A focus on reducing PAC spending has been shown to yield a number of benefits.
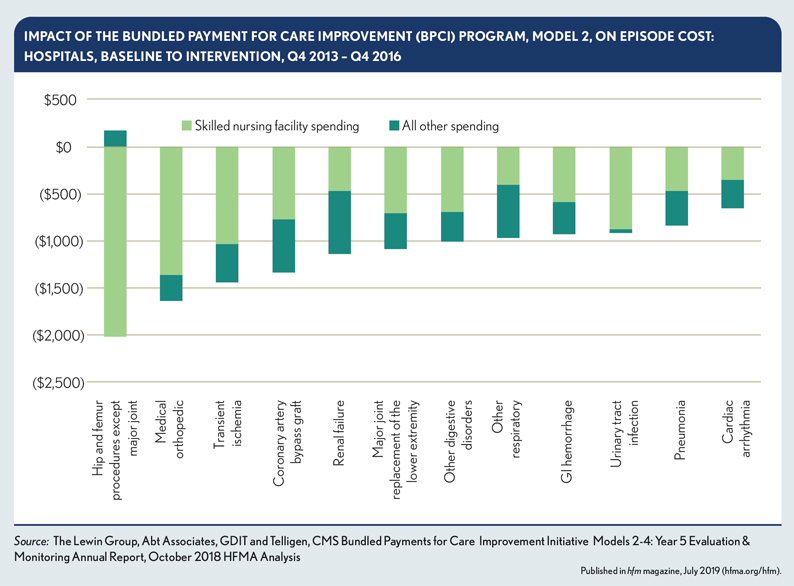
The Institute of Medicine estimates that eliminating variation in PAC spending would reduce variation in Medicare spending overall by 73%.a That assertion is corroborated by recently reported results of Medicare’s Bundled Payment for Care Improvement (BPCI) program regarding hospital-initiated episodes, where reduced skilled nursing facility (SNF) spending accounted for 70% of episode savings among episodes that experienced statistically signifi cant savings (see the exhibit below).b The reduced SNF spending resulted from making
The use of high-value PAC providers also been shown to have the spillover effect of reducing readmissions. In Medicare alternative payment models, provider participants often see this improvement opportunity associated with PAC spending as “low-hanging fruit” relative to other opportunities, such as:
- Reducing ambulatory-care-sensitive admissions, which are multi-factorial and heavily influenced by SDOH.
- Implementing palliative-care programs, which may require a cultural shift.
- Redirecting referrals to freestanding sites of service, which may not offer significant savings relative to other opportunities.
Footnotes
a. Institute of Medicine, Variation in health care spending: target decision making, not geography, July 2013.
b. HFMA analysis of BPCI year 5 Evaluation report. patients’ homes, with home-health support, the discharge setting of choice wherever appropriate, rather than SNFs.