An HFMA-CereCore survey found that nearly a quarter of CFOs say they need better collaboration with CIOs when making technology decisions. This includes additional information about the risk assessment of IT spend, prioritization of major initiatives and alignment to corporate goals, expected ROI and more.
Half of healthcare organizations are pursuing some type of digital health strategy; however, nearly a quarter of CFOs (23%) say they are somewhat or very dissatisfied with the collaboration between finance and IT, or that there is no collaboration at all.
This trend was identified in a 2022 survey of 238 healthcare finance, accounting and revenue cycle executives, sponsored by CereCore. Other findings included:
- 29% of CFOs need CIOs to provide more information about the expected ROI of IT initiatives.
- 42% of CFOs say they need CIOs to provide more information about how to prioritize major initiatives, align those initiatives to corporate goals and assess the risk of IT spend.
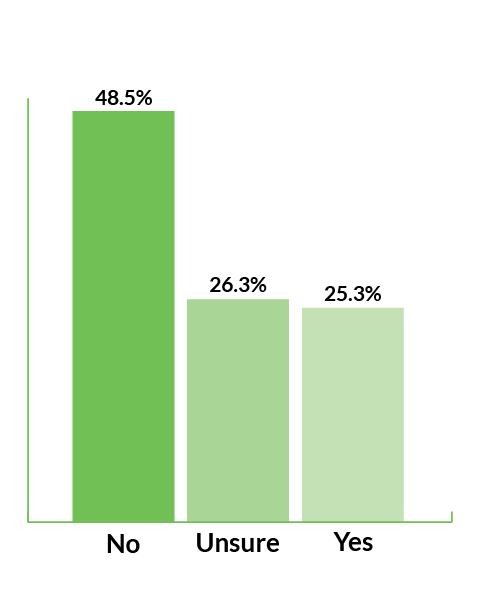
- Only a quarter of healthcare organizations track results and measure ROI for technology investments.
- When investing in technology, 41% of CFOs need CIOs to provide more information about a long-term strategy and how the IT investment will improve a function, service or product.
The survey results clearly demonstrate the need for greater collaboration between finance and IT, said Peyman Zand, vice president of advisory services at CereCore.
“IT has become more complex and integrated with every facet of the business,” he said. “It shouldn’t exist on its own. If CFOs and CIOs communicate more effectively and find common ground to understand each other’s perspectives, they could really move the needle on strategic initiatives.”
Improving collaboration between finance and IT
What does greater collaboration entail? “I’ve consulted with successful healthcare organizations and what sets them apart has been complete alignment between CFOs, CIOs, key business unit leaders and the enterprise as a whole,” said Zand.
“The CEO sets the tone, but once the players are aligned, collaboration will happen naturally. CFOs and CIOs begin talking the same language on the cost of IT operations. For example, CIOs help CFOs understand this question: ‘What is the risk for delayed spending?’”
The benefits of this collaboration are substantial, said Zand. “The more collaborative the relationships, the better prepared organizations are to stay ahead of competitors and disruptors. When the CFO and CIO have an ongoing dialogue about technology investments for the future, they pave the way for technology to bring innovation to clinical and business units.”
For example, presenting a business case on healthcare technology is a perfect opportunity for an organization’s leaders to discuss strategy and goals, risks, value, ROI and success metrics. When CIOs understand clinical and business unit challenges, they can suggest technologies that solve real-world problems. Vice versa, CFOs get a better understanding of the risks associated with delaying an IT investment and the value of moving forward with the IT investment.
“Another example is when CIOs go to the Chief Medical Offer (CMO) and say, ‘I know this product will bring advantages to your work area. Are you interested in looking at it with me?’ This changes the whole template of how CIOs are perceived,” said Zand.
Assessing impact on clinical, business units
In contrast, healthcare organizations without ongoing synergy between finance and IT may prioritize initiatives based on subjective evidence (e.g., what a high-value physician wants), said Zand.
“It’s about process first, people second and technology third,” he added. For example, before investing in a new cardiac system, he said CFOs need to ask these questions: Why are we doing this? Are there not enough cardiac surgery centers in our geographic region? If so, how many cardiac surgeons and other resources would we need? Do we need to open 10 centers, or do we really only need five? Where is the greatest demand?
“The final step is the system,” said Zand. “CFOs need to follow this process before listening to a surgeon who says, ‘I went to this conference and saw a cool cardiac surgery system that I want.’ That technology might not be well suited for your organization. For example, it might be designed for a health system with 100 surgeons rather than 10.”
Sharing data for strategic decisions
Data sharing is an important element of this collaboration. When IT is tightly aligned with the strategic road map and business unit goals, CIOs know what data CFOs need and when, said Zand. For example, IT can develop emergency department (ED) analytics to help CMOs prepare for seasonal increases and staff the ED more effectively.
Likewise, as organizations consider joining an Accountable Care Organization (ACO), IT can provide the right historical data and analytics to promote success, said Zand. “When I look at the ACOs that are successful, it’s because those ACOs have been able to use and analyze data in a way that actually helps the populations they serve. IT is one of the keys to their success and so is the ongoing dialogue between the CIO and CFO.”
Tracking ROI over time
Despite an emphasis on ROI, the majority of CFOs tend not to track it over time, the HFMA survey found. This is an area ripe for collaboration, said Zand. Talking about ROI and the value of technology investment begins with presenting a solid business case.
More specifically, IT can help develop and track the key performance indicators necessary to understand impact, such as revenue, quality of care improvement, physician satisfaction, patient attraction, retention and more. Having a systematic approach for prioritization and tracking ROI will help reduce personal biases from decision-making.
Do you track results and measure ROI for technology investments?
Exploring zero-based IT budgets
A zero-based budget is one way to better integrate IT into the enterprise as a whole, said Zand. “All of the IT budget exists within the business units,” he added. “IT gets paid by the business unit for the work it does. This can be a very effective strategy to encourage alignment between business unit and IT leaders. It also reduces waste as business units will only request what is needed to improve their business and bring a return on investment.”
Leveraging health IT outsourcing
Another strategy is to outsource a portion of IT services, said Zand. “Outsourced services can help organizations get out of the mundane, utility part of IT management,” he said, adding that many external firms manage IT more efficiently and at a lower cost. “These external firms also tend to have better compensation packages and career paths for IT resources.”
However, the goal isn’t necessarily to outsource everything. “It’s about being selective. Organizations need to retain certain functions and outsource the utility part of it,” he added.
The biggest benefit of IT outsourcing? “It allows the CIO to then concentrate on more innovation, especially when they’re tightly aligned to strategic goals,” said Zand. “This is the kind of innovation healthcare organizations can achieve, but only when they’re not primarily focused on daily operations.”
Conclusion
Greater collaboration between finance and IT is a necessary step toward ensuring sound IT investments. At the heart of this collaboration? Collaborative business case development, data sharing, clinical and business unit integration and partnership with an outsourced IT vendor. The more process-oriented an organization becomes, the more efficient and innovative it becomes.
Download the Finance and IT Collaboration Survey Report
About CereCore
CereCore® provides IT services that make it easier for you to focus on supporting hospital operations and transforming healthcare through technology. With a heritage rooted in our nation’s top-performing hospitals, we serve as leaders and experts in technology, operations, data security, and clinical applications. We partner with clients to become an extension of the team through comprehensive IT and application support, technical professional and managed services, IT advisory services, and EHR consulting, because we know firsthand the power that integrated technology has on patient care and communities.
This published piece is provided solely for informational purposes. HFMA does not endorse the published material or warrant or guarantee its accuracy. The statements and opinions by participants are those of the participants and not those of HFMA. References to commercial manufacturers, vendors, products, or services that may appear do not constitute endorsements by HFMA.






