Creative solutions to tackling top challenges in healthcare: 3 key insights
The pandemic forced healthcare leaders to hit “reset” on organizational priorities as workforce shortages, high rates of burnout, technology infrastructure limitations and data security concerns challenged their ability to meet the healthcare needs of their communities.
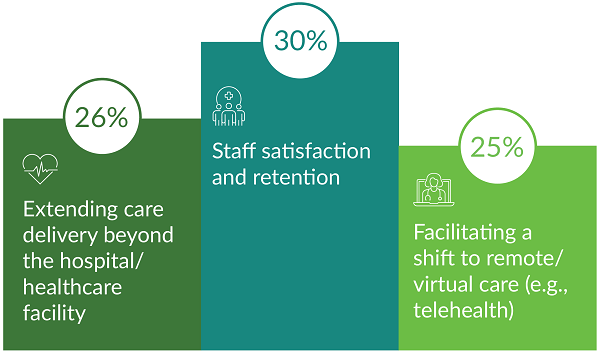
A global survey of 3,000 healthcare leaders conducted by Philips indicates leaders are intensely focused on staff satisfaction and retention, the drive to extend care delivery beyond hospital walls — including through digital investments — and unlocking the power of big data and analytics. But the pace of development has been slow, survey results indicate. For example, many leaders are frustrated about the lack of progress in embedding data throughout care pathways, with 51% saying data silos hinder their ability to use data effectively. Nearly one out of four say technology infrastructure limitations impede their ability to successfully leverage data (For more information, see the exhibit on the third page of this article). Meanwhile, among late technology adopters, 32% say they face challenges gaining staff buy-in for technology investments.
In this HFMA roundtable sponsored by Philips and moderated by HFMA in Summer 2022, healthcare finance leaders throughout the United States shared ways their organizations navigated three of the biggest challenges in an environment shaped by COVID-19 and the lessons they learned along the way.
Tackling the human capital crisis is top of the agenda for healthcare leaders
1. Ensuring staff are adequately supported; decreasing the risk of burnout.
Have there been any efforts to innovate your care delivery model to ensure clinical staff are used more efficiently and effectively? How can new models help?
Brian Sims: One of the major conversations we’re hearing around new care models and new staffing models is around the use of technology and care extenders so that lower-level staff can support nurses. For instance, certain types of technologies can help medical assistants triage patients appropriately to ensure patients are treated in the appropriate setting. This helps avoid instances where patients end up seeking care in the emergency department because they didn’t receive the right care in the right place at the right time for their condition. We’re also seeing increased use of monitoring technology to ensure quality of care is not disrupted and, in fact, can actually be improved, despite the human capital issues we have in healthcare.
The impact of organizational gratitude in addressing burnout also cannot be overstated. Burnout issues stem not just from high clinician-to-patient ratios, but also the working environment — especially during a pandemic. It’s about finding ways to enhance the environment of care and make the administrative duties of care easier.
Karie Ryan: What we’re seeing is that leading organizations are empowering a “system of action.” They’re using data to keep the entire care team informed, making sure that data from monitoring devices, telehealth and more are available anywhere, anytime. We’re also seeing solutions emerge that help clinicians close critical gaps in patient data while supporting continuity of care. The best solutions prompt clinicians to alert a physician when intervention is needed, ensuring patients are triaged appropriately and that they get the care they need quickly.
George Farhat: Our anesthesia practice has grown through acquisitions, and each practice has analyzed its local staffing. We look at clinical opportunities on a consolidated basis, learning from best of breed. We talk about clinical staffing and ways to expand nursing coverage with our care team. When an acute care partner like our practice is integrated with the hospital network, if we are engaged exclusively, this gives us more range to consider, ”How can we optimize this facility to the best of our ability?” versus following a surgeon model and providing support as the surgeons request it, which is not as efficient. There are some constraints on how we can partner with hospitals based on the level of engagement, but it’s a huge opportunity for us to expand the level of care and access while leveraging our care teams to provide more support.
Amy Pyke: Real-time decision support for clinicians is a game changer for reducing administrative burden and the risk of burnout. A recent survey shows one of the top threats to patient safety is incomplete patient data. Yet lack of interoperability limits clinicians’ access to data in critical moments. By investing in tools that speed access to data and help clinicians decipher which information is important for making care decisions, hospitals can help improve quality of care while reducing the risk of burnout.
2. Navigating the challenges — financially and operationally — of providing care in a pandemic environment.
The financial challenges of healthcare reform implementation are in the minds of hospital executives. What are some of the obstacles you’re facing, and how is your organization handling these financial challenges?
Donna Kelly Ramicone: Labor shortages are killing us right now. And you know, we’ve tried all different kinds of things, such as labor pools that travel to our hospitals, but we’re ready for new and creative ideas because what we’re doing isn’t working anymore. We’re trying to figure out who has some new innovative ideas that we can use.
Nasha Bunch: One of the things our organization has been doing to try to cut costs is to create a labor pool. There is a critical shortage of talent across the board. We’re competing with other health systems in our area by offering not only bonuses to come to our organization, but also retention bonuses for key areas. We’re also exploring multitasking opportunities for some employees. For example, we’re training our registrars to do insurance verification so that if an employee leaves the organization or needs to take time off, the work doesn’t stop.
Ryan: We’re seeing this everywhere, and it’s a huge burden. One of the most pressing challenges for caregivers in ICUs is the volume of data they collect. Each patient in the ICU generates thousands of data points per day, leaving physicians and nurses feeling overwhelmed as they struggle to decipher which data points are useful and increasing the mental burden imposed on the team. If a hospital has a shortage of nursing and other clinical staff, it makes the situation much more difficult.
Craig Gilliland: We’ve had a little bit of luck by increasing referral bonuses. We have sign-on bonuses, of course, and like all hospitals, we were throwing money at [recruitment and retention] that we really don’t have. We brought in a new HR director, and he really pushed to increase the referral bonus, because if you’re a nurse and you know a nurse, you will probably have greater luck in recruiting that person than the hospital as an organization will. We’ve gained at least some traction in recruiting new talent to our hospital since increasing our referral bonuses.
Elaine Matzenbacher: We’ve increased our referral bonuses, but the difference for an organization like ours is that we can’t use agency workers. There really aren’t agency nurses who are specialized in our side of healthcare. Instead, we’re incentivizing our current staff with longevity increases. With staff who have been here for five years, 10 years, 15 years or longer, we’ve given them $1 to $2 an hour more than the base rate to make sure we’re keeping our staff. We’ve also incorporated staff-wide bonuses the past couple of years. Again, you’re throwing money at your staff, and it’s money that you may or may not have, but it’s the only way.
Ryan: As ICUs and general wards typically have technology from a variety of manufacturers, vendor neutrality becomes critical in closing data gaps between care settings that could interrupt the pace of patient care. Standardizing the monitors and tools they use across floors, towers and sites and then allowing the data to flow uninterrupted are two approaches.”
Healthcare leaders identify barriers to effective data use

3. Making decisions around technology when labor and financial resources are constrained.
How do you prioritize the use of new technology and decide which technology is going to be implemented, and when, and how it will be funded?
Paresh “Perry” Patel: Technology is like a bug that you have to be one step ahead of because it changes. Even the technology we put in place two years ago, at the start of the pandemic, is sort of obsolete and/or doesn’t have all the functionality that clinicians need. With new technology requirements being adopted, healthcare organizations are always going to be somewhat behind. The key is to find a technology partner that can grow with you without killing you with fees, because spending on technology fees is out the window at this point.
Sims: We sometimes conflate technology with innovation. Innovation doesn’t require technology. To be on the forefront of change, organizations must be thoughtful and mindful about how to do something they’ve always done in a new way. Maybe that requires technology, maybe it doesn’t, but when you present a technology solution or tool for a problem that has already been identified by clinicians as having the potential to make a task easier, that’s when it gets prioritized. People are getting a little weary of being told what something can do for them without considering whether that’s something they want technology to do or whether it’s something they are already doing well without the help of technology. You can innovate without spending money.
Bunch: Our IT department vets ideas for new technology first to make sure it works with our current systems and that it’s unlike anything we already have. From there, they go to administrators to determine whether a new solution or upgrade will be approved and, if so, how to roll it out, and the type of training that should be conducted. There’s a whole process of evaluating a tool or upgrade before a decision is made.
Gilliland: It’s also important to consider the type of support you can expect from the vendor. One data challenge that kind of goes unseen is the turnover within all these data analytics companies. I can’t ever get the data that I’m requesting for this or that because of COVID. More people are working from home, so they don’t come on site. They used to roll up their sleeves with me and work side by side. Now, they try to assist me remotely. That doesn’t always work out like we’ve hoped it would. We talk about nurses bouncing around for the dollar. Well, developers do, too. So do salespeople. I’d be willing to pay a little more if I thought I could talk to the same person to get my questions answered quickly; get my data.
Farhat: You also have to understand your total cost-of-care model because everything flows from that. And as it relates to financial targets, population health targets and quality targets: Those are the types of things where our hospital leaders are looking for solutions to anticipate what’s coming and stay ahead of the curve.
Ryan: Considerations around new technologies should always start from the viewpoint of, “What is the problem we’re trying to solve?” Once you’ve determined what problem you’re trying to solve, think about the KPIs and ways to gain ROI from an operational perspective, financial and quality perspective. When you make technology decisions with these perspectives in mind, the decisions you make will have greater value for your team, your patients and your organization.
Panelists

CRAIG GILLILAND, MBA
CFO and corporate compliance officer for Pleasant Valley Hospital in Point Pleasant, West Virginia

PARESH “PERRY” PATEL, CHFP, MBA, CHA
CFO of the Community Service Board for Fairfax County Government in Fairfax County, Virginia

AMY PYKE
Head of global market access, reimbursement and health policy for Philips in Cleveland, Ohio

DONNA KELLY RAMICONE
Director of finance/controller for Tenet Healthcare in Charleston, South Carolina

KARIE RYAN, RN
Clinical transformation lead for Philips in Cambridge, Massachusetts

BRIAN SIMS
Vice president, quality and equity for Maryland Hospital Association in Elkridge, Maryland

ELAINE MATZENBACHER
CFO for Hospice of Southern Illinois in Belleville, Illinois
NASHA BUNCH, MBA
Director of patient access for St. Christopher’s Hospital for Children in Philadelphia, Pennsylvania
GEORGE FARHAT
Director of revenue, financial services for U.S. Anesthesia Partners in Dallas, Texas
About Philips
Philips is a leading health technology company focused on improving people’s lives across the health continuum – from healthy living and prevention, to diagnosis, treatment, and home care. Applying advanced technologies and deep clinical and consumer insights, Philips delivers integrated solutions that address the Quadruple Aim: improved patient experience, better health outcomes, improved staff experience, and lower cost of care. Partnering with its customers, Philips seeks to transform how healthcare is delivered and experienced. The company is a leader in diagnostic imaging, image-guided therapy, patient monitoring and health informatics, as well as in consumer health and home care.
This published piece is provided solely for informational purposes. HFMA does not endorse the published material or warrant or guarantee its accuracy. The statements and opinions by participants are those of the participants and not those of HFMA. References to commercial manufacturers, vendors, products, or services that may appear do not constitute endorsements by HFMA.






