Findings of a three-year study that involved 7,000 patients in long-term care facilities show telebehavioral health can produce a meaningful ROI.
Telebehavioral health is an innovation with the potential to lower overall costs of care by keeping residents of long-term care facilities out of the hospital and the emergency department (ED).
The impact of behavioral health diagnoses and services on residents of long-term care facilities should not be downplayed. About 50 percent of people living in long-term care facilities have a behavioral health diagnosis, according to the U.S. National Center for Health Statistics. Diagnoses include dementia, depression, anxiety, delirium, and other cognitive and neurological disorders.
Moreover, long-term care is only becoming more pressing as an area of concern within the nation’s healthcare system. About 1.4 million people reside in long-term care facilities in the United States, and that number is expected to increase 80 percent by 2050. a Further, nearly 30 percent of long-term care facilities are outside major metropolitan areas, in locations where behavioral health services are scarce or nonexistent.
Deploying telebehavioral health services means purchasing and installing sophisticated equipment that meets all privacy and security requirements and is acceptable to providers, residents, and caregivers. It thus involves a substantial capital outlay that can amount to hundreds of thousands of dollars. The cost can be depreciated, and there might even be salvage offsets when the equipment is refreshed, but for finance executives, the fundamental question is, “What is the return on such an investment?”
One benefit that telebehavioral health can be expected to deliver is improved access to care. But finance leaders also must determine the ROI from increased revenue billing to Medicare for telemedicine procedure codes, and savings through indirect effects such as lower use of hospital services and ED visits. The key question is: “Does telebehavioral health actually produce such savings?” The ability to achieve meaningful savings would be important under risk-based contracts in which reductions in hospital services and ED visits are rewarded and care for patients is improved.
Telehealth programs for primary and specialty medical care have been studied for many years. A review of the literature shows 1,494 citations about telehealth. b By contrast, telehealth for residents with behavioral diagnoses has been studied with only small samples, and there has been little primary research into integration of behavioral and physical health with telehealth. This report may be one of the first to look at the financial implications of telehealth for such patients.
The Bridges to Behavioral Health Project
To assess the potential revenue impact from telebehavioral health services, we reviewed results of the Bridges to Behavioral Health Project, an initiative involving the deployment of such services in facilities operated by the Newport News, Va.-based Riverside Health System, which serves the tidewater region of eastern Virginia. The project was a collaboration between Bay Rivers Telehealth Alliance in Tappahannock, Va., and Riverside Health System’s Center for Excellence in Aging and Lifelong Health, and it was supported by a grant from the Health Resources and Services Administration of the U.S. Department of Health & Human Services.
The aim of the project was to deploy new tele-behavioral health services in long-term care facilities, behavioral health clinics, and hospitals at existing rural sites. This deployment provided the conditions for a natural experiment to examine the financial effect of adding telebehavioral health services to the long-term care facilities. In the period of Jan. 1, 2013, through Dec. 31, 2015, five facilities received the intervention and five did not, allowing the financial performance of facilities with telehealth services to be compared with that of other facilities. The differences noted provide the basis for the analysis that follows.
The framework for thinking about the impact of telebehavioral health is a straightforward consideration of the new set of interventions made possible through telehealth and their effect on the process efficiency of delivering care. In general, these interventions include the following:
- Diagnostic interview examinations performed by psychiatrists
- Individual psychotherapy sessions
- Pharmacologic management neurobehavioral status examinations
- Follow-up in-resident telehealth consultations
- Health behavioral assessments
Telehealth interventions were followed by appropriate clinical services.
The telebehavioral health initiative also provided for professional development and continuing medical education to facility staff and community providers.
Notably from a financial standpoint, our analysis disclosed that the patients in the intervention group (i.e., the five facilities deploying telehealth services) experienced a decrease in the likelihood of ED visits, no change in the likelihood of an inpatient hospital visit, a decline in outpatient hospital visits (by more than 11 percentage points), and an increase in reporting of cognitive impairment. Quality of care improved because the new telehealth services discovered previously undiagnosed cognitive impairment, which could then be treated. The absolute number of residents in the intervention group with moderate or severe pain fell by roughly half.
Statistical tests for differences revealed the intervention and comparison group were the same in terms of demographic characteristics (gender, race, age, age group), with no statistical differences among key segments, including the roughly two-thirds of the two groups who were female, the one-fourth who were African American, and the mean age of 78 years. Moreover, there were no statistical differences prior to the initiative between the intervention and comparison groups for number of physician office visits, resource utilization groups (2012 version), length of stay for those with a hospital stay, falls, or 30-day hospital readmissions.
ROI Factors
Results of these analyses of effects of the use of telebehavioral health over the three-year period were used to model the financial impact. ROI analysis factors included following:
- The numbers of telebehavioral health visits and the increased Medicare revenue derived from them
- Indirect revenues from avoided hospital services and avoided ED visits, taken from the analysis of the intervention and comparison groups described above
- The original capital outlays for secure telebehavioral health equipment that is compliant with the Health Insurance Portability and Accountability Act (HIPAA)
Intervention Components
A telebehavioral health intervention involves two basic components: the deployment of the telemedicine equipment and the commitment of the clinical staff engaged to perform the intervention.
The telehealth equipment deployed in the intervention sites was a CISCO CA300 telemedicine cart system supported by secure and private T-1 business internet lines. The equipment was installed in 2013. None of the facilities had the equipment or the capability to deliver telebehavioral health services in 2012.
Services in each facility in the intervention group were delivered by a board-certified geropsychiatry physician and a collaborating geropsychiatry nurse practitioner. The services performed and their CPT codes were as follows:
- Individual health behavior assessment (CPT codes 96150-96154)
- Individual psychotherapy (CPT codes 90804-90809)
- Pharmacologic management (CPT code 90862)
- Psychiatric diagnostic interview examination (CPT code 90801)
- Neurobehavioral status examination (CPT code 96116)
Study Assumptions
The assumptions on which the pro forma analysis is based involved four key considerations: volume of visits, telehealth originating-site fee, indirect revenues, and the original capital outlay. Because data for the three-year study period (2013-15) were incomplete, certain assumptions were extrapolated from the data.
Behavioral telemedicine services. The procedure code, amounts paid by source, and date of services for telebehavioral health patient visits for 2014 and 2015 were known; however, there were no similar data for 2013. We assumed a straight-line trajectory of visit volume and assigned the percentage increase from 2014 to 2015 (which was 33.5 percent) to deflate the 2014 visits for an assumed number of 2013 visits.
Telehealth originating-site fee. Medicare allows billing when the distant site provider certifies that the beneficiary was present at an eligible originating site when the telehealth service was provided. The Medicare telehealth originating site fee is $25 and is shown in the exhibit below as added revenue for each visit.
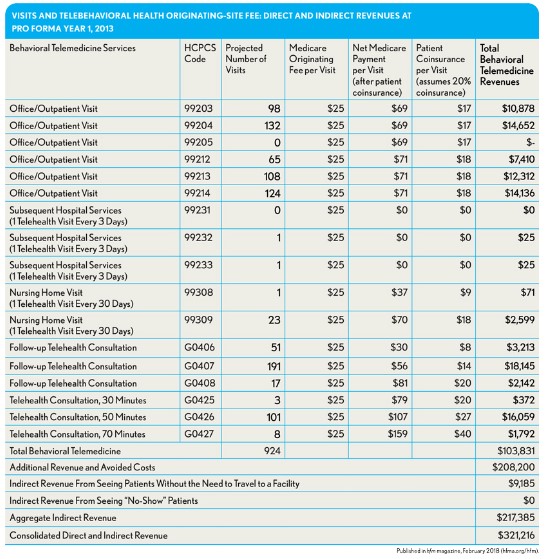
Indirect revenues. We assumed, as do other similar studies of telehealth, that there is an indirect revenue effect. c We used the results of the analysis of the early effects from the baseline year of 2013 to the final intervention year of 2015 to make ROI assumptions about indirect revenues. We assumed that there were avoided hospital outpatient department visits that would free appointments for other patients, and we assumed a reduction in ED visits that would free space for net revenues from other patients. The assumptions were that there would be 198 fewer hospital outpatient department visits and 78 fewer ED visits per year, based on our analysis of the actual experience discussed above. A reduction in hospital admissions and length of stay that would reduce hospital costs was not observed from 2013 to 2015.
It was assumed that these indirect costs were constant in each pro forma year. Finally, the indirect revenues account for savings from the providers not traveling to see the patients for traditional face-to-face visits.
Original capital outlay. The original capital outlay was $470,638 for long-term care facility equipment, $15,000 for software licenses, and $120,732 for servers and infrastructure changes. With a depreciation life of six years, the annual straight-line depreciation was $31,789.
ROI Findings
In the pro forma Year 1, the Bridges to Behavioral Health Project received from all insurers, almost exclusively Medicare, a weighted average of $112 per visit ($103,831/924). The physician and office management expenses were $79 per visit ($72,640/924) yielding an operating contribution margin of $34 per visit (excluding the initial capital outlay). If fixed expenses were to include depreciation for the original capital outlay, annual total fixed expenses would increase to $85,775. However, factoring in fixed expenses (assumed to be 5 percent of the initial capital outlay and ignoring transmission expenses, which were not available) of $45 per visit ($41,062/924), the contribution margin is $-11. When indirect revenues are added, which are $217,385 in aggregate per year, or $235 per visit ($217,385/924), the contribution margin rises to about $224 per visit.
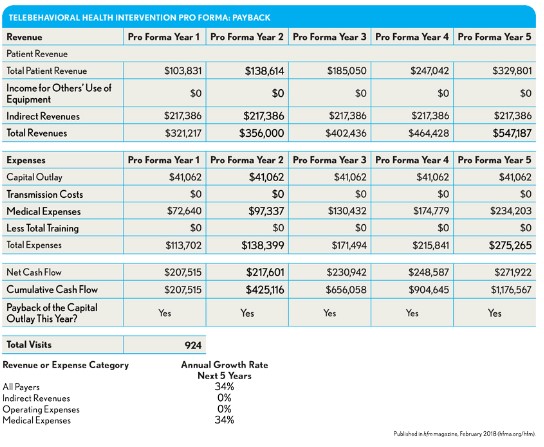
The five-year pro forma in the exhibit above shows the payback, including the initial capital outlay. This telebehavioral health intervention virtually broke even the first year, with a significant payback beginning the second year and increasing each year thereafter. Year 2 and Year 3 reflect the actual experience, in which total patient revenues grew 34 percent. The pro forma assumes the same growth rate in each year. Telebehavioral health has a large ROI largely because of the favorable effects on indirect revenue.
Practical Considerations for Finance Executives
Telehealth is quickly becoming the preferred option for many health systems challenged with provider shortages. Implementing a hub-and-spoke model that allows a provider to reside in one location and provide advice and care to remote areas is becoming increasingly prevalent. Telehealth within long-term care settings is a relatively new area of opportunity that many health systems—particularly those that deliver the full continuum of care—are pursuing.
Elderly patients often require more time and resources than do younger patients, and the care requirements for the elderly become even more complicated when these patients have behavioral health needs. Geriatric and palliative care providers are trained to treat these patients but are in limited supply nationwide. As the population ages, the need for these specialists will only grow in the coming years.
Telehealth affords an avenue for long-term care facilities—particularly those located in rural areas—to deliver the behavioral health care their residents need. The technology not only allows for better care of residents but also helps the residents avoid unnecessary visits to physician offices and EDs. By proactively engaging and treating these patients, facility resources can be used as intended.
Most long-term care facilities operate with thin operating margins due to a heavy Medicaid payer mix. It therefore is vital for them to avoid the disruption of routine processes that can all too often occur with individuals who have behavioral health needs. Under an attribution/risk-sharing type of model, properly managing the behavioral health needs of attributed lives can help ensure that a health system lands on the upside of any risk-sharing pool.
The provision and billing of Medicare for telehealth services are subject to Centers for Medicare & Medicaid Services (CMS) rules and applicable state laws, including scope-of-practice laws especially for physician assistants and nurse practitioners. The technology used must be HIPAA-compliant. For more information, visit the CMS Medicare Learning Network. d
The value proposition of telebehavioral health is not simply a reflection of revenues compared with expenses and capital outlays. Real value also comes from the ability to keep each patient in the proper care setting without disrupting either normal workflows or, more important, the patient’s life. With such an environment, family members are likely to be well-satisfied with the care their loved ones are receiving. Satisfied patients and families are qualitative benefits that offer financial rewards to facilities and health systems.
Footnotes
a. Harris-Kojetin, L., Sengupta, M., Park-Lee, E., Valverde, R., “Long-Term Care Services in the United States: 2013 Overview,” National Center for Health Statistics, Vital and Health Statistics, December, 2013.
b. Totten, A.M., Womack, D.M., Eden, K.B., McDonagh, M.S., Griffin, J.C., Grusing, S., Hersh, W.R., “Telehealth: Mapping the Evidence for Patient Outcomes from Systematic Reviews.” Technical Brief No. 26. (Prepared by the Pacific Northwest Evidence-based Practice Center under Contract No. 290-2015-00009-I.) AHRQ Publication No.16-EHC034-EF, Rockville, MD: Agency for Healthcare Research and Quality, June 2016.
c. McCue, M.J., and Palsbo, S,E., “Making the Business Case for Telemedicine: An Interactive Spreadsheet,” Telemedicine and e-Health, April 2006.
d. https://www.cms.gov/Outreach-and-Education/Medicare-Learning-Network-MLN/MLNProducts/downloads/TelehealthSrvcsfctsht.pdf
Acknowledgements
The authors gratefully acknowledge grant funding for the project described by the Telehealth Network Grant Program (TNGP) #H2ARH2478, which is administered through the Office for the Advancement of Telehealth, Federal Office of Rural Health Policy, HRSA. The project officer was Carlos Mena, MS, who we thank for helpful comments during the project. The project director was Donna Dittman-Hale. The views expressed are those of the authors and do not necessarily reflect the opinions of the funder.





