidated savings.