The Hospital of the Future Part I: Can healthcare leaders deliver a healthier future?
As high-tech care meets old-school constraints, the hospital of the future is not necessarily a building, but new models of care delivery.

With support from:






It’s a scene “The Jetsons” might have portrayed: A patient scheduled for surgery checks into the hospital by scanning a QR code with her smartphone, then is digitally led to her room. There, a smart TV welcomes her and orients her to the room. Soon, a robot arrives, delivering the gown she’ll change into and the medication her physician requested that she take before the procedure. It will be an hour before she sees a human face.
This type of Rosey the Robot-style hospital encounter already exists in hospitals like Cedars-Sinai Medical Center in Los Angeles and Hancock Health in Greenfield, Indiana.1 But reaching this future state presents unique challenges in some older facilities.

“We don’t have the infrastructure from a true ‘size of the door’ perspective to fit some of these robots into our platform,” said Cecelia Moore, MHA, CPA, CFO and treasurer for Vanderbilt University Medical Center in Nashville, Tennessee.
“I think we’ll get there, but I do think it’s going to take some retrofitting and building to be able to use those types of tools. If you’ve got an older facility, that’s going to be tough to do,” she said. “We went to use a little piece of technology, and we thought it was going to be great, and then we realized: ‘Oh, yeah, our infrastructure won’t support it right now.’ That was a real eye-opener for us.”
Across the industry, the pace of change in healthcare is putting pressure on healthcare leaders to develop a future-forward point of view about what’s next and what’s needed.
Nearly nine out of 10 healthcare finance professionals surveyed by HFMA believe technological innovation will be one of the forces that will reshape healthcare the fastest. Also a driving force: the need to make healthcare more affordable and reduce costs of care (66%). Regulatory and policy changes ranked third at nearly 57%.
Survey Question
Tech innovation and affordability concerns drive push toward healthcare transformation
In your view, what are the forces that will reshape healthcare the fastest?
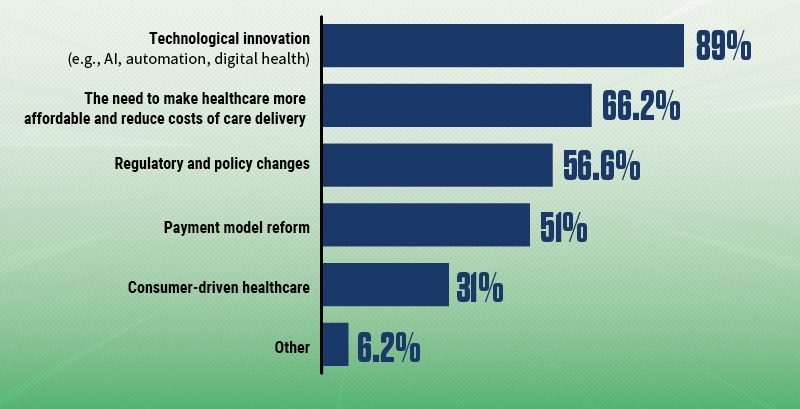
Note: Survey participants could select more than one response.
Source: HFMA survey of healthcare finance professionals, Jan. 27-Feb. 16, 2026
About 44% of healthcare finance professionals also predict “significantly more” care will be provided outside hospital walls within 10 years, while nearly 37% say it will at least be “moderately more.”
But as the baseline of what’s possible in healthcare changes rapidly, there are also signs that the industry is clinging to an old model of healthcare delivery.
A recent analysis indicates that health systems are investing a record amount on new hospital construction, far more than on outpatient facilities like ambulatory surgery centers.2 And while an Oliver Wyman report projects that annual healthcare spending could rise to $9 trillion in the next decade unless the industry recommits to affordability, healthcare leaders are concerned their organizations aren’t prepared to meet the moment.3
Among HFMA survey respondents, one out of four believe leaders are somewhat or very unprepared to lead the hospital of the future.
“We’re at a crossroads in healthcare,” said Jeremy Friese, MD, founder and CEO of Humata Health, a prior authorization-focused tech company.
“For the first time ever, nobody is financially on solid footing,” he said. “Historically, it’s been a situation where either the providers were OK or the payers were OK, but it was like a zero-sum game, and you were just moving money around. We’re now at the first time ever where our economy essentially revolves around healthcare, and healthcare finances are not sustainable, period. If it doesn’t change in 10 years, we’ll have a major problem.”
Survey Question
Majority have confidence in C-suite’s ability to lead the hospital of the future
How prepared do you believe senior healthcare leaders are to lead the hospital of the future?
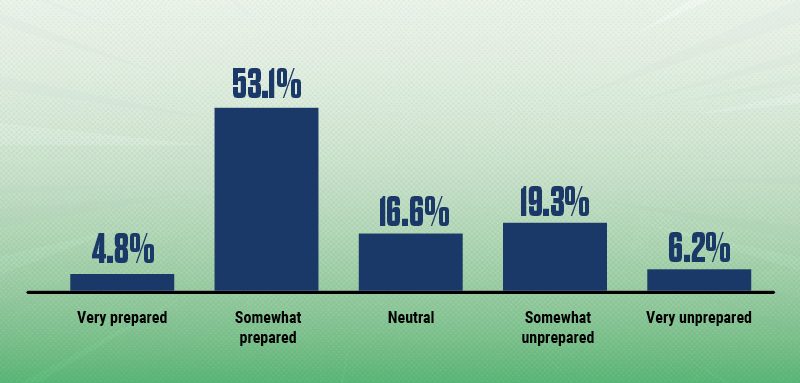
Source: HFMA survey of healthcare finance professionals, Jan. 27-Feb. 16, 2026
The growing imperative for a digital-first delivery model
For healthcare leaders, one challenge of predicting what the hospital of the future will look like is the difficulty of letting go of the current model of care, according to David Nace, MD, HFMA Healthcare Leadership Council member and chief medical officer for Innovaccer, which leverages data to support value-based care.

“People don’t like change, but impermanence is just a fact of life, and it’s speeding up when it comes to the future of care delivery,” Nace said.
He believes the hospital of the future will be “a digital-first, patient-centric ecosystem that extends care beyond physical walls into homes, utilizing data-driven, predictive insights.”
In such a world, hospitals with physical walls will still be required, but their role, design and function will undergo transformation, he said. And those walls may need to be highly adaptable.
“There’s a lot of discussion around buildings needing to have prefabricated, removable, flexible walls so the configuration of a room could be shifted quickly depending on what’s needed in the moment,” Nace said.
Sarah Hatchett, senior vice president, CIO for Cleveland Clinic, said accelerated advancements in healthcare technology, including AI, are prompting leaders to carefully consider their facility needs in a world of tech-enabled care.
“We’re talking a lot about how the building itself needs to be designed, anticipating some of these scaling-type technologies,” Hatchett said. “How do we create buildings that are more flexible — for example, with walls that can be moved, these sorts of things, because you simply can’t know exactly what it is that will be needed in the future?
“We have to be able to start building physical plants that can flex up and down depending on how this technology starts to show up. We’re already seeing that happen today.”
Survey Response
On whether the United States will be closer to an affordable and sustainable healthcare system by 2036:
“Baby steps closer. This is a highly complex problem being regulated by people with limited understanding and personal/political agendas that are at odds with reform.”
Hospital of the Future survey respondent
Hospitals could play a reduced role in a more diversified ecosystem
For healthcare leaders, gauging the hospital of the future’s role in the healthcare ecosystem — and preparing their organizations for this future state — also has become a leadership imperative.
Among healthcare finance professionals surveyed by HFMA, nearly half (about 47%) envision that the hospital of the future will primarily provide care for people with advanced and critical care needs. About one in five believe hospitals will remain the acute care hub of a health system.
When Nick Barcellona, CFO for WVU Medicine, a regional health system with 25 hospitals across West Virginia, Ohio, Pennsylvania and Maryland, considers whether the hospital of the future will be a place or more of a platform, he envisions it could be “a little of both.”
He expects hospitals will offer a higher concentration of acute services, with lower acuity care delivered via telemedicine or in outpatient or ambulatory settings or the home.
“I think technology is going to look dramatically different, and I think we’re kidding ourselves if we think we know what that’s going to look like in 10 years,” said Barcellona, whose undergraduate degree is in computer engineering.
“I do think we will be required to utilize technology in a lot of different ways in the hospital of the future, specifically when I think about the talent pipeline and the shortage of physicians and nurses and other care providers,” he said. “The advent of technology and how we utilize that to deliver care is going to dramatically transform the way we interact with our patients.
“That said, I do also think the four walls of the hospital are still going to exist. I think we are always going to need emergency departments and intensive care units or suites and, essentially, quaternary care, tertiary care. People are still going to get sick. They’re still going to need complicated heart surgery, complicated cancer care, transplants, emergent care, and I think all of those things are still going to be done within the four walls of a hospital.”
In Friese’s view, hospitals can either become a convener of care — sick care and wellness care — or their role in the healthcare ecosystem can become dramatically smaller.
“The kind of leaders that embrace the platform approach will be the leaders that drive scalable hospital systems that deliver on the promise of well care and sick care,”
Friese said.
“We need to move from a brick-and-mortar sick care model toward plotting an interconnected platform of technologies that deliver well care and sick care focused on the patient, focused on customer service and patient well-being,” he said.
Survey Question
Opinions vary on what the hospital of the future could look like
When you think about the hospital of the future 10 years from now, do you envision that the hospital will be a place, or more of a platform?
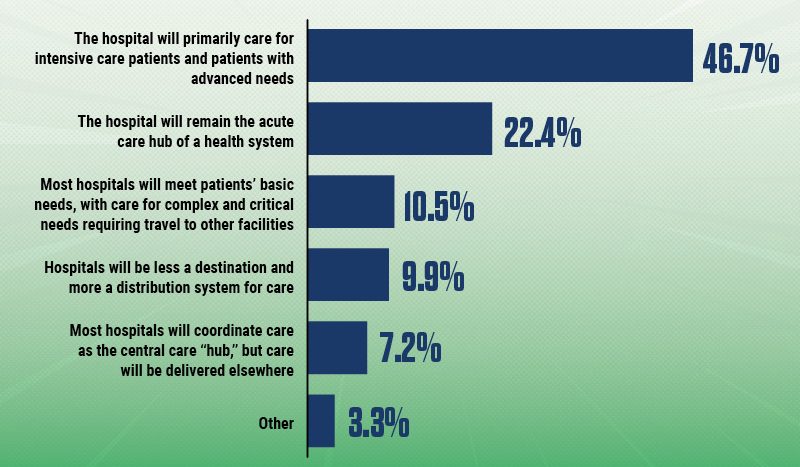
Source: HFMA survey of healthcare finance professionals, Jan. 27-Feb. 16, 2026
Adopting AI and reducing waste
As healthcare leaders think about the future of care and care delivery, some changes in approach already are occurring with advancements in technology, especially AI.
“With the introduction of AI, we’re starting to see shifting in that hospital care model from reactive to more predictive in nature,” said Hatchett of Cleveland Clinic. “Automation and AI are going to help us with coordinating and monitoring decision support around that care. So, for example, insights are going to be surfaced to clinicians as part of their workflow.”
As technology is deployed at scale throughout the care ecosystem, Hatchett anticipates this will amplify the care delivery model, but also make it “a lot less human dependent.”
There is also increased focus on the need to remove administrative waste from the U.S. healthcare system. By 2035, PwC anticipates that $1 trillion in annual healthcare spending will be redirected from administrative overhead and brick-and-mortar facilities toward next-generation care.4 According to PwC, such a move could elevate healthcare from a model where costs are breaking the system toward a care delivery model that:
- Strengthens the ability to anticipate disease before symptoms emerge
- Supports continuous, personalized and predictive care that evolves with the individual
- Empowers tech-savvy consumers to pay out of pocket for care innovations that might be incorporated by commercial health plans and government payers
- Replaces an infrastructure-heavy delivery model with virtual command centers and consumer-facing technologies that allow consumers to receive care when and where they need it and empower clinicians to focus on complex care interventions

The vision of a system where administrative strain and waste give way to more personalized, connected care is within grasp, said Darshak Sanghavi, MD, chief medical officer for Machinify, which focuses on removing waste related to healthcare payment.
Moreover, he believes it can be achieved within the next decade.
“For too long, we have dramatically added complexity to the areas of healthcare that, in fact, have very little to do with the actual patient care system,” Sanghavi said.
“I’m a pediatric cardiologist, and I still take care of children with complex heart defects and take care of children in primary care as well,” he said. “The administrative load in healthcare is already getting a little better, honestly. I think about the amount of time I used to spend trying to find a chest X-ray, or when I did an echocardiogram, sending it via a VCR videotape — and this was just 10 or 15 years ago. Now, it’s all digital. So already, technology is making that better.”
At Corewell Health, a Michigan-based not-for-profit health system that operates 21 hospitals, efforts to strip administrative waste from advanced primary care have significantly improved access to care. That, in turn, has decreased emergency department visits and hospitalizations while improving patient satisfaction scores.
For example, in 2023, Corewell Health launched an inboxologist program where a registered nurse initially reviews all incoming messages in a physician’s inbox. The nurse addresses messages that can be managed independently and then forwards the remaining messages to the advanced practice provider, or inboxologist, who handles the majority of the messages. Only messages that specifically require a physician’s expertise are routed to the physician, and they are carefully teed up so that the physician doesn’t spend extra time searching through the chart for relevant information.

“Prior to Covid, our primary care providers were getting about 600,000 messages a year via MyChart. After Covid, that increased to 3 million,” said Rima Shah, MD, senior vice president and chief medical officer for Corewell Health. “The inboxologist was created as a way to reduce their inbox burden.”
Corewell Health hired 30 inboxologists. The results were dramatic.
“We decreased the physician’s in-basket by 50%. There has never been anything I have tried that has decreased the in-basket by 50%. That’s a huge impact,” Shah said. “By doing that, we were able to add 20,000 more patient visits in eight months.”
Corewell Health also reimagined how patients under full-risk arrangements are connected with the care they need.
“In a traditional primary care clinic, let’s say you have a patient who calls and says, ‘I’m on my way to my visit today, but I’ve got a flat tire, so I’m going to need to reschedule.’ If you’re in a normal fee-for-service clinic, the receptionist would likely say, ‘OK, we’ll get you in as soon as we can,’” said Matt Cox, FHFMA, CPA, executive vice president, CFO for Corewell Health and 2026-27 HFMA Chair.

“When you’re in one of our advanced primary care clinics, what we would say is, ‘Wait there. We’re going to come and pick you up, and we’re going to get someone to fix your tire. It’s really important that you get in today because we’re managing your diabetes, and you need to meet with your physician.’”
Similarly, when these patients have health concerns outside of their appointments, they are connected with a nurse who assesses their needs, offers care advice and determines whether they should come into the office for care.
“It’s really about focusing on the patients who need care the most and helping them be seen when they need to be seen,” Cox said. “We keep slots open so they can get in right away if something has changed with their health.”
Ultimately, the future of primary care will be a model that shifts from visit- and physician-based care toward team-based, technology-enabled, continuous care of patients, Shah said.
That’s an area where AI could make an impact.
“We’ve got a massive labor problem in healthcare, and we need to solve that with technology,” said Friese of Humata Health. “We aren’t going to crank out more doctors, nurses and techs and revenue cycle staff. We’re just not. And so we have to solve those problems with robots and software. The manufacturing industry has been doing this with both AI and robots. We need to embrace some of that.”
Survey Question
Acute care hub or system-level command center?
What do you view as the hospital’s primary role in the future healthcare ecosystem?
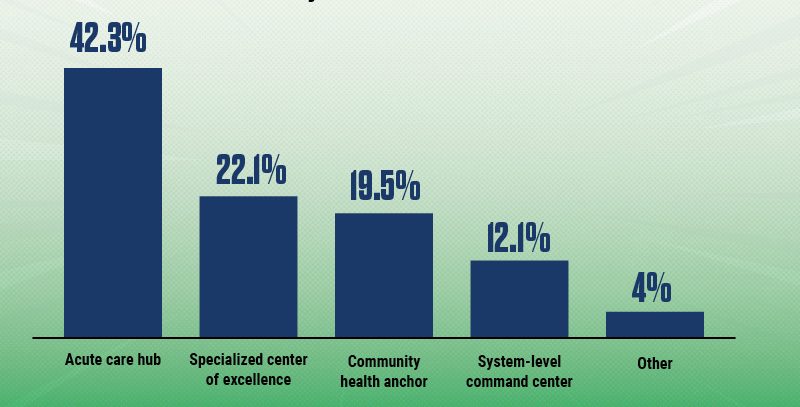
Source: HFMA survey of healthcare finance professionals, Jan. 27-Feb. 16, 2026
Hospitals of the future start with imagination, courage
In an episode of “The Jetsons,” the Peek-a-Boo Prober — a talking pill that gave George Jetson’s doctor a view of his esophagus and stomach in seconds — was decades ahead of its time.5 Today, that invention is awfully similar to a capsule endoscopy camera.6 But even in this futuristic world, a human doctor still directed the care experience and assessed the results.
“The reality is, we’re still going to need good leaders. We’re going to need good caregivers. We’re going to need good problem solvers, because the AI is not perfect, either,” said Barcellona of WVU Medicine. “And we’re going to need someone who can help navigate and bridge the gap between our care delivery and what some of these tools are doing on the back end.”
For CFOs, it’s a call to embrace the technologies that are advancing care and operations, but in a controlled way, he said.
“I think we have to be out there listening and seeing what other sectors are doing and learning and then bringing that back to our teams and allowing those teams to be creative,” he said. “You need to continue to develop and continue to learn, and that skill is transferrable regardless of the tool or technology.”
Staying curious is just as important, Cox said.
“People who are curious are going to be willing to experiment and try new things, and they’re going to take risks,” Cox said. “And I think all those things are necessary for the future.”
4 ways to prepare for the hospital of the future

- Become well-versed in what AI can do — and what it can’t. “I think we all need to be more technology-savvy so that we’re not just asking the question, ‘What’s the ROI?’ but also, ‘Are we going to do a proof of concept? How quickly? Does this allow us to provide higher quality care? Does it allow us to take care of a bigger population with the same hard footprint?’” said Cecelia Moore, MHA, CPA, CFO and treasurer for Vanderbilt University Medical Center in Nashville, Tennessee.
- Strive to be a visionary thinker. “In general, when people are trying to advance healthcare and health technologies, there is a tendency to want to do something that feels familiar to you,” said Darshak Sanghavi, MD, chief medical officer for Machinify. “Oftentimes, hospitals — even when they’re nonprofit — are incentivized by quarterly margins. It’s more difficult to picture, ‘What does a patient experience look like in three years, five years or 10 years?’”
- Take the time to fully understand an AI tool’s capabilities before pushing it out to your team. “If the person who’s using it doesn’t find value in what’s there, they’re probably going to quickly forget about it and say, ‘That’s not for me,’” said Sarah Hatchett, senior vice president and CIO for Cleveland Clinic. “You only get one shot with folks as far as their ability to trust and adopt the AI tools. If you try to push it too early and the product is not quite ready yet, you may miss an opportunity to improve the product.”
- Lean into storytelling in communicating your vision for the future. “The number one skill for leaders in an AI world is storytelling,” said Jeremy Friese, MD, founder and CEO of Humata Health. “Leaders who are able to tell a story in a way that helps people understand and move in a direction of adopting advanced technologies will be the ones who thrive, and their organizations will be the ones that thrive.”
Footnotes
1. “Robots help nurses get the job done – with smiles and beeps,” Cedars Sinai Newsroom, YouTube, Dec. 8, 2021; and Woods, N., “Hancock Health rolls out first-of-its-kind robot in hospital to boost efficiency,” WRTV Indianapolis, YouTube, Oct. 31, 2025.
2. Daly, R., “FastFinance: Hospital building surge; AI-coding study pushback,” HFMA FastFinance Podcast, March 17, 2026.
3. Hoban, C., Strull, R., Flignor, M., and Kreutzer, Z., “Healthcare’s growing affordability crisis,” Oliver Wyman, January 2025.
4. PwC, From breaking point to breakthrough: The $1 trillion opportunity to reinvent healthcare, Sept. 17, 2025.
5. “Test Pilot,” Season one of “The Jetsons,” Dec. 30, 1962.
6. Mayo Clinic staff, “Capsule endoscopy,” Mayo Clinic, Oct. 30, 2025.
PHOTOS BY MARSHALL CLARKE; COVER ILLUSTRATION OF AN IMAGE BY MARSHALL CLARKE
This report was developed with generous support from its sponsors.
In a supplement to the report:
- Cheryl Cruver, AGS Health’s president, U.S. markets and chief commercial officer, focused on patient care and access.
- Ben Beadle-Ryby, AKASA’s chief revenue officer, said the hospital of the future will need imagination, courage and new operating models.
- Seth Cohen, Cedar’s president, discussed how the hospital of the future will be defined by how it delivers care and how it gets paid for it.
- Thea Campbell, Solventum’s business director, revenue cycle/revenue integrity centered on revenue cycle operations in a digital-first ecosystem.
- Kyle Fetter, Xifin’s chief financial officer and Sanjay Kumar, Xifin’s chief technology officer explained technology is foundational to operate hospitals.





