Cost transformation requires accountability
Moderate goals and moderate success in achieving them will not produce transformative outcomes.
A new report on performance improvement jointly released by Kaufman Hall/Axiom and HFMA indicates that hospitals and health systems continue to face stiff headwinds. Respondents to the survey that was the basis of the report’s findings cited flat or declining inpatient volumes and downward pressure on commercial insurance rates as the two most significant pressures on revenue. Nearly half the respondents (47%) cited rising salaries and wage inflation as the most significant pressure on expenses.
Without greater accountability, incumbent providers will struggle to compete
The pressures on hospitals and health systems will not abate. The flat or declining inpatient volumes noted by respondents are indicative of changes reshaping both healthcare delivery and healthcare business models. Growth is occurring outside the hospital wall’s in outpatient centers and retail locations.
Incumbent health systems face the prospect of increased competition from new market entrants that do not bear costs of providing acute inpatient care, nor the burdens of legacy assets, delivery models and culture. They often have significant reserves of capital at hand, either through private equity backing or the scale and resources of national competitors such as
CVS Health or Walmart. Many are experienced retail operators accustomed to competing on price.
Effective competition in a new, retail-focused healthcare business model will depend on the ability of incumbent providers to execute on strategies that radically reform their cost structure and enable them to compete on access, convenience and price. Yet signs of the ability to engage in this radical restructuring are not promising. While 96% of survey respondents indicate that their organization has targeted cost reduction goals, these goals represent 10% or less of current costs for 84% of respondents. And fewer than 1 in 4 respondents report that they have had success in accomplishing “all” or “most” of their cost transformation goals to date.
In short, most organizations have set moderate cost transformation goals and have had moderate success in achieving them. This will not result in the transformative outcomes the current healthcare environment demands.
What is holding organizations back? The survey results show a three-way tie for the most significant impediments to achieving cost transformation goals. They include:
- A lack of good data and insight into costs and where savings opportunities exist
- Too many savings opportunities that are too politically sensitive to pursue
- A failure to hold leaders accountable to performance for cost transformation goals
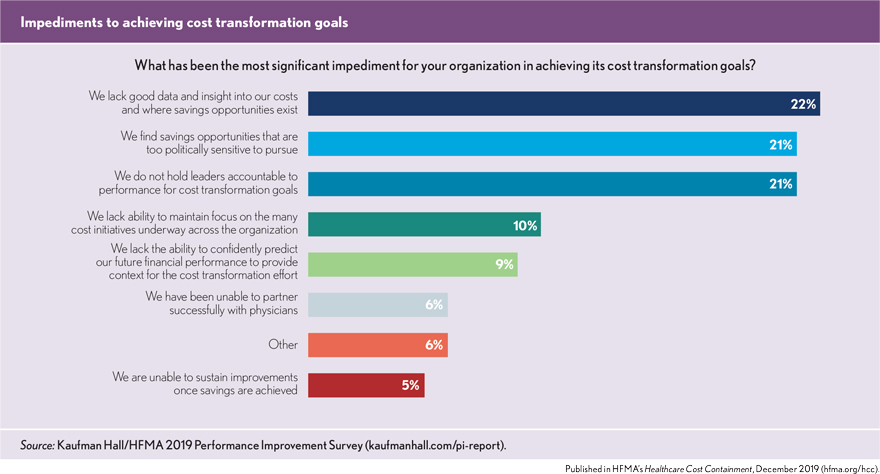
Two of these three impediments point to problems of accountability. Organizations simply cannot afford to maintain politically sensitive “sacred cows” that refuse to contribute to cost transformation goals. And they cannot fail to hold their leaders to account for the performance improvement goals they need to achieve.
Tactics and technology to improve accountability
Establishing greater accountability for achieving performance improvement goals is one of four strategies recommended in the report. Strategies, however, require implementation and execution. The following tactics and technology will help your organization improve accountability.
Build a culture of accountability. Accountability is ultimately a question of culture, defined by an organization’s leadership through their ability to unite around common goals and by stakeholders organization-wide through their willingness to take ownership of and responsibility for performance results. Culture change starts at the top, with an assessment of the composition, expertise and priorities of the organization’s board and executive team. A balanced board and executive team sets the stage for promoting collaboration between clinicians and finance and administrative professionals to ensure that cost transformation goals are achieved throughout the organization.
The next step in building a culture of accountability includes defining:
- Specific objectives to be met in each organizational dimension, based on an informed analysis of available opportunities
- Initiatives that are in place or will be implemented to meet the objectives
- Specific metrics that are appropriate to the performance of initiatives
- Specific agreed-upon milestones of progress and accountable individuals
These objectives, initiatives, metrics and milestones should not be issued as a mandate from the executive team. Instead, they should be developed collaboratively with leaders who will be accountable for the results to build their sense of ownership.
Establish a results management office. The often-used tactic of appointing a senior leader to serve as a performance improvement champion can backfire if others perceive that the champion is responsible for the success or failure of an initiative. A results management office (RMO) provides an alternative approach to accountability.
Specific responsibilities of an RMO can include project management or process redesign support; assistance with data integrity, analytics and reporting; change management; and facilitation of consistent, proactive and constituent-specific communications. Underperforming teams can seek out the RMO’s assistance voluntarily, but if a team is consistently underperforming, leadership has the option of requiring that the team accept help from the RMO. While the RMO and its staff help facilitate change, they are not directly accountable for results. Accountability remains with the team and its designated operational leaders.
Implement a strategy management solution. The work of performance improvement teams, RMO staff and executive leadership will be made easier by implementation of a strategy management solution that enables stakeholders throughout the organization to easily track progress on initiatives and drill down to investigate possible causes when progress stalls or begins falling behind targeted milestones.
Key elements of an effective solution include the following:
Structured and clean data. Performance improvement teams often will require data from multiple sources and systems. The strategy management solution should be able to accurately classify and standardize data from multiple sources to provide a “single source of truth” for the organization.
Timeliness. An effective solution should provide detailed and up-to-date information, regularly refreshed, to ensure initiatives stay on track.
Appropriateness. The strategy management solution should offer multiple views of data as appropriate for end users — from broad views across the organization for senior executives to more focused and deeper views into specific initiatives for operational teams.
Accessibility. All users should be able to easily drill down into reports to identify progress on goals, execution risks and accountable leaders.
Visualization. Data should be visualized in a way that enables users to quickly identify areas requiring attention through simple color-coding or directional arrows to indicate progress trends.
Facing the future
Accountability is just one key to future success in a rapidly changing healthcare environment, but without it, organizations will struggle to achieve their goals. Incumbent providers will be put to the test as the healthcare business model shifts to a price-competitive, retail-focused market. All stakeholders within the organization must understand what is at stake and their responsibilities for achieving results.






