3 key enablers to implementing a successful clinical revenue cycle operating model
Hospitals and health systems should adopt a new operating model to support clinicians and clinical departments as they increasingly take on responsibility for revenue cycle activities focused on promoting revenue integrity.
With the advent of value-based payment models and new revenue cycle technologies, the revenue integrity function of hospitals and health systems can no longer be siloed within the walls of finance. Today, a new revenue cycle concept, called the clinical revenue cycle (CRC) is required that bridges clinical operations with finance, compliance, business operations and technology.
Revenue-integrity concepts under value-based payment, such as risk adjustment and payment based on hierarchical condition categories (HCCs), are commanding clinicians’ attention as never before. And with evolving electronic health records (EHRs), organizations are compelled to rely more than ever on clinical personnel to drive clinical documentation and to assume responsibility for accurate charge selection and coding, which ultimately determine payment. These changes signal the emergence of the CRC.
The CRC defined
The CRC is that part of a hospital’s or health system’s revenue cycle whose functions reside within the clinical side of the organization. It stems from strategies hospitals and health systems increasingly have pursued to support ventures into value-based contracting, including acquiring new technologies and employing physicians. With these strategies, clinical departments and clinicians assume responsibility for documenting the complexity of care and capturing hospital and physician charges that accurately reflect their services, productivity and revenue.
Specifically, with clinician involvement, the CRC focuses on the following discrete functions:
- Inpatient and outpatient clinical documentation
- Acuity capture
- HIM operations
- Professional and hospital coding
- Inpatient and outpatient clinical documentation improvement
- Utilization and care management
- Evidence-based practice compliance
- Denials management with respect to clinical issues
- Charge capture performance improvement
- Chargemaster, pricing and reimbursement
As they assume these new responsibilities, clinical staff who perform CRC-related activities require education, robust reporting capabilities and feedback on revenue integrity performance, which are offerings that many hospitals and health systems do not yet provide. A data-analytics-based approach can help enable necessary data entry in a way that fits into workflows and closes the loop with appropriate analytics. Meanwhile, ongoing communication of revenue performance between financial and clinical areas is required to ensure work is performed collaboratively at best-practice levels. To achieve sustainable revenue integrity, organizations must implement a CRC operating model that provides a strong, formalized framework for driving accountability, focusing on outcomes and fostering collaboration and communication.
The CRC operating model
The CRC operating model involves an interdisciplinary approach that bridges clinical care, technology and finance areas. Its broad purpose is to coordinate and optimize all revenue cycle activities that interface with clinical operations, taking into consideration all CRC functions and key stakeholders. Under the CRC operating model, clinicians play an active role in identifying, preserving and recovering revenue compliantly with a primary focus on business functions that are traditionally considered the “middle” of the revenue cycle, including:
- Inpatient and outpatient clinical documentation
- Hospital and physician coding
- Hospital and physician charge capture
To fulfill their new CRC role, clinical departments and clinicians must focus on appropriately documenting the acuity of each patient’s condition and leveraging workflow to enable the coding and charge capture of associated hospital and physician billable services, procedures, items and pharmaceuticals, with accurate pricing and charges. Then, to ensure the CRC is fully integrated, the organization must track the extent to which these efforts translate into adequate payment. To yield sustainable results, the approach must be proactive, interdisciplinary and transparent, with consistent communication and strategic feedback provided to all key stakeholders.
Key enablers for a successful CRC operating model include:
- Strong governance with clear decision rights
- Clearly defined business processes enabled by technology
- Culture that promotes teamwork and collaboration
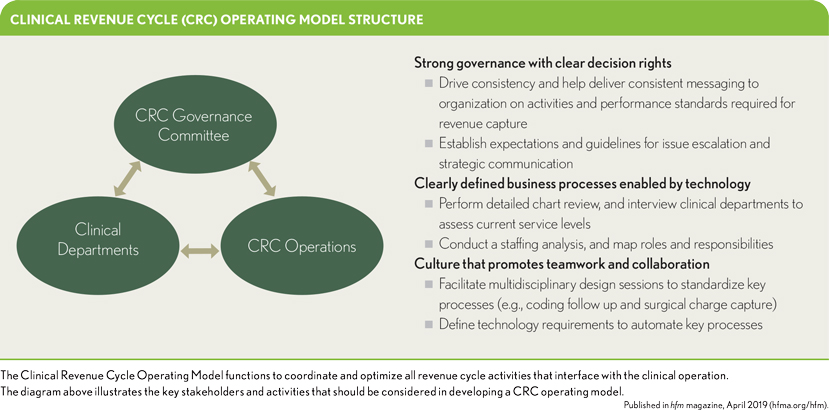
Strong governance with clear decision rights
To provide CRC oversight, organizations require a strong governance structure, championed by senior leadership and designed to accomplish four primary objectives:
- Ensure performance standards are consistently high across programs
- Effectively manage stakeholders’ expectations
- Facilitate processes for escalating and resolving issues
- Deliver consistent messaging to the organization regarding required actions and performance for effective revenue capture
The importance of this structure increases as evidence-based practices and other clinical factors increasingly become essential components of the revenue integrity function, requiring cross functional team to make key decisions and manage clinical quality.
To provide cross-functional oversight to the CRC, the governance structure should be led by a CRC governance committee cochaired by clinical, administrative and revenue cycle champions selected from each of the appropriate business process and clinical operational areas including the hospital C-Suite, physician leadership and representation from high-focus clinical service lines.
The governance committee should have a clear charter, decision-making authority, and defined roles and responsibilities. Leaders should have clearly defined decision rights that empower them to make decisions quickly and effectively.
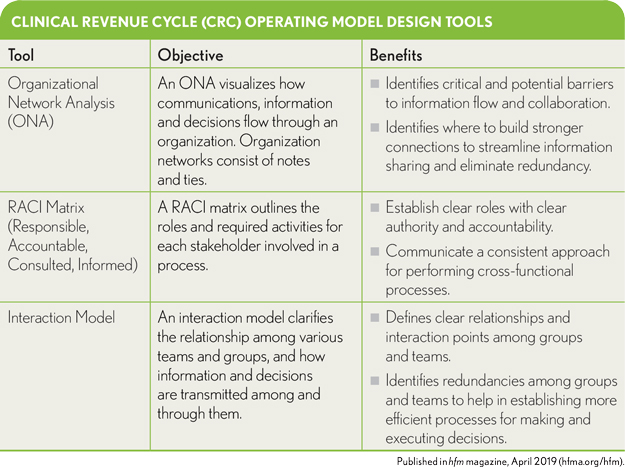
The committee also should make use of various available tools to inform the CRC operating model’s design and to drive ongoing model performance.
Clearly defined business processes enabled by technology
With the convergence of hospital and physician revenue operations and shared processes for optimizing revenue and quality performance, organizations need to ensure operational processes are well coordinated and integrated, and highly productive such as clinical documentation, charge capture workflow, audits, training and education, as well as feedback communication and reporting. To set the stage for developing and effectively managing such processes, and drive predictable outcomes, organizations should start with the following steps:
- Set clear process objectives
- Identify process owners and consumers
- Design well-integrated process interfaces
With respect to outpatient clinical documentation improvement and coding, for example, organizations should set a clear process objective of improving assignment of HCCs in primary and internal care departments. To ensure messaging is clear and to provide a unified voice to clinicians, process owners should be identified with clear roles and responsibilities, performance expectations and communication pathways. These individuals should include physician champions, clinical documentation specialists and consumers or end users (e.g., clinicians, clinical administrators, and quality and finance personnel). Finally, interfaces among the clinical documentation, coding, reporting, auditing and education processes should be created to provide for a seamless workflow.
All processes should be well documented, with documentation made accessible to process users to ensure they fully understand the processes, thereby helping promote accountability across the system. CRC functions should be centralized to allow for strategic control of business process performance and consistency. This centralized oversight should include space and planning for activities requiring face-to-face engagement on a local level, such as physician education and elbow-to-elbow support.
The CRC operating model should be supported by a dedicated EHR and analytics center that helps to establish a single source of truth for revenue performance data and enables staff to conduct clinical revenue cycle functions across the enterprise.
Culture that promotes teamwork and collaboration
Senior leaders can no longer afford to work in silos in today’s complex, dynamic environment, with the expansion of revenue cycle functions into nonfinance areas in healthcare organizations. The goal should be to create a symphony of experts who all play in harmony rather than a cacophony of experts who sound great alone but create a disorganized commotion together.1
Fostering a culture that promotes teamwork and collaboration is critical to CRC success. It also is critical that all stakeholders be committed to a team approach to driving culture change. Effective team interactions that promote flow of information and knowledge among clinicians, clinical operations specialists and revenue cycle managers are essential to achieving positive outcomes.
Key objectives in creating cross-functional teams are to provide quickness and agility for mounting collaborative efforts focused on meeting performance targets and to support the efficient flow of information through technology-enabled business processes. Regarding the latter objective, a network analysis of the multidisciplinary team can help promote a deeper understanding of the underlying connections and flow of information that shape how work is performed within and beyond formal business processes. Such insights can help optimize information exchange and improve overall coordination across the operating model.
Measures of success
A CRC program has the greatest chance to succeed if the governance committee is in regular contact with clinical departments and providers, monitors key performance indicators (KPIs) for a central viewpoint (see the sidebar below for a list of KPIs) and directs support consistently across the organization. Administrative, clinical and revenue cycle leaders should review KPIs monthly, quickly identifying lower-performing departments and holding them accountable during governance committee meetings.
Sidebar: High-impact clinical revenue cycle key performance indicators
To measure the success of their CRC operating model, the governance committee should consider the following three aspects of performance.
Communication. Expectations for communication should reflect a top-down leadership approach, where follow up is performed both electronically and verbally, and where there are clear guidelines regarding how clinicians and clinical departments can request help or reach out with questions. Providers and clinical departments should be kept current on performance requirements through frequent updates on charging, coding and regulations using clearly prescribed communication channels.
Reporting. Dashboards tracking KPIs should be shared electronically on a daily, weekly or monthly basis depending on the metric and business objective. Departmental leadership should be consistently informed of performance. Reporting also should be routinely provided in as close to real time as possible to all who are responsible for charge capture, charge reconciliation, coding or revenue monitoring to inform them of how they are trending against performance goals.
Support. The governance committee should assume responsibility for allocating resources, directing them to the areas of greatest opportunity and/or value to the organization. KPI and ROI analyses should inform this process and allow for dynamic staffing across the CRC to optimize revenue performance, compliance and clinician satisfaction.
The clarity and adaptability imperatives
Organizations that adopt a CRC operating model ultimately can gain clearer line of sight into their overall revenue capture performance to drive continuous gains amid significant change in internal and external business requirements. Implementing a CRC operating model requires a dynamic approach that can evolve constantly with ongoing market demands, changing regulatory shifts and the healthcare organization’s overall needs.
Sidebar: Revenue integrity: An evolving function for hospitals and health systems
Sidebar: 5 essential steps for driving revenue integrity through the CRC





