40% of hospitals reconsidering traditional budgeting amid pandemic: HFMA poll
An HFMA survey sponsored by Strata Decision Technology found that two-fifths of hospitals and health systems were looking to overhaul their traditional budgeting process, with one in five moving to rolling forecasting.
Two in five hospitals are actively moving away from traditional budgeting or considering doing so in response to the COVID-19 pandemic, the survey found.
A large number of hospitals and health systems in 2020 joined a movement away from traditional annual budgets in response to the financial planning disruptions caused by the pandemic and some associated policy responses. Voluntary and involuntary suspensions of elective procedures disrupted revenue streams across the sector and led many to look for planning approaches that could better take into account rapidly evolving financial developments.
That shift was identified in the October 2020 HFMA-Strata survey of 132 healthcare finance executives. The survey found:
- 21% are considering or have implemented rolling budget forecasting
- 20% are thinking of future budgets in
different ways
How has COVID-19 affected changes to your financial strategy?*
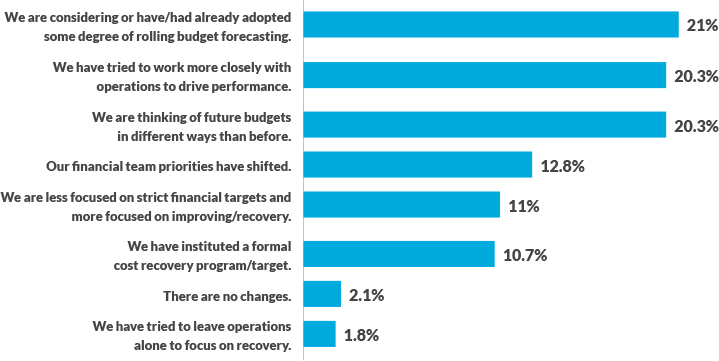
*Question asked of all survey participants
Source: HFMA-Strata Research Study, October 2020
“It comes down to uncertainty in the face of a rapidly evolving market,” said Frank Stevens, vice president of financial planning at Strata. “Organizations struggle to accurately predict the impact of COVID-19 and how long that impact will continue. Trying to create a budget plan for 12 to 18 months from now is basically impossible.”
St. Joseph’s Health, a regional not-for-profit healthcare system in Syracuse, New York, was one organization that shifted its forecasting approach in 2020.
In March, when the pandemic hit, St. Joseph’s was far along in developing the budget for FY21 (which began in July 2020) using a traditional static budgeting methodology with monthly forecasting, said Meredith Price, CFO for St. Joseph’s, which is part of Trinity Health.
“As we approached FY21, we recognized the budget that we had begun earlier in the spring really didn’t hold much credence in terms of what we were seeing at the time,” Price said. “So, at that point, we decided to do a rolling forecast and focus on a quarterly basis because things were changing so rapidly.”
Her organization had previously discussed transitioning from a static budget to rolling forecasts but had decided not to make the change.
“This gave us the burning platform to pull the trigger on it,” Price said.
Care New England Health System in Rhode Island has a similar story. It had decided to move to a rolling forecast before COVID-19, but the pandemic served to highlight the need for this approach to financial planning. As of press-time, the health system was finalizing its first quarterly iteration of a rolling forecast to supplement its traditional budget for FY 2021. Starting in FY 2022, it will rely entirely on a rolling forecast.
“An annual budget becomes stale pretty quickly,” said Gail Robbins, senior vice president of planning and finance at Care New England. “Comparing actual performance to the budget becomes less and less meaningful as the year goes on. A rolling forecast allows us to stay on top of and respond to current events.”
Use of rolling forecasting
Approaches to rolling forecasting by those that have adopted or considered it varied widely. The survey found:
- 33.9% were considering adding rolling forecasting to their budget process
- 21.4% had used it to replace their annual budgeting process
- 12.5% were considering it as an annual replacement for their budgeting process
- 8.9% were considering it as a short-term replacement for their process
Prior to COVID-19, Overlake Medical Center and Clinics in Bellevue, Washington, had only begun to explore a rolling forecast as a supplemental resource to the annual planning process. However, the pandemic expedited the need to move forward.
“With COVID, there was an immediate need to understand how our current financial results translate into new trends,” said Jenna Bevilacqua, MBA, director of finance at Overlake. “Our goal was to identify changes in trends, have the ability to model multiple scenarios and use the forecast to assist in development of mitigation strategies that we can act on.”
Overlake officially rolled out its first rolling forecast this past fall. It will continue to complete a full annual budget to provide department-level goals, but it plans to routinely update the rolling forecast quarterly beginning in 2022 so it can immediately act on any trends.
Timelines to implementation
Among hospitals and health systems in the survey group that were still considering broad use of rolling forecasting, 69% said they were starting with piloting or were testing its use.
The timing of a move toward rolling forecasting among those considering it varied widely:
- 52.8% – within six months
- 16.7% – in 12 months
- 11.1% – in 18 months
- 19.4% – in more than 18 months
At VCU Health System in Richmond, Virginia, a rolling forecast has been in place for three years.
“Even before COVID, there were a lot of moving parts — legislative actions at both the state and federal levels that were impacting our budget,” said Jeffrey A. Setien, director, financial planning and analytics. “When we had a static budget, we couldn’t be as nimble. A rolling forecast gives us an opportunity to keep freshening the budget and plan based on the most current data we had.”
Medicaid expansion was one such change. The health system knew that more patients would likely become eligible for Medicaid, but it didn’t know specifically how many — and how those transitions from self-pay and charity care to Medicaid would affect revenue. That’s where having a rolling forecast helped.
Why make the move?
One advantage of a rolling forecast is increased agility. “You don’t just develop a plan and lock in on it, said Strata’s Stevens. “You keep revisiting the plan as changes materialize. It’s more accurate because you refresh your plan as more information becomes available. The approach provides much greater agility.”
The shift to rolling forecasts has given St. Joseph’s increased agility during the pandemic and has been used to drive daily performance, Price said. The availability of rapid data allowed the organization to identify when financial performance stemming from volume changes was below or beyond expectations, for example.
For instance, after the health system had to suspend elective cases during spring 2020, it focused on ramping back up in the summer. But its estimates on the how quickly it would restore volumes proved too conservative.
“With the rolling forecasts, we found we were doing better than we had expected from a recovery standpoint,” Price said. “We were able to put in place different reporting mechanisms to respond to that, both from a staffing perspective and a revenue perspective, and then reset our target. So, we weren’t shooting for these lower targets that we originally thought we were going to hit and then were quickly outpacing and exceeding.”
The rolling forecast allowed the organization to continually reset its financial targets toward more realistic goals and press for continued improvement. The result was not only better performance, but also engagement of areas directly impacting the ability to perform, Price said.
For Care New England, being able to account for unanticipated changes in volume has been critical. “Rolling forecasting allows us to routinely update our financial targets in response to changes in volume,” said Robbins. This includes being able to account for the effect of additional waves of COVID-19 on inpatient and outpatient volumes and related revenue and expense.
At Overlake, a rolling forecast has also enabled greater flexibility in terms of adapting to the pandemic and its financial impact.
“This new process allows us to update our budget assumptions based on the latest trends, and we are able to provide revised metrics and year-end goals to our board,” Bevilacqua said.
At VCU Health System, having a rolling forecast enables cashflow management during a time of significant investment in infrastructure, including an expansion of ambulatory services, a new EHR, a new children’s hospital and more.
“These substantial investments are all taking place at the same time, necessitating a nimble response and forward-looking information,” said Michael C. McNeely, FHFMA, CPA, CSMC, vice president of finance at VCU Medical Center.
A rolling forecast is also more efficient than a traditional annual budget because it is less granular and thus takes less time to create, said Stevens. “You can condense the planning process from five months to a month or even weeks per iteration of the rolling forecast. The efficiency gains are dramatic.”
Finally, with a rolling forecast comes greater accountability. “Organizations that successfully make this shift are also adopting a continuous improvement or period-over-period improvement approach to performance management,” Stevens said.
Challenges and lessons learned
Transitioning detailed department-level budgets to a rolling forecast centered on high-level trend data had its own set of challenges, said Bevilacqua. In particular, Overlake needed to educate leaders on the rolling forecast process, how to analyze trend data (rather than transactional data) and how to correlate trend data with the annual budget.
Care New England also faced similar challenges, though Robbins said a thoughtful and collaborative approach helped. “We spent a lot of time upfront thinking about what the model itself was going to look like. What are the key expenses and drivers that affect the bottom line that we need to incorporate into the model?”
It was a similar story at St. Joseph’s. Price found education on the use of rolling forecasting was needed for both management teams and organizational leadership. The focus also was on developing the right KPIs to track and monitor going forward.
Price pressed leaders to identify, “‘How can we keep improving performance, which is going to be KPI-driven, as opposed to just looking at a number or whether we are on budget?’ [The process] will be more ratio- and KPI-driven.”
In FY22, St. Joseph’s plans to adopt a form of rolling forecasting at the department- or service-line level.
Another challenge is that although the goal of a rolling forecast is to be able to pivot quickly, it’s often easier said than done, said McNeely. “How fast do we ask the organization to shift and change? For a large organization like ourselves, it’s hard to move quickly.”
Finally, some organizations may need to overcome misconceptions related to rolling forecasting — particularly the idea that financial targets change monthly or quarterly, said Stevens. “Most organizations that take this approach still lock in on an annual target,” he said. “Then they use the rolling forecast to see where they are in terms of meeting that target and what they need to do to get back on track.”






