EHR-RCM replacement and retirement economics: Driving ROI through data archiving
A recent report from the healthcare claims clearinghouse InstaMed says almost three-quarters of providers are unable to collect from patients within a month. This situation has prompted 58 percent of providers included in InstaMed’s analysis to identify patient pay balances as their greatest revenue cycle concern. Moreover, the statistics point to the reason for this concern: It has been reported that for every 30 days that payment languishes in A/R, the chances of collecting decrease by 30 percent, while the odds that patients will pay off their accounts fall to 6 percent by the time the fourth statement is sent. And for every dollar billed to a patient, nearly half will never be collected.
This problem can be exacerbated by inefficiencies in a provider’s EHR or RCM system—and indeed, as providers have sought to improve, upgrade, or replace their legacy systems, a key focus of these efforts has been to ensure the new or improved systems provide functionality that will improve A/R collections. Yet upgrading an EHR or RCM system or installing a new one is not a panacea for the A/R problem, because this very process poses its own challenges—including knowing what to do with patient A/R data housed in the legacy system.
Challenges with Legacy EHR Retirement and A/R Liquidation
As administrators at healthcare organizations begin to tackle these all-too-prevalent A/R problems, in addition to examining the extent to which their revenue cycle challenges are a function of inefficiencies in their legacy EHRs, they must also consider how disruptive it would be to bring in a new EHR. Their fundamental objective should be to implement a cost-effective and operationally more-effective alternative to the soon-to-be-retired legacy system without unsettling staff, users, and patients. Although this objective may seem obvious, it poses many challenges.
One challenge with a major upgrade that soon becomes apparent is that the legacy system cannot just be scrapped. Federal and state regulations require the storage of patient health information for at least five years, and often for more than a decade. It is necessary, therefore, that data housed in legacy systems be maintained. This requirement raises the questions of how to best maintain the current system without incurring more risk and additional costs, and whether it requires keeping the replaced billing system running in tandem with the new system.
Then, too, there is the matter of setting priorities. If organizations focus solely on the design and setup of their new system, they may inadvertently overlook cash protection. Many organizations assume they can handle their A/R with the legacy system internally right up to the moment of conversion. What they find about two months prior to the transition, however, is they cannot maintain solid performance due to the need to focus on training and the many well-documented implementation challenges that occur. (Consider, for example, a report of the experiences of Boston-based Dana Farber Cancer Institute.)
When transitioning to a new EHR or RCM system, healthcare organizations should understand that, from a financial perspective, liquidating cash in A/R is paramount. After the conversion, administration should focus on allocating the same resources toward liquidating A/R completely from the legacy systems by any means necessary, including issuing corrected billing for denied claims, submitting claims to secondary payers, engaging in collections activities, and writing off outstanding A/R. How an organization proceeds with this effort will depend on the organization’s approach to data archiving.
Active Versus Static Archiving: Relative Benefits
The healthcare IT research firm KLAS breaks data archiving into two methods: static archiving and active archiving.
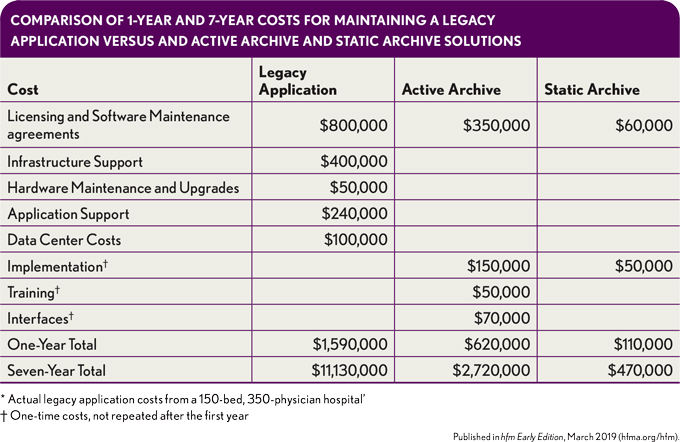
Static archiving provides only read-only access to records, with annotative capabilities. A static archive requires, in addition to implementation, only licensing and software maintenance agreements (SMA), and it is therefore, by far, the lowest-cost option, with a total estimated expense one-tenth of that for an active archive.
Active archiving provides similar functionality to a patient accounting system, but it also requires interfaces and additional training. Active archival solutions are specifically designed for a transition from a legacy system that is being retired to help the organization resolve outstanding A/R within that system. The risk associated with an active archive system is the relatively high cost often can exceed the amount of revenue it enables an organization to capture. An active archival system also requires additional spending on:
- Licensing and SMAs
- Infrastructure support
- Hardware maintenance and upgrades
- Application support
- Data center, plus additional costs for related implementation, training, and interfaces
Active archival systems also have limited utility for reconciling A/R in legacy patient accounts systems, typically lasting only about one year, after which the likelihood of collecting outstanding A/R becomes quite low. This assertion is supported by the industry average collection success rate and is based on the age of debt from the Kaplan Collection Agency, which indicates collecting on debt dwindles more each month an account is past due.
Advantage of Payment Plans
Healthcare organizations that use patient payment plans will find that such plans further reduce the utility of active archival systems relative to a static archival approach. A recent survey found that patients participating in payment plans are much more likely to repay, with 76 percent expressing an intent to fully repay the outstanding debt on time.
Moreover, third-party patient financial engagement companies, such as CarePayment, offer conversion of outstanding patient payment plans, offering lump-sum payments greater than 80 cents on the dollar. These companies also offer conversion of one-time aged A/R yielding lump-sum payments of 20 cents on the dollar. Thus, using patient payment plans also represents a significant opportunity for healthcare organizations to recover revenue when migrating to a new system.
The foregoing factors—for example, limited utility of active archives and the advantages of payment plans for rapidly converting aged A/R—suggest that there are distinct advantages to using a static archiving solution for meeting data maintenance requirements when transitioning from a legacy EHR or RCM system to an upgraded or new system
EHR and RCM System Transition Recommendations
To smooth the transition to the new system, all end-users should be prepared for the transition, and managers should have a good understanding of how the new functionality can be used to run their departments. These are fundamental characteristics of a high-performing revenue cycle, which invariably will experience less disruption during such a transition than a low-performing revenue cycle.
In sum, the key areas to consider for such a transition include the following:
- Development of a strategy for resolving legacy system A/R, including data archival and sunsetting the system prior to the cutover to the new system
- Creation of a denials management plan for resolution of the legacy system A/R, and for developing workflows after the new system’s implementation (e.g., refinement and/or development of a line-item denials workflow for improved tracking and reporting)
- Establishment of baseline key performance indicators for the most critical revenue cycle functions several months before go live, and assurance that the capability exists to capture these metrics before, during, and after the transition
- Development of clear patient communications regarding the upcoming statement changes and potential receipt of redundant statements
As healthcare organizations transition to new systems, it is essential that they reconcile payments as thoroughly as possible. The organizations must determine criteria for posting to the legacy system as well as the new system. A strong internal business team with clearly organized, well-managed accounts should be able to pursue this process independently.
Outside resources with experience in managing payment postings and reconciliation across both systems may be pursued. With proper process and guidance, internal and external staffs can complement each other to rapidly and accurately record all payments and adjustments in both systems.
The transition also may offer excellent opportunities to make other improvements in existing processes. Procedural areas such as self-pay collection, insurance-payer interaction and processing, and payment-and-posting practices could be made more productive.
Strategic and ROI Consideration
When retiring a legacy EHR or RCM system, a healthcare organization should address three important considerations with respect to handling outstanding A/R:
- The A/R profile (i.e., professional versus facility, insurance versus self-pay, and patient payment plans)
- Existing revenue cycle vendors (contracts/SMA plus costs to run and staff)
- Release of information/retention requirements
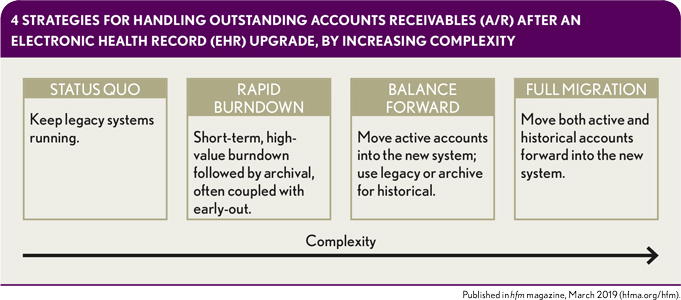
An organization also has the option of pursing any of four main strategies in such an initiative. These strategies, in increasing complexity, are:
- Maintenance of status quo (keeping legacy systems running)
- Rapid A/R burndown, often accomplished through an increase in resources devoted to collecting A/R, coupled with early-out collections, whereby a collection agency buys the debt.
- Balance forward, where a snapshot of current balances is brought into the new system.
- Full migration of all data from legacy application to new application, including replication of integration with external systems such as general ledger and materials management.
When evaluating strategies, attention to ROI is vital. For example, the cost of burndown should be less than the value of the outstanding A/R, and the cost of retiring the legacy system should be less than cost of maintaining the existing system, in terms of total cost of ownership. All essential inputs and outputs to the ROI calculation should be carefully considered, including the A/R profile, likely recovery rate, and existing and new solution costs (e,g., cost of IT, staffing, licenses, maintenance, and training).
Early-out and/or short-term reconciliation using the legacy system often provide the most cost-effective solutions when retiring a legacy EHR or RCM system. That said, there are some circumstances when it may make financial sense to adopt an archival solution to replace the functionality in the legacy system. Such an approach may be preferable, for example, when a large portion of A/R is outstanding relative to industry benchmarks, or where legacy systems are very large, with the result that software maintenance costs are exorbitant and A/R reduction is likely to take an extremely long time.
In short, by preparing A/R for conversion with the right acceleration and liquidation strategy up front, an organization can best protect cash flow and avoid adverse financial consequences.





