RCM recalibration: Patient financial experience captures leaders’ top focus
Healthcare finance leaders constantly navigate pressures to sustain growth, control costs and improve efficiency to enhance revenue cycle management (RCM). As technologies advance, patient expectations evolve and reimbursement rates remain elusive, these uncertainties make the balancing act even more precarious.
A recent survey shows that healthcare finance leaders are shifting their priorities and investment strategies to stay ahead of these challenges.
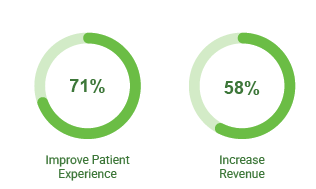
According to FinThrive’s third-annual Transformative Trends and Data-Driven Insights Report, 2025 signaled a structural recalibration in how healthcare leaders define financial performance. For the first time since FinThrive began conducting this survey, patient experience surpassed revenue growth as the top strategic priority among revenue cycle leaders, with 71% of executives ranking it as their most important goal.
This shift reflects a growing recognition that revenue growth is increasingly achieved through experience-driven operational design which drives patient loyalty over traditional volume-based strategies. In fact, the top-performing organizations recognize that these two priorities are intertwined, because better experiences attract and retain more patients, protect market share, reduce friction and stabilize margins over time.
“Patient experience is a revenue growth goal,” said Jacob Collins, vice president of revenue cycle at Phoebe Putney Health System in Southwest Georgia. “In other words, experience doesn’t replace revenue; it’s how you obtain it.”
Instead of choosing between patient experience and economics, leaders are increasingly relying on AI, automation and integration to reduce friction across the revenue cycle — leveraging technology to combat denials, streamline authorizations, improve documentation and enhance every other touchpoint along the way.
Survey results also reveal how healthcare finance leaders are connecting patient loyalty, RCM efficiency and automation into one cohesive strategy for operational resilience.
Workflow reality check
Until recently, many health leaders assumed that the patient experience referred only to clinical care. But increasingly, organizations understand that it’s the entire experience — not just great clinical care, but a smooth onboard to the organization, correct and timely data capture and convenient ways to pay — that distinguishes them, according to Collins.
“Healthcare is complex, and there are a lot of different touchpoints throughout the revenue cycle between scheduling, authorization, eligibility and financial clearance that can create ‘interaction fatigue,’” Collins said. “Reducing the friction can help improve that experience.”
The interaction fatigue of manual revenue cycle workflows can frustrate patients who face delays or redundant payer approval challenges; and it can also wear on staff, who are prone to burnout and even leave because of the heavy administrative burden. Each point of friction carries financial implications as patient and staff attrition leads to revenue leakage, slow cash flow and strained resources — triggering a spiral of poor financial performance.
Fortunately, innovative technologies offer effective solutions to smooth these workflows and improve the experience for patients and staff alike. Not surprisingly, automation and AI adoption is surging among health finance leaders, with three out of four citing automation as a top initiative for 2026 and more than half (56%) reporting AI/automation as their prime investment focus.
Patient experience takes the lead
71% of financial leaders rank it as their top focus, compared to 58% who chose revenue growth.
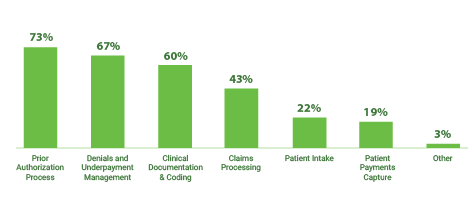
The top three use cases for RCM automation focus on streamlining these bottlenecks by targeting the prior authorization process (73%), denials and underpayment management (67%) and clinical documentation and coding (60%).
“We’re implementing targeted, smart, efficient automation and AI capabilities,” Collins said. “That does two things: One, it helps control expenses in terms of the resource component, and two, it allows our team to focus on more complex issues and patient-centered interactions.”
Likewise, nearly six out of 10 leaders surveyed agreed that the primary driver behind AI investment is alleviating administrative burdens, with the goal of minimizing errors and turnaround times while freeing staff for more important work.
In fact, Collins said, the biggest risks of dismissing revenue cycle automation are staff burnout and turnover.
“As leaders, we need to take care of our staff by giving them the tools to do their jobs more efficiently,” he said, “and process automation is one of the tools you can use to make their jobs easier.”
After all, the same manual tasks that drain staff also degrade patient experience, which will ultimately deplete the bottom line.
“If I’m not automating my front-end processes, my patient access team is not going to have the most effective tools. If they don’t have the most effective tools, then patient experience is going to decline, and people are going to go where it’s easier to get in, where authorizations are coming more quickly and estimates are more accurate, where there is less friction,” Collins said. “As those front-end processes bottleneck, your revenue on the backend is going to decrease.”
Where do healthcare finance leaders believe AI and automation will have the most significant impact?
AI and automation will most significantly impact:
Targeted investments
As part of healthcare’s RCM recalibration, organizations are redefining technology’s role in the revenue cycle. The survey results show leaders stepping back from short-term fixes like cost cutting — which ranked lowest among this year’s strategic goals at 36% — to focus instead on strategic technology investments that drive growth.
According to a separate study from FinThrive and HFMA, nearly half (47%) of healthcare organizations have already implemented multiple AI or automation tools, while another 38% are in early pilot stages. Given the vital role that technology plays in enhancing patient experience and boosting the bottom line, deciding where and how to apply technology represents a challenging decision.
“We’re always looking to cut costs and be more efficient where we can so we can continue to reinvest in our teams so that we can provide the best patient experience possible,” said Miguel “Mike” Vigo IV, chief revenue cycle officer at UC San Diego Health in California. “When it comes to AI, we’re very meticulous in how we’re balancing our technology investments to add efficiencies, so we can grow organically without increasing costs.”
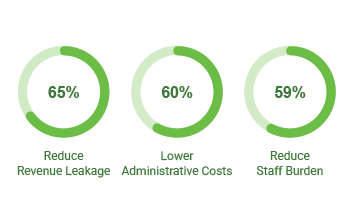
The Transformative Trends report revealed the top motivations for investing in automation, which include reducing revenue leakage (65%), lowering administrative costs (60%) and reducing the burden on staff (59%). For organizations like UC San Diego Health, tech investment decisions often consider all three of these factors simultaneously.
As organizations reassess their technology strategies, many are seeking clearer benchmarks to evaluate maturity and identify gaps across the revenue cycle. One approach that Vigo, like hundreds of other finance leaders, is using to bring structure to that assessment is the Revenue Cycle Management Technology Adoption Model (RCMTAM) developed by FinThrive in partnership with HFMA.[1] The framework leverages extensive benchmarking data — more than 30,000 data points — from healthcare finance leaders to help organizations benchmark their tech stack maturity, pinpoint gaps and prioritize opportunities where AI-enabled technologies can drive measurable improvements.
“The RCMTAM tool provided us with the clarity and direction we needed to either improve our metrics considerably or maintain transparency on stable KPIs,” Vigo said. “It’s been invaluable in helping us pivot resources and realign strategies.”
Of the several hundred RCMTAM surveys that have been completed, at least half of them have identified patient access as a potential gap, estimates Hemant Goel, president and CEO at FinThrive.
“That tells me the industry is somewhat immature on the front-end, and there’s an opportunity to modernize the patient experience,” he said.
The Transformative Trends survey confirms this observation, revealing that hospitals are investing in patient experience initiatives that influence financial outcomes — such as enhancing scheduling and self-service tools (52%) and improving payment processes (41%). Digital conveniences like these are no longer a competitive advantage; they are table stakes. Healthcare consumers demand seamless scheduling and flexible payment options, delivered with the same ease they experience in retail environments.
Health systems that meet these expectations see measurable gains not only in patient experience scores, but also in downstream financial stability. Failing to weigh the importance of the patient experience and focusing solely on revenue when making tech investments can deter success, puts health systems at risk, destroying both patient volumes and profit margins, Vigo said.
“If you deprioritize the patient experience, you’ll start to see your volumes decrease and then all of a sudden, your market share will drop as people reschedule to other places,” he said. “You have to be very methodical with your technology investments to make sure they benefit both your revenue and your patient experience.”
Top motivations for automation investment
Technology transformation
Looking ahead, the organizations that thrive will be those that focus on a combination of clinical and financial pathways for their patients, Goel said. This is best supported by connecting operational efficiency, patient loyalty and intelligent technology applications into a cohesive strategy, recognizing that long-term financial stability relies on a seamless experience.
For example, a collaborative and cohesive approach leverages technology to strengthen patient experience. Such an approach enables hospital employees to use intelligent tools that effectively and efficiently address potential issues for patients, deepening patient loyalty while strengthening financial outcomes.
Successful transformations require deliberate alignment across people, processes and technology along with a strategic approach that seeks to deploy the innovative benefits of an RCM platform over time, according to Collins.
“You don’t have to go ‘all in’ immediately,” Collins said. “You can take incremental steps and do some simple process automations to make your employees’ lives better, and that’s the key. A happy, effective workforce helps improve your patient experience and ensures patient loyalty.”
Incremental progress is practical, but success will depend on ensuring each investment reinforces a cohesive operating model. Leading organizations eliminate friction from the revenue cycle in an automated way, recognizing that patient experience, workforce sustainability and resilient technology should function as one integrated financial strategy.
“It’s time to take inventory of your current capabilities, and the RCMTAM is one way to do that,” Goel said. “There’s a ton of friction in the revenue cycle, and technology plays a role in removing that friction to enable it to run smoothly. You must have the people, processes and technology in place to wrap your arms around the patient financially as well as clinically.”
Even the most sophisticated automated workflows are only as reliable as the security protocols protecting them. Amid rising cyber risks, tech-savvy leaders are realizing that revenue cycle stability and data security are now inseparable.
According to FinThrive’s Transformative Trends and Data-Driven Insights Report, 85% of organizations have already modified their RCM technology strategies to protect against cybersecurity threats and clearinghouse interruptions.
“Never have I been as concerned about security and compliance as I am now,” said Collins. “Automated processes are only going to work if they’re built in a system that’s secure, so it’s imperative that not only my internal systems but also my vendor partners maintain vigilance around data security.”
As catastrophic cyber events across the industry have demonstrated, a single ransomware attack or system outage can completely halt insurance verification, authorizations, claim submissions and eligibility checks — seriously disrupting cash flow throughout the revenue cycle.
“If you can’t recover and send out claims quickly, the money will take months to come back,” said Goel. “And if you don’t have the cash reserves to endure the outage, that can be devastating to your profitability.”
In addition to an internal security team that ensures strict compliance with industry standards and certifications such as SOC, NIST, CSF and HITRUST, standby claims and standby eligibility solutions provide hospitals with critical backup capabilities during unplanned revenue cycle interruptions.
“Cybersecurity threats are very sophisticated, so it’s not a matter of if, but when,” Goel said. “It comes down to recovery: How quickly can you get your systems back online and return to normal operations? That timing is critical. The more you are down, the more the revenue is at risk.”
As new tools have emerged to enhance every step of the revenue cycle, the solutions tend to stack up — adding complexities and duplications that present stumbling blocks to smooth technology integrations. In fact, FinThrive research reveals that the average hospital uses between 15 and 30 vendors just to manage various aspects of RCM.
“EHRs were never designed to submit bills or process payments,” Goel said, “so as they started incorporating things like prior authorization and insurance eligibility, third-party solutions had to bridge that gap between payer, hospital and patient. That has caused an explosion of RCM tools in the market.”
Now, as part of the RCM recalibration identified in FinThrive’s Transformative Trends and Data-Driven Insights Report, healthcare organizations are trying to reduce these complexities by consolidating vendors, with 71% planning to reduce vendors from their mix as they move toward a more unified RCM platform. This consolidation helps lower the cost to collect, simplify workflows, reduce risks and foster stronger accountability across the revenue cycle.
“There’s a lot of duplicity between RCM technology services, and the larger footprint you have, the more risk you have,” Goel said. “If everything’s all in one place, it’s a lot easier to understand how the eligibility transaction relates to the estimate, to the charges, to the bill, to the claim and ultimately to the payment. It becomes much more actionable to be alerted through analytics on one area versus going to 12 different places to collect those insights.”
This industry-wide shift toward vendor consolidation signals that organizations are looking for strategic, long-term partnerships with trusted vendors, rather than a patchwork of quick-fix point solutions. Organizations that seek to drive a lower cost to collect through effective financial pathways are well-positioned for financial sustainability for the future. The trends and initiatives identified in this survey drive toward that change and will enable improved financial outcomes for years to come.
About FinThrive
FinThrive delivers a comprehensive suite of revenue cycle solutions powered by a single, unified data foundation built for scale and intelligence. Organizations can adopt the RCM capabilities they need—from clearinghouse and claims management to denials prevention, patient engagement, insurance discovery, and analytics—while benefiting from shared data, embedded AI, and consistent workflows across the front, middle, and back of the revenue cycle. By replacing fragmented point solutions that limit visibility and drive costly inefficiencies, FinThrive enables revenue teams to unlock greater intelligence as adoption expands—where each added capability strengthens performance, accelerates cash velocity and predictability, and compounds financial value over time. Visit finthrive.com.
This published piece is provided solely for informational purposes. HFMA does not endorse the published material or warrant or guarantee its accuracy. The statements and opinions by participants are those of the participants and not those of HFMA. References to commercial manufacturers, vendors, products, or services that may appear do not constitute endorsements by HFMA.
Footnotes
[1]. Revenue Cycle Management Technology Adoption Model, FinThrive, www.finthrive.com/rcmtam.





