How to future-proof your travel nurse and clinician staffing
In fiscal year 2021, an innovative in-house travel staffing approach saved Trinity Health $32.1 million, and it has saved another $33.9 million in the first two quarters of the fiscal year 2022. Trinity’s experience offers an important lesson for other health systems on how to address ongoing clinician staffing challenges that were exacerbated by the pandemic.
The delivery of healthcare as we know it had not yet been completely upended by COVID-19 when Trinity Health started building its internal travel staff solution for nurses and clinicians. Now, two years into the pandemic, Trinity has a fully developed cross-system program in place that embodies new perspectives on teaming. The program, called FirstChoice, is enabling the 88-hospital system to recruit mobile staff and schedule them at lower costs because they’re retained within its system — thereby securing Trinity’s ability to deliver high-quality care into the future.a
“Even prior to the pandemic, like most health systems, we were using contract labor — and more than we wanted to,” said Gay Landstrom, PhD, RN, NEA-BC, FACHE, senior vice president and chief nursing officer (CNO) for Trinity Health.

Trinity Health previously had operated float pools that would look familiar to most health systems. Many clinicians have long objected to the rigid scheduling requirements that characterize this traditional approach, however, and the pandemic delivered a gut punch that accelerated staff’s intolerance for rigid scheduling requirements and increased their demand for flexibility. In addition to falling short on clinicians’ demands for flexibility, float pools are not designed to work across multiple geographies, further limiting their utility for health systems.
“Our staff who need flexibility see traditional restrictions as a potential deal-breaker. It’s old thinking,” Landstrom said. “Any health system that doesn’t recognize that a significant chunk of the workforce needs flexibility must acknowledge that those potential employees will seek out and find that flexibility elsewhere. We estimated that in our own backyards about 25% of the clinical labor force would never work directly for Trinity Health because of those rigid permanent employment structures.”
Trinity Health wanted to increase its appeal as a local employer while reducing its reliance on contract staffing and agencies. This imperative became the impetus for Landstrom to champion an expansion of Trinity Health’s regional pilot to build an internal travel pool or regional hiring marketplace. The initiative had been in an incipient stage for about 10 years as a team of human resources, nursing and finance leaders gathered evidence to make the case not only for creating regional hubs across the enterprise, but also for organizing them into a systemwide program. The goal? To create a true in-house traveler program that offered the flexibility traveling clinicians were finding only at staffing agencies.
And then came March 2020. The loose-knit patchwork of full-time staffing, structured float pools and high-cost agency relationships crumpled under the catastrophic disruption wrought by the COVID-19 pandemic.
“We realized we might need to move 60, 80, 100 people into a location that previously didn’t use a lot of contract labor to accommodate surges,” Landstrom said. “And we needed to do it fast, across multiple geographies. That was new for us.”
With many pandemic- and personnel-related variables out of its control, the healthcare organization recognized quickly that its proprietary travel staffing model was one lever it could actually pull to make a difference.
“Some of our leadership had been on the fence about the travel program until the pandemic hit, but it quickly became clear this might be exactly what we needed,” Landstrom said. “Not only didn’t we pause the program, but our team realized we needed to accelerate it.”
In March 2020, Trinity leaders deployed additional resources to more rapidly implement the health system’s regional hiring marketplaces. And they began recruiting with the idea of giving individuals a choice of a rotation of four, eight or 13 weeks within a region or across the system.
In fiscal year 2021, the savings from Trinity Health’s in-house travel staffing approach amounted to $32.1 million. Today, more than 1,000 FirstChoice staffers are employed in long-term assignments (LTAs), and 1,815 colleagues — mostly registered nurses but also respiratory therapists, surgical technicians and others — were hired in 2021. The approach also has dramatically altered how Trinity Health views the future of the healthcare workforce and the potential that employees will increasingly see the health system as an attractive employer.
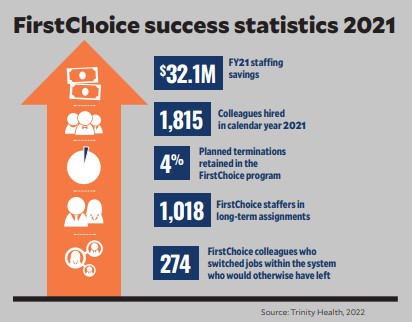
Trinity Health built FirstChoice with job candidates’ desire for flexibility top of mind and a commitment to the internal buy-in that would be required for long-term success. Its approach was characterized by adherence to the following four guiding principles.
1 Build an internal team with an eye for long-term, cross-department alignment. “Trinity Health sought to make itself a destination employer for all clinicians and for non-clinician colleagues, including those who may need to take a month of the year to care for an elderly parent out of state,” Landstrom said.
That goal made it clear who would need to be part of the planning.
“Finance and human resources need to be locked at the hip with clinical leadership,” she said.
Landstrom and Trinity’s chief of human resources, Ed Hodge, were tapped as co-sponsors of the program, with a new cost center that reports to both of them and responsibility clearly defined as shared between clinical operations and HR. Pilot programs provided pro forma numbers for what promised to be an unprecedented process. The pilots also drove tight collaboration between Landstrom as operations owner and financial leadership to document early insights and anticipate the outcomes of various scenarios:
- An internal communication action plan ensured that strategy, operations and finance teams had all been informed about the pilot and its goals.
- The existing travel planning team was also brought in for input.
- The program was structured to allow for including other workforce lines, such as food service and environmental services, in the future.
Together, this team worked through pay structures, expectations for floating staff among facilities, staffing software to connect staff and make assignments, minimum competency and clinical experience requirements, and a balance of benefits that clarify the appeal for existing staff of remaining in a permanent position.
2 Connect with candidates. Trinity Health added technologies to modernize and speed up its hiring process. Reducing time-to-hire would require evolving legacy protocols and processes as phone tag and voicemails would not play well in a future-proofed hiring approach.b Trinity Health also would need to place a premium on talking with high-quality candidates instead of simply weeding through applications to vet candidates.
“Contract workers have many offers in front of them,” Landstrom said. “They weren’t going to tolerate an overly bureaucratic process. If we took even 24 to 48 hours to get back to them, that could be too long for hero nurses who are motivated to run to the fire and intolerant of delay.”
New automation capabilities, streamlined applications and text and mobile app capabilities were deployed to allow Trinity Health to vet candidate qualifications faster, and new chat capabilities gave them faster ways to reach and move forward with strong-match candidates.
“We needed to act like a very responsive external contract agency. We needed talent acquisition professionals to be jumping and using new, faster communication approaches to vet and bring in strong candidates,” Landstrom said.
3 Pilot and scale. For Trinity, bringing the CEOs of 90+ regional health systems and service lines on board was a much heavier lift than implementing a regional program. COVID-19 served as the impetus to move from an informed pilot to a cross-regional jobs marketplace. When the time came to move, pro forma data and a ready team helped them decide not just to move forward, but to do it quickly so they could maneuver as many as 100 colleagues into locations that previously didn’t use much contract labor.
The FirstChoice structure also helped redeploy staff who were not being called in because of postponed elective surgeries and other efforts to reduce hospital load. At the same time FirstChoice was ramping up, hiring leaders were adjusting regional scheduling and querying colleagues across Trinity Health’s
25 states to ask colleagues if they would be willing to serve temporarily at another ministry within the system.
4 Stay smart on compensation. A FirstChoice nurse receives a higher salary but lower benefits. With COVID-19 driving up compensation, Trinity Health realized it needed to closely monitor shifts in travel nursing compensation and respond to changes quickly.
“Nurses might be willing to work for us for a lower rate, but we had to stay on top of market rate changes and use new tools to track them in almost real time,” Landstrom said. This regular monitoring kept Trinity Health’s pay rates competitive, and the health system was able to ensure its internal resource pool was still more cost-effective than an external staffing agency.
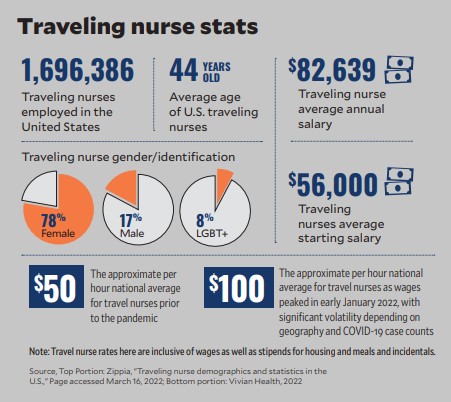
FirstChoice’s in-house resource pools tap a new group of job candidates — those who may not have considered working permanently — and show them what it might be like to try out different roles within Trinity Health. FirstChoice employees inherently get visibility into the Trinity experience and become high- priority candidates for permanent staff recruiting efforts.
This is an important lesson for any health system considering such an approach: Demonstrating new flexibility can open them up to additional job candidates for urgent near-term needs and can seed goodwill for these candidates to “test you out” and choose your health system for a permanent position in the medium and long term.
Most important for Trinity Health was reframing its understanding of its potential to attract teammates from labor pools that previously were closed to the health system.
“Agency and travel staff can’t be seen as outsiders anymore,” Landstrom said. “FirstChoice people are Trinity Health people, supporting our mission and our values. They’re not external, and that’s been a transition for our system. This is an entirely new way of engaging with a vital workforce.
“The historical lack of access to these labor pools has been an accepted foundational belief. But the workforce is shifting. Health systems need to shift with it.”
A new response to a long-standing need
Despite the unprecedented challenges U.S. health systems face today, they have an opportunity to take a “glass half-full” approach. Health systems are rethinking what it means to be a desirable employer. They are responding now to demands that the nursing community has been making for decades. Innovation is accelerating by necessity — with automation impacting candidate recruiting, communication and qualification. In the case of in-house resource or travel pools, health systems are discovering how to improve retention and use their own backyards as a new recruiting ground. If they embrace these opportunities, we will see the emergence of a more capable and resilient healthcare ecosystem that is much better prepared to absorb the next shock to the system.
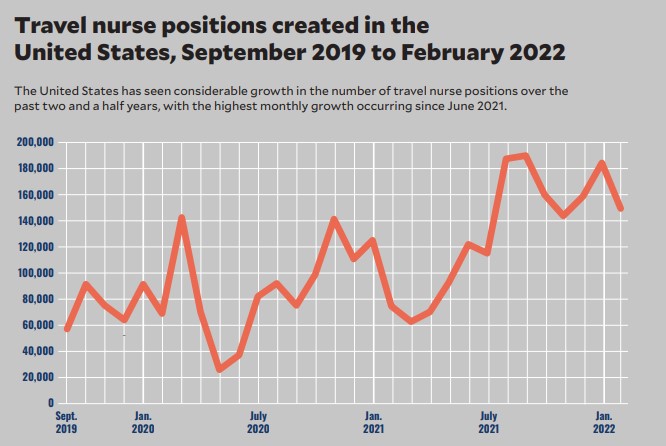
Footnote
a With 6,800 employed physicians and other clinicians across 88 hospitals and 131 continuing care locations, Trinity Health serves 30 million people across 25 states.
b Traditional outreach from health systems is phone tag all the way, and even if it works well and a candidate is made an offer, it can take another 30 to 45 days to verify licenses and certifications and get the teammate in the door.
Why health systems should revisit their historical approach to temporary staffing
Historically, health systems have seen temporary staffing as a useful strategy for filling staffing gaps and maintaining safe staff-to-patient ratios during planned permanent staff outages, like family and sick leave, or expected seasonal surges and unplanned situations such as regional outbreaks of COVID-19.
Although permanent staff come with the cost of benefits and overhead, temporary staff come with staffing agency premiums. These premiums can add 25% to 30% to the health system’s cost for a traveler, none of which accrues to the individual clinician.
COVID-19 drove those costs to the stratosphere: Same-employer travel nursing job openings were up an average of 54% in Q4 of 2021, compared with the same period pre-pandemic in 2019. Average weekly pay for these positions has nearly doubled for travel nurses across all specialties, and is up 94% for travel ICU nurses, according to analysis of job openings in the Vivian Health marketplace. But that’s not the only reason health systems have for years sought to address staffing concerns:
- Staffing shortages can lead to violations of safe staffing guidelines, with implications not only for patient outcomes, quality rankings and payments but also for clinician performance, job satisfaction and mental health.
- Staffing agency costs can be unpredictable, wreaking havoc on a carefully planned balance sheet.
- Despite their broad experience, travel nurses often have limited time to orient to their units, making it likely peers on the floor will see them as outsiders.
- Amid COVID-19, credit rating agencies are increasingly scrutinizing nurse staffing, per the neutral outlook from Fitch and the negative outlook Moody’s assigned to the nonprofit and public health sectors in December 2021.a
Picking up extra shifts within a system can allow clinicians to maintain a stable home life while still enjoying a travel structure’s variety, flexibility and increased compensation. And bringing in known colleagues who are trained within a system’s protocols can smooth onboarding and ease the travel-versus-permanent dynamic that can cause friction within departments.
Systemic hiring challenges predating COVID-19 will most certainly continue post-COVID. Efforts to expand old-school float pools and build systemwide travel pools have largely been unsuccessful because of significant recruitment challenges, including the following.
- Traditional search processes are too slow. Most health systems simply aren’t set up to hire quickly. It can take months to get the right nurse in the door, aggravating shortages, affecting safety ratios and damaging revenue performance while these positions remain unfilled.
- Travel nurses may regard permanent positions at a local hospital as not viable due to a lack of flexibility. Included in this pool can also be those types of individuals who tend to “run toward the fire”— the clinician heroes who find the greatest value in going wherever there is the greatest need, but who lack the visibility to identify those needs within their local system.
- Traditional job boards commoditize clinicians. Job postings tend to be vague and lacking in financial detail, resulting in applicants who aren’t strong matches. Candidates also rarely can complete a universal profile that enables them to upload their qualifications only once to apply for multiple positions across employers. More often, they are forced to reenter the same information repeatedly. It’s no wonder up to 70% of candidates don’t complete the application process and their candidacy “dies a death by applicant tracking system.”
- Nurses seeking open positions are often stymied by complex and opaque hiring processes. A lack of clearly spelled-out qualification requirements, for example, results in much wasted time for both employers and candidates.
- The pace of hiring has accelerated with the use of new technologies, but most health systems haven’t caught up. Candidates expecting to hear responses within a day aren’t willing to wait when they have multiple offers on the table.
Footnote
a Shields, Y., “Rising labor costs dampen hospital sector’s pandemic recovery prospects,” The Bond Buyer, Dec. 13, 2021.





