Hospitals predict significant shifts in payer mix, revenue cycle operations post pandemic
Although the United States is still in the thick of its COVID-19 response, many healthcare leaders are starting to anticipate several challenges and opportunities that could emerge once the pandemic wanes. To gain a better understanding of healthcare executives’ perspectives on the post-pandemic future, the Healthcare Financial Management Association (HFMA) surveyed 151 healthcare leaders, asking about their projections for five areas, including payer mix, consumer and employee experience strategies, revenue cycle IT budgets, electronic health record (EHR) satisfaction and price transparency preparedness. Participants included C-level executives as well as vice presidents and directors of finance across hospitals and health systems. Through its Center for Health Insights, Guidehouse analyzed the research conducted by HFMA, and the following sections discuss key takeaways.
Most leaders anticipate major shifts in payer mix
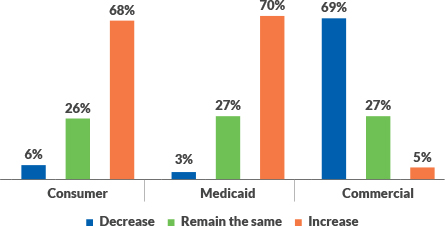
Approximately 70% of hospital and health system leaders are preparing for an increase in self-pay consumers and Medicaid beneficiaries post-COVID-19. Around this same number foresee a decrease in commercial reimbursement. These predictions stem from the volatile unemployment picture, which is causing a significant number of people to lose access to their employer-sponsored health plans. Without these plans, an individual may change to self-pay status or have to seek Medicaid benefits depending on their economic situation.
“With health system margins primarily driven by elective services, the pandemic is gravely impacting provider revenue streams and payer mix,” says Timothy E. Kinney, Guidehouse partner. “As our economy labors post-pandemic, insured patients will struggle to shoulder greater cost sharing through high-deductible plans coupled with volatile unemployment rates. Healthcare leaders need to closely evaluate their payer mix and develop winning consumer experience strategies to overcome a slow recovery in patient volumes and an uptick in self-pay and Medicaid enrollees.”
Providers are ramping up consumer engagement strategies
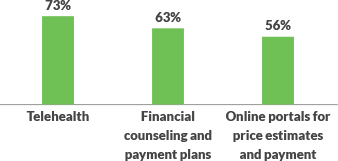
During this time, hospitals and health systems have amplified patient engagement, pursuing new strategies and expanding on existing ones. Notably, 92% of executives say their organizations have increased telehealth, with 73% using it to better engage patients and address consumer responsibility. Leaders also indicate their organizations are expanding financial counseling and payment plans (63%) in response to patients’ changing financial circumstances, and more than half (56%) are using online portals to deliver price estimates and receive payments.
“Hospitals and health systems have always prioritized meeting patient needs, but those needs and how to best address them are changing as the pandemic endures,” says Rick Gundling, senior vice president, healthcare financial practices for HFMA. “Going forward, organizations have to be flexible, continuously looking for effective strategies that can meet patients where they are and engage them in care and payment.”
Changes in the coming year
Revenue cycle IT budgets are expected to decrease
Hospital and health system leaders are expecting a decline in RCM IT budgets over the next 12 months, which represents a marked change from pre-pandemic thinking. In 2019, 69% of survey respondents anticipated their IT budgets would grow and only 5% felt they would decrease. This year, only 35% state their organization’s IT budgets will increase and nearly one-third (27%) think they will go down.
Organizations still need to find ways to decrease revenue cycle costs and increase economies of scale. This work is important at any time, but it is especially critical in the current environment. Healthcare leaders are looking to external entities to help, mentioning vendor partnerships (37%) and outsourcing arrangements (32%) most often when asked about potential cost-containment strategies.
Even though overall technology investments may go down, the idea of using technology to keep costs in check is still appealing. Fully 27% of executives predict they will use advanced health IT, including predictive analytics and robotic process automation, to reduce costs.
“As the revenue cycle workforce goes remote and budgets tighten, health system leaders are evaluating strategic investments in vendor partnerships and outsourced services,” says Mary Beth Briscoe, FHFMA, FACHE, CPA, MBA, CMRP, a senior advisor to Guidehouse who formerly served as a health system CFO and HFMA national board chair. “While digital technologies will be a necessity post-COVID-19, they must be methodically selected to ensure they are unlocking long-term performance improvement opportunities.”
Consumer engagement strategies underway
EHRs are becoming more accepted, but challenges remain
As EHRs continue to mature, providers are seeing greater benefits from their capabilities. More than 40% say that the benefits of EHR adoption outweigh the challenges, and this is up from 31% a year ago. Almost 70% of providers indicate they appropriately use available EHR functions, and more than half (55%) quickly adapt to new functionality releases. Despite the more positive view of EHRs, there are still some hurdles to overcome. For example, only one-in-five executives cite a seamless transition to telehealth within the EHR, which has been an essential component in engaging with patients during the pandemic.
“COVID-19 has demonstrated the reliance on the robust use of EHRs, and organizations are seeing many benefits from these tools,” says Gundling. “That said, there is much more work to be done, and organizations should use this unexpected opportunity to conduct a performance assessment and see where improvements could be made to drive better value.”
Executives are concerned with price transparency compliance
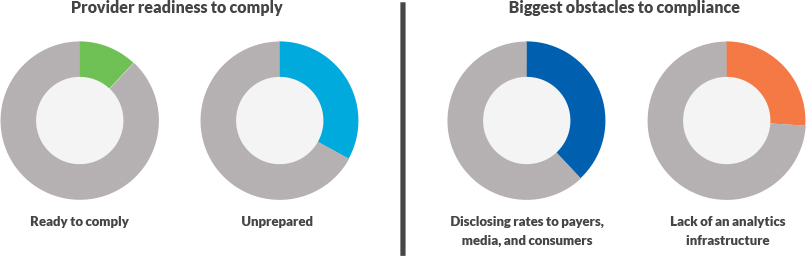
The hospital price transparency rule from the Centers for Medicare & Medicaid Services (CMS) is scheduled to go into effect on January 1, 2021. However, only 12% of healthcare leaders feel their organizations are ready to comply, with one-third suggesting they are unprepared. Concerns about disclosing rates to payers, media, and consumers (38%) and lack of an analytics infrastructure (26%) are cited as the biggest obstacles for compliance. As the year closes, hospitals and health systems will need to accelerate their efforts in this area to meet the needs of patients as well as the approaching deadline.
Readiness for price transparency
About Guidehouse
Guidehouse is a leading global provider of consulting services to the public and commercial markets with broad capabilities in management, technology, and risk consulting. We help clients address their toughest challenges and navigate significant regulatory pressures with a focus on transformational change, business resiliency, and technology-driven innovation. Across a range of advisory, consulting, outsourcing, and digital services, we create scalable, innovative solutions that prepare our clients for future growth and success. Headquartered in McLean, Va., the company has more than 8,000 professionals in over 50 locations globally. Guidehouse is a Veritas Capital portfolio company, led by seasoned professionals with proven and diverse expertise in traditional and emerging technologies, markets, and agenda-setting issues driving national and global economies. For more information, please visit: www.guidehouse.com.






